pseudo-science
As I don’t live in the UK at present, I miss much of what the British papers report about so-called alternative medicine (SCAM). Therefore, I am a bit late to stumble over an article on the business activities of our Royals. It brought back into memory a little tiff I had with Prince Charles.
The article in the Express includes the following passage:

The UK’s first professor of complementary medicine, Edzard Ernst, dubbed the Duchy Originals detox tincture — which was being sold on the market at the time — “outright quackery”.
The product, called Duchy Herbals’ Detox Tincture, was advertised as a “natural aid to digestion and supports the body’s elimination processes” and a “food supplement to help eliminate toxins and aid digestion”.
The artichoke and dandelion mix cost £10 for a 50ml bottle.
Yet, Professor Ernst said Charles and his advisers seemed to be ignoring the science in favour of relying on “make-believe” and “superstition”, and said the suggestion that such products could remove bodily toxins was “implausible, unproven and dangerous”.
He noted: “Prince Charles thus financially exploits a gullible public in a time of financial hardship.”
This passage describes things accurately but not completely. What actually happened was this:
Unbeknown to me and with the help of some herbalists, Duchy Originals had developed the ‘detox tincture’ during a time when I was researching the evidence about ‘detox’. Eventually, my research was published as a review of the detox concept:
Background: The concept that alternative therapies can eliminate toxins and toxicants from the body, i.e. ‘alternative detox’ (AD) is popular.
Sources of data: Selected textbooks and articles on the subject of AD.
Areas of agreement: The principles of AD make no sense from a scientific perspective and there is no clinical evidence to support them.
Areas of controversy: The promotion of AD treatments provides income for some entrepreneurs but has the potential to cause harm to patients and consumers.
Growing points: In alternative medicine, simplistic but incorrect concepts such as AD abound. AREAS TIMELY FOR RESEARCH: All therapeutic claims should be scientifically tested before being advertised-and AD cannot be an exception.
When I was asked by a journalist what I thought about Charles’ new ‘detox tincture’, I told her that it was not supported by evidence which clearly makes it quackery. I also joked that Duchy Originals could thus be called ‘Dodgy Originals’. The result was this newspaper article and a subsequent media storm in the proverbial teacup.
At Exeter University, I had just fallen out of favor because of the ‘Smallwood Report’ and the complaint my involvement in it prompted by Charles’ first private secretary (full story in my memoir). After the ‘Dodgy Originals story’ had hit the papers, I was summoned ominously to my dean, Prof John Tooke, who probably had intended to give me a dressing down of major proportions. By the time we were able to meet, a few weeks later, the MHRA had already reprimanded Duchy Originals for misleading advertising which took most of the wind out of Tooke’s sail. The dressing down thus turned into something like “do you have to be so undiplomatic all the time?”.
Several months later, I was invited by the Science Media Centre, London, to give a lecture on the occasion of my retirement (Fiona Fox, the head of the SMC, had felt that, since my own University does not have the politeness to run a valedictory lecture for me, she will organize one for journalists). In that short lecture, I tried to summarize 19 years of research which inevitably meant briefly mentioning Charles and his foray into detox.
When I had finished, there were many questions from the journalists. Jenny Hope from the Daily Mail asked, “You mentioned snake-oil salesmen in your talk, and you also mentioned Prince Charles and his tinctures. Do you think that Prince Charles is a snake-oil salesman?” My answer was brief and to the point: “Yes“. The next day, this was all over the press. The Mail’s article was entitled ‘Charles? He’s just a snake-oil salesman: Professor attacks prince on ‘dodgy’ alternative remedies‘.
The advice of Tooke (who by then had left Exeter) to be more diplomatic had evidently not borne fruits (but the tinctures were discreetly taken off the market).
Diplomatic or honest?
This has been a question that I had to ask myself regularly during my 19 years at Exeter. For about 10 years, I had tried my best to walk the ‘diplomatic route’. When I realised that, in alternative medicine, the truth is much more important than diplomacy, I gradually changed … and despite all the hassle and hardship it brought me, I do not regret the decision.
I was reminded of an event that I had forgotten which, however, is so remarkable that we should remember it. It relates to nothing less than a homeopath’s attempt to save the world!
The homeopath’s name is Grace DaSilva-Hill. She has been a professional homeopath since 1997, with a clinic in Charing (Kent) and international on Zoom, Skype or WhatsApp video. She practises Sensation Homeopathy as refined by Drs Joshis (Mumbai), and Homeopathic Detox Therapy as developed by Dr Ton Jensen. She is also a practitioner of EFT-Tapping. In 2014, Grace very nearly saved the world with homeopathy – well, at least she gave it her very best try. Here is her original plan:

Yes, I agree, that’s hilarious! And it’s hilarious in more than one way:
- It is funnier than any comedian’s attempt to ridicule homeopathy.
- It is a highly effective approach by homeopaths to discrediting themselves.
But, at the same time, it is also worrying. Homeopaths are taken seriously by many influential people. Think of Prince Charles, for instance, or consider the way German homeopaths have convinced the government of Bavaria to invest in research into the question of how homeopathy can be used to reduce antibiotic resistance.
At the time, the formidable Andy Lewis on his QUACKOMETER commented as follows:
We might dismiss this as the fantasies of a small group of homeopaths. However, such thinking is widespread in homeopathic circles and has consequences. Grace is a well known homeopath in the UK, and in the past, has been a trustee and treasurer for the Ghana Homeopathy Project – an organisation that has been exporting this European form of quackery to West Africa. Grace believes that serious illnesses can be treated by a homeopath. For an article in the journal of the Alliance of Registered Homeoapths, Grace discusses treating such conditions as menigitis, malaria and stroke.
Homeopaths in West Africa have hit the news this week as a group tried to enter Liberia in order to use their spells on people with Ebola. The WHO fortunately tried not let them near any actual sick people and they have been kicking and screaming since. The Daily Mail’s rather dreadful article reported that they
“had used homeopathic treatments on patients, despite the instructions from health officials in the capital Monrovia not to do so. She said she had not felt the need to quarantine herself after returning to India but was monitoring her own condition for any signs of the disease.”
The homeopaths appear to have absolutely no understanding how dangerous and irresponsible their actions have been….
Homeopathy is stupid. Magical thinking. A nonsense. Anything goes. And whilst those doctors in the NHS who insist on spending public money on it without taking a responsible stand against the common and dangerous excesses, they can expect to remain under constant fire from those who think they are doing a great deal of harm.
Meanwhile, the public funding of homeopathy in England has stopped; France followed suit. Surely Grace’s invaluable help in these achievements needs to be acknowledged! If we regularly remind decision-makers and the general public of Grace’s attempt to save the world and similarly barmy things homeopaths are up to, perhaps the rest of the world will speed up the process of realizing the truth about homeopathy!?
The author of this study introduces the subject by stating that Reiki is a biofield energy therapy that focuses on optimizing the body’s natural healing abilities balancing the life force energy or qi/chi. Reiki has been shown to reduce stress, pain levels, help with depression/anxiety, increase relaxation, improve fatigue, and quality of life.
Despite the fact that the author seems to have no doubt about the effectiveness of Reiki, she decided single-handedly to conduct a study of it – well, not a real study but a ‘pilot study’:
In this pilot randomized, double-blinded, and placebo-controlled study, the effects of Reiki on heart rate, diastolic and systolic blood pressure, body temperature, and stress levels were explored in an effort to gain objective outcome measures and to understand the underlying physiological mechanisms of how Reiki may be having these therapeutic effects on subjective measures of stress, pain, relaxation, and depression/anxiety.
Forty-eight subjects were block-randomized into three groups (Reiki treatment, sham treatment, and no treatment). The changes in pre-and post-treatment measurements for each outcome measure were analyzed through analysis of variance (ANOVA) post hoc multiple comparison test, which found no statistically significant difference between any of the groups. The p-value for the comparison of Reiki and sham groups for heart rate was 0.053, which is very close to being significant and so, a definitive conclusion can not be made based on this pilot study alone.
The author concluded that a second study with a larger sample size is warranted to investigate this finding further and perhaps with additional outcome measures to look at other possible physiological mechanisms that may underlie the therapeutic effects of Reiki.
I have a few questions about this paper:
- If a researcher already knows that a treatment works, why do a study?
- If she nevertheless does a study, why a pilot that is not meant for evaluating effects but for testing the feasibility?
- Why does the author calculate effects instead of evaluating the feasibility of his project?
- Why does the author try to interpret a negative outcome as though it signifies an almost positive effect?
- Why did someone who knows how to do research at the Ohio Wesleyan University (the author’s affiliation) not give her some guidance?
- Why did the reviewers of this paper let it pass?
- Why does any journal publish such rubbish?
Oh, the embarrassment!
It’s a journal for which I once (a long time ago) served on the editorial board.
This study compared the effectiveness of two osteopathic manipulative techniques on clinical low back symptoms and trunk neuromuscular postural control in male workers with chronic low back pain (CLBP).
Ten male workers with CLBP were randomly allocated to two groups: high-velocity low-amplitude (HVLA) manipulation or muscle energy techniques (MET). Each group received one therapy per week for both techniques during 7 weeks of treatment.

Pain and function were measured by using the Numeric Pain-Rating Scale, the McGill Pain Questionnaire, and the Roland Morris Disability Questionnaire. The lumbar flexibility was assessed by Modified Schober Test. Electromyography (EMG) and force platform measurements were used for evaluation of trunk muscular activation and postural balance, respectively at three different times: baseline, post-intervention, and 15 days later.
Both techniques were effective (p < 0.01) in reducing pain with large clinical differences (-1.8 to -2.8) across immediate and after 15 days. However, no significant effect between groups and times was found for other variables, namely neuromuscular activation, and postural balance measures.
The authors concluded that both techniques (HVLA thrust manipulation and MET) were effective in reducing back pain immediately and 15 days later. Neither technique changed the trunk neuromuscular activation patterns nor postural balance in male workers with LBP.
There is, of course, another conclusion that fits the data just as well: both techniques were equally ineffective.
On 20 February 2021, I published on my blog a comment on a new study of an Ayurvedic remedy for COVID-19. The study was in my view suspect, and I expressed this as follows:
I have the following concerns or questions about this trial:
- Why do the authors call it a pilot study? A pilot study is merely for testing the feasibility of a trial design and is not meant to yield definitive efficacy results.
- The authors state that the patients were asymptomatic yet in the discussion they claim they were asymptomatic or mildly symptomatic.
- Some of the effect sizes reported here are extraordinary and seem almost too good to be true.
- The claim of no adverse effect is implausible; even placebos would cause perceived adverse effects in a percentage of patients.
- If the study is solid and withstands the scrutiny of the raw data, it is of huge relevance for public health. So, why did the authors publish it in PHYTOMEDICINE, a relatively minor and little-known journal?
An article in The Economic Times’ reported this:
Patanjali Ayurved released what it called the first “evidence-based” medicine for Covid-19 on Friday. It claimed it has been “recognised by the WHO (World Health Organization) as an ayurvedic medicine for corona”. Patanjali promoter, yoga guru Baba Ramdev, released a scientific research paper in this regard at the launch, presided over by Union health minister Harsh Vardhan and transport minister Nitin Gadkari. The Ayurveda products maker said it has received a certification from the Ayush ministry. “Coronil has received the Certificate of Pharmaceutical Product (CoPP) from the Ayush section of Central Drugs Standard Control Organisation (CDSCO) as per the WHO certification scheme,” it said in a statement. Under the CoPP, Coronil can be exported to 158 countries, the company said, adding that based on the presented data, the ministry has recognised Coronil as medicine for “supporting measure in Covid-19”.
Am I the only one who fears that something is not entirely kosher about the study? (This is an honest question, and I would be pleased to receive answers from my readers)
What happened next is most puzzling. After putting it on Facebook several times, I got banned for 72 hours from posting this article or anything else on Facebook. When this period had elapsed, I put the article in question again on Facebook. Subsequently, I was banned again but this time for 7 days. Facebook gave the following explanation:
You can’t post or comment for 7 days
This is because your previous posts didn’t follow our Community Standards.
No one else can see these posts.
1 Mar
Your post goes against our Community Standards on misinformation that could cause physical harm
We usually offer the chance to request a review, and follow up if we’ve gotten decisions wrong.
We have fewer reviewers available at the moment because of the coronavirus (COVID-19) outbreak. We’re trying hard to prioritise reviewing content with the most potential for harm.
This means that we may not be able to follow up with you, though your feedback helps us do better in the future.
Thank you for understanding.
On Twitter, the hype had begun even before its text was available. Priti Gandhi, for instance, tweeted:
Yet another feather in India’s cap!! 1st evidence-based, CoPP-WHO GMP certified medicine for Covid-19 released today. Congratulations to @yogrishiramdev ji, @Ach_Balkrishna ji & the team of scie…
EDZARDERNST.COM An RCT on the efficacy of ayurvedic treatment on asymptomatic COVID-19 patients
________________________________
As I did not feel I had broken any rules, I protested against the bans each time. When the 2nd ban was over, I posted my article yet again and, sure enough, yesterday I got banned again, this time for 30 days. Here is how they let me know:
You can’t post or comment for 30 days
This is because you previously posted something that didn’t follow our Community Standards.
This post goes against our standards on misinformation that could cause physical harm, so only you can see it.
Learn more about updates to our standards. On Twitter, the hype had begun even before its text was available. Priti Gandhi, for instance, tweeted: Yet another feather in India’s cap!! 1st evidence-based, CoPP-WHO GMP certified medicine for Covid-19 released today. Congratulations to @yogrishiramdev ji, @Ach_Balkrishna ji & the team of scie…
EDZARDERNST.COM An RCT on the efficacy of ayurvedic treatment on asymptomatic COVID-19 patients
As the reason for the ban always seems to be the Ayurvedic study, I suspect that some party interested in the product is behind the complaints that lead to the bans. I find it extraordinary that I can be banned repeatedly without having done anything wrong and without my objections ever being considered.
This study aimed to evaluate the effect of Traditional Chinese Medicine (TCM) on patients with gastric cancer following surgery and adjuvant chemotherapy in Taiwan. The cohort sampling data set was obtained from the Registry of Catastrophic Illness Patient Database, a research database of patients with severe illnesses from the National Health Insurance Research Database, Taiwan. Patients who had received a new diagnosis of gastric cancer and had undergone surgery were enrolled. the researchers matched TCM users and nonusers at a ratio of 1 : 3 based on the propensity score, and TCM users were also grouped into short-term and long-term users.
The number of TCM users and nonusers was 1701 and 5103 after applying the propensity score at a ratio of 1 : 3. Short-term users and long-term TCM users were independently associated with a decreased risk of death with HRs of 0.59 (95% confidence interval (CI), 0.55-0.65) and 0.41 (95% CI, 0.36-0.47), respectively, compared with TCM nonusers. The researchers also obtained similar results when they adjusted for covariates in the main model, as well as each of the additional listed covariates. They also observed similar HR trends in short-term users and long-term TCM users among men and women aged <65 years and ≥65 years. The most commonly prescribed single herb and herbal formula in our cohort were Hwang-Chyi (Radix Hedysari; 11.8%) and Xiang-Sha-Liu-Jun-Zi-Tang (15.5%), respectively.

The authors concluded that TCM use was associated with higher survival in patients with gastric cancer after surgery and adjuvant chemotherapy. TCM could be used as a complementary and alternative therapy in patients with gastric cancer after surgery and adjuvant chemotherapy.
This is an interesting study which seems well-done – except for one fatal mistake: even in the title, the authors imply a causal relationship between TCM and survival. Their conclusion has two sentences; the first one speaks correctly of an association. The second, however, not only implies causality but goes much further in suggesting that TCM should be used to prolong the life of patients. Yet, there are, of course, dozens of factors that could interfere with the findings or be the true cause of the observed outcome.
Anyone with a minimum of critical thinking ability should know that CORRELATION IS NOT CAUSATION; sadly, the authors of this study seem to be the exception.
Just as I read that the right-wing preacher Lance Wallnau once claimed he had cured Rush Limbaugh of his lung cancer – Limbaugh died yesterday of that cancer – I found this paper in the bizarre journal ‘EXPLORE’ reporting a much more successful (or should I say ‘tall’?) tale of healing by prayer.
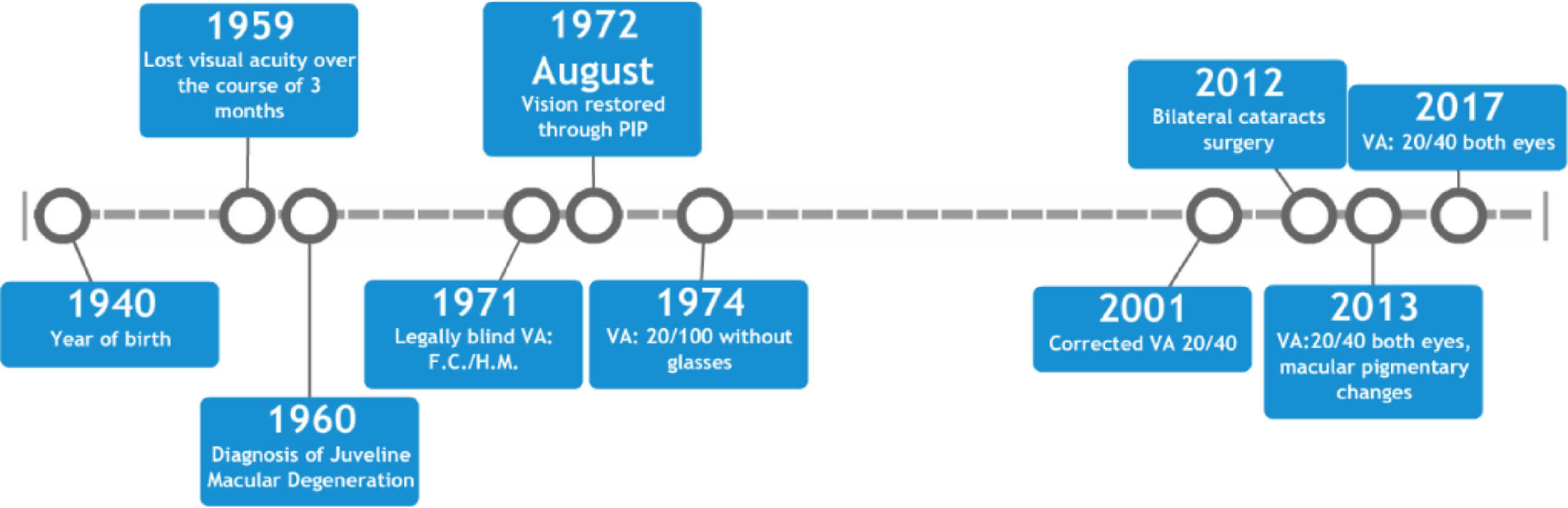
This case report describes an 18-year-old female who lost the majority of her central vision over the course of three months in 1959. Medical records from 1960 indicate visual acuities (VA) of less than 20/400 for both eyes corresponding to legal blindness. On fundus examination of the eye, there were dense yellowish-white areas of atrophy in each fovea and the individual was diagnosed with juvenile macular degeneration (JMD).
In 1971, another examination recorded her uncorrected VA as finger counting on the right and hand motion on the left. She was diagnosed with macular degeneration (MD) and declared legally blind. In 1972, having been blind for over 12 years, the patient reportedly regained her vision instantaneously after receiving proximal-intercessory-prayer (PIP). Subsequent medical records document repeated substantial improvement; including uncorrected VA of 20/100 in each eye in 1974 and corrected VAs of 20/30 to 20/40 were recorded from 2001 to 2017.
To date, her eyesight has remained intact for forty-seven years, according to the authors of this paper.
The course of these events is summarised in the graph below.
And here is what the patients was reported stating:
“What people need to understand is ‘I was blind’, totally blind and attended the School for the Blind. I read Braille and walked with a white cane. Never had I seen my husband or daughters face. I was blind when my husband prayed for me- then just like that- in a moment, after years of darkness I could see perfectly! It was miraculous! My daughter’s picture was on the dresser. I could see what my little girl and husband looked like, I could see the floor, the steps. Within seconds, my life had drastically changed. I could see, I could see!”
This report originates from the GLOBAL MEDICAL RESEARCH INSTITUTE. Their website claims that our mission is to investigate the effects of prayer in the resolution of conditions where the prognosis is typically poor, even with medical intervention. We are also developing randomized, controlled clinical trials of healing prayer effects.
Three questions came to my mind while reading all this:
- Are RCTs in prayer really needed? The believers already ‘know’ and will not trust the findings of the research, if they are not positive.
- Who do they try to convince the public with a case report that dates back 47 years?
- What do they think of Carl Sagan’s bon mot, ‘EXTRAORDINARY CLAIMS REQUIRE EXTRAORDINARY EVIDENCE’?
The drop in cases and deaths due to COVID-19 infections in India has been attributed to India’s national policy of using homeopathy. Early in the epidemic, the national “Ministry of AYUSH, recommended the use of Arsenic album 30 as preventive medicine against COVID-19. Its prophylactic use has been advised in states like Karnataka, Tamil Nadu, Kerala, and Maharashtra. The ‘OFFICIAL HOMEOPATHY RESOURCE’ is now claiming that homeopathy is the cause of the observed outcome:
And now the results of that policy and use are clear, even though skeptics and other scientists in the conventional paradigm are mystified as to why the drop is so dramatic. They know nothing about homeopathy and its history of successfully treating epidemics.
India has a population of 1 billion, 300 million people. Relative to this massive population the number of cases per day and especially the number of deaths per day are now exceptionally low. According to the Daily Mail:
“Scientists are trying to work out why coronavirus cases in India are falling when at one point it looked like the country might overtake the US as the worst-hit nation.
In September the country was reporting some 100,00 new cases per day, but that went into decline in October and is now sitting at around 10,000 per day – leaving experts struggling to explain why.”
END OF QUOTE
According to my sources, the number of daily new cases in India rose steadily to reach its maximum of almost 100000 new cases per day in mid-September. Thereafter, the figure fell in almost the same fashion as they had previously risen.

Currently, they have reached a plateau of about 13000 cases per day, and around 100 patients per day are reported to dies of COVID-19 every day. There are several possible contributors to these relatively positive outcomes:
- India has administered the Covid-19 vaccine to about 10 million people in one month since launching the world’s largest vaccination program on Jan. 16. However, this timing cannot explain the fall of cases before mid-January.
- The Indian government has attributed the dip in cases partly to mask-wearing, which is mandatory in public in India and violations can draw hefty fines.
- Large areas of India have reached herd immunity.
- Some of the various non-homeopathic remedies that have been recommended by the Ministry of AYUSH might be effective.
- There might be a host of other factors that I don’t know about.
- The figures coming out of India may not be reliable.
- The homeopathic remedy Arsenic album 30 might indeed be an effective preventative.
Which of these explanations are valid?
Most likely, it is not one but several working together. However, the hypothesis that homeopathy has anything to do with the course of the pandemic in India seems most unlikely. Apart from the fact that highly diluted homeopathic remedies are implausible and have not been shown to be effective, the timing of events is clearly against this explanation: if I am correctly informed, the homeopathic remedies were dished out months before the decline in cases started. In fact, simply going by the timing, one would need to assume that homeopathy led to the enormous increase before the remarkable drop.
Of course, it would be interesting to see the results of the homeopathy trials that allegedly started in India about 8 months ago. They could bring us closer to the truth. But somehow, I am not holding my breath.
The fact that the NHS England has stopped reimbursing homeopathy in 2018 is probably quite well known. France followed more recently, and then Germany too reported trouble for homeopaths on various levels. About two years ago, the manufacturer of homeopathic products, Hevert (Germany), threatened legal action against several German critics of homeopathy for expressing the fact that highly diluted homeopathic remedies do not work beyond placebo. Crucially, the medical associations of many regions in Germany have – one after the next – discontinued their training in and recognition of homeopathy.
Now similar difficulties are being felt also by Austrian homeopaths. In 2019, the Vienna medical school closed its course on homeopathy because students had filed a complaint about its unethical content. And recently, it was reported by the Austrian ‘Initiative für Wissenschaftliche Medizin‘ that at a secret webinar run by lobbyists in Vienna things were reported to no longer going well for homeopathy. Faced with such problems, the lobbyist, Dr. Jens Behnke, recommended in the above-mentioned secret webinar an alliance of all so-called alternative medicine (SCAM):
“…..and if we do not form this broad alliance now, in order to make appropriate professional PR and lobbying … then everything will fall apart….”
Now a union of pseudomedicine and politics is being forged with the aim of stopping the decline of quackery and paving the way for pseudomedicine in Austria. A resolution has been tabled in the Austrian parliament with the following demands:
- Institutionalising of the field of “Complementary Medicine” as “Integrative Medicine” in the academic education at all medical schools.
- Appropriate support for and funding of complementary medicine research, especially in the university sector.
- Establishment of a broad range of complementary medicine in the hospital sector, in outpatient but also inpatient healthcare.
- Promotion of active knowledge transfer in the area of integrative and complementary medicine within the Austrian medical profession.
- Securing of complementary diplomas by the Austrian Medical Association.
The motion was introduced by the Freedom Party (FPÖ, the Austrian far-right party) on 21.12.2020, forwarded to the Health Committee for consultation, and is now scheduled for consultation there. The application was introduced by the FPÖ-Nationalratsabgeordnete Mag. Gerhard Kaniak (Chairman of the Health Committee of Parliament, pharmacist), Peter Wurm (entrepreneur), Dr. Dagmar Belakowitsch (physician), and “other deputies”. It is supported by members of the “Initiative Complementary Medicine at Austrian Universities” of the Austrian Society for Homeopathic Medicine. The list of signatories of the motion reads like the “Who’s Who” of pseudo-medicine procedures in Austria – foremost homeopathy, but also anthroposophic medicine, ozone therapy, functional myo-diagnostics (= kinesiology), Ayurvedic medicine, orthomolecular medicine, TCM, etc. It almost goes without saying that it also includes Prof Michael Frass (a prominent member of THE ALTERNATIVE MEDICINE HALL OF FAME), who regular readers of my blog would have met several times before.
__________________________
Instead of a comment (other than I sincerely wish that reason prevails in Austria and the motion is going to be defeated), I think I will quote the concluding phrases from my memoir (which incidentally also covers my most turbulent time in Vienna):
When science is abused, hijacked, or distorted in order to serve political or ideological belief systems, ethical standards will inevitably slip. The resulting pseudoscience is a deceit perpetrated on the weak and the vulnerable. We owe it to ourselves, and to those who come after us, to stand up for the truth, no matter how much trouble this might bring.
Physicians who include so-called alternative medicine (SCAM) in their practice are thought to have an understanding of health and disease different from that of colleagues practicing conventional medicine. The aim of this study was to identify and compare the thoughts and concepts concerning infectious childhood diseases (measles, mumps, rubella, chickenpox, pertussis, and scarlet fever) of physicians practicing homeopathic, anthroposophic and conventional medicine.
This qualitative study used semistructured interviews. Participating physicians were either general practitioners or pediatricians. Data collection and analysis were guided by a grounded theory approach.
Eighteen physicians were interviewed (6 homeopathic, 6 anthroposophic, and 6 conventional). All physicians agreed that while many classic infectious childhood diseases such as measles, mumps, and rubella are rarely observed today, other diseases, such as chickenpox and scarlet fever, are still commonly diagnosed. All interviewed physicians vaccinated against childhood diseases.
- A core concern for physicians practicing conventional medicine was the risk of complications of the diseases. Therefore, it was considered essential for them to advise their patients to strictly follow the vaccination schedule.
- Homeopathic-oriented physicians viewed acute disease as a biological process necessary to strengthen health, fortify the immune system and increase resistance to chronic disease. They tended to treat infectious childhood diseases with homeopathic remedies and administered available vaccines as part of individual decision-making approaches with parents.
- For anthroposophic-oriented physicians, infectious childhood diseases were considered a crucial factor in the psychosocial growth of children. They tended to treat these diseases with anthroposophic medicine and underlined the importance of the family’s resources. Informing parents about the potential benefits and risks of vaccination was considered important.
All physicians agreed that parent-delivered loving care of a sick child could benefit the parent-child relationship. Additionally, all recognized that existing working conditions hindered parents from providing such care for longer durations of time.
The authors concluded that the interviewed physicians agreed that vaccines are an important aspect of modern pediatrics. They differed in their approach regarding when and what to vaccinate against. The different conceptual understandings of infectious childhood diseases influenced this decision-making. A survey with a larger sample would be needed to verify these observations.
The authors (members of a pro-SCAM research group) stress that the conventional physicians saw many risks in the natural course of classic childhood illnesses and appreciated vaccinations as providing relief for the child and family. By contrast, the physicians trained in homeopathy or anthroposophic medicine expected more prominent unknown risks because of vaccinations, due to suppression of the natural course of the disease. Different concepts of disease lead to differences in the perceptions of risk and the benefit of prevention measures. While prevention in medicine aims to eliminate classic childhood diseases, anthroposophic and homeopathic literature also describes positive aspects of undergoing these diseases for childhood development.
This paper thus provides intriguing insights into the bizarre thinking of doctors who practice homeopathy and anthroposophical medicine. The authors of the paper seem content with explaining and sometimes even justifying these beliefs, creeds, concepts, etc. They make no attempt to discuss the objective truths in these matters or to disclose the errors in the thought processes that underly homeopathy and anthroposophical medicine. They also tell us that ALL the interviewed physicians vaccinated children. They, however, fail to provide us with information on whether these doctors all recommend vaccinations for all patients against all the named infectious diseases. From much of previous research, we have good reasons to fear that their weird convictions often keep them from adhering strictly to the current immunization guidelines.