integrated medicine
As I am currently not in the UK, I (almost) missed the news about my ex-friend Michael Dixon (can you forgive me please, Michael?). I am going to report it here as published in the Independent without any comments of my own (which would inevitably have an after-taste of sour grapes):
The King has personally honoured his top medical team amid his treatment for cancer. Dr Michael Dixon, head of the Royal Medical Household, and Charles’s GP Dr Fiona Butler – otherwise known as the Apothecary to the King – have been recognised by Charles for their personal service to the monarch and the royal family…
Dr Dixon has been made a Commander of the Royal Victorian Order (CVO) and Dr Butler is now a Lieutenant of the Royal Victorian Order (LVO), with the accolades announced on the King’s official birthday. Awards of the Royal Victorian Order are in the King’s gift and are bestowed independently of Downing Street to people who have served the monarch or the royal family in a personal way. Dr Dixon and the King have known one another for decades, and he is responsible for overseeing the eminent members of the medical profession entrusted to care for the royal family.
His appointment as head of the Royal Medical Household following Charles’s accession drew criticism due to his outspoken support for alternative therapies, such as faith healing and herbalism. In 2023, Buckingham Palace set out the doctor’s beliefs to The Sunday Times, saying: “Dr Dixon does not believe homeopathy can cure cancer. His position is that complementary therapies can sit alongside conventional treatments, provided they are safe, appropriate and evidence-based.”
As the Prince of Wales, Charles was a passionate campaigner for integrated health, raising the profile of combining evidence-based, conventional medicine with an holistic approach to healthcare. Dr Dixon’s previous roles include a practising GP, a fellow of the Royal College of GPs, a fellow of the Royal College of Physicians, former chairman of NHS Alliance and the chairman of the College of Medicine…
_____________________
In case you are not familiar with the relevant history and wonder about the “ex-friendship”, there are numerous posts on this blog about Dixon that might explain. Alternatively, you could read my memoir, A Scientist in Wonderland.
On this blog, I have often been highly critical of integrative (or integrated) medicine (IM) – see, for instance:
- Integrative medicine: a satirical perspective
- A slightly different perspective on ‘INTEGRATIVE MEDICINE’
- Memorandum ‘INTEGRATIVE MEDICINE’
- Prince Charles’ opening speech at the ‘biggest ever’, ‘history-making’ integrative medicine conference
- The European Parliament’s Pathetic Attempt to Dabble in Integrative Medicine
- Integrative Medicine or Infiltrative Pseudoscience?
- Integrative Medicine: here is my slightly altered and much improved version
- More uncomfortable thoughts on ‘integrative medicine’
- The reality of ‘integrative medicine’ consists of little more than re-discoveries from conventional medicine, platitudes and outright nonsense
Recently, I began to realize that my previously critical stance has been largely due to the fact that 1) a plethora of definitions of IM exist causing endless confusion, 2) most, if not all, of the definitions of IM are vague and insufficient. At the same time, IM is making more and more inroads which makes it imprudent to ignore it.
I therefore decided it is time to change my view on IM and think more constructively. The first step on this new journey is to define IM in such a way that all interested parties can come on board. So, please allow me to present to you a definition of IM that is constructive and in the interest of progress:
IM is defined as the form of healthcare that employs the best available research to clinical care integrating evidence on all types of interventions with clinical expertise and patient values. By best available research, I mean clinically relevant (i.e., patient oriented) research that:
- establishes the efficacy and safety of all types of therapeutic, rehabilitative, or preventive healthcare strategies and
- seeks to understand the patient experience.
Healthcare practitioners who are dedicated to IM use their clinical skills and prior experience to identify each patient’s unique clinical situation, applying the evidence tailored to the individual’s risks versus benefits of potential interventions. Ultimately, the goal of IM is to support the patient by contextualising the evidence with their preferences, concerns, and expectations. This results in a process of shared decision making, in which the patient’s values, circumstances, and setting dictate the best care.
If applied appropriately, IM has the potential to be a great equaliser – striving for equitable care for patients in disparate parts of the world. Furthermore, IM can play a role in policy making; politicians are increasingly speaking to their use of research evidence to inform their decision making as a declaration of legitimacy. IM reflects the work of countless people who have improved the process of generating clinical evidence over several decades, and that it continues to evolve.
Developing the skills to practise IM requires access to evidence, opportunities to practise, and time. IM proponents strive to find novel ways to integrate evidence into personal holistic health in the best interest of our patients.
_________________________
I feel confident that this could create a basis for a fresh start in the dabate about the merits of IM. I for one am all for it!
In case some of my readers thought that the wording of my definition sounded somewhat familiar, I should perhaps tell you that it is my adaptation of the definition of evidence-based medicine (EBM) as published in ‘BMJ Best Practice‘.
What does that mean?
The points I am trying to make are the ones that I have tried to get across many times before:
- IM is a flawed, unethical, superflous and counter-productive concept.
- It is flawed because it is aimed at smuggling unproven or disproven treatments into routine care which can only render healthcare less safe and less effective.
- It is unethical because it cannot provide the best possible healthcare and thus is not in the best interest of patients.
- It is superflous because the aspects of IM that might seem valuable to proponents of so-called alternative medicine (SCAM) are already part of EBM.
- It is counter-productive because it distracts from the laudable efforts of EBM.
It has been reported that King Charles’ charity, formerly the Prince’s Foundation, is compelled to return £110,000 to the Indian government. The funds were earmarked for an NHS alternative medicine clinic championed by Charles, which never materialised. The proposed clinic was aimed at integrating Indian traditional medicine into the UK’s healthcare system.
But why did the plan fail?
The answer is simple: the National Health Service (NHS) did not approve it.
The history of the UK ‘Ayurvedic Centre of Excellence’ goes back several years. Here is an excerpt of my book ‘CHARLES, THE ALTERNATIVE KING‘ where I discuss it as one of Charles’ many pipe dreams in the realm of so-called alternative medicine (SCAM):
In 2018, India’s prime minister Narendra Modi paid a visit to the Science Museum in London where he inspected the ‘5000 Years of Science and Innovation’ exhibition. The event was hosted by Charles and included the announcement of new ‘Ayurvedic Centres of Excellence’, allegedly a ‘first-of-its-kind’ global network for evidence-based research on yoga and Ayurveda. The first centre was said to open in 2018 in London. Funding was to come partly from the Indian government and partly from private donors. The central remit of the new initiative was reported to be researching the effects of Ayurvedic medicine.
Dr Michael Dixon (yes, you may have met him several times before, e.g. here, here, or here) commented: “This is going to be the first Ayurvedic centre of excellence in the UK. We will be providing, on the NHS, patients with yoga, with demonstrations and education on healthy eating, Ayurvedic diets, and massage including reflexology and Indian head massage. And all this will be subject to a research project led by Westminster University, to find out whether the English population will take to yoga and these sorts of treatments. Whether they will be helped by it and finally whether it will reduce the call on NHS resources leading to less GP consultations, hospital admissions and operations.”
On its website, the College of Medicine and Integrated Health announced that a memorandum of understanding with India’s Ministry of Ayurveda, Yoga and Naturopathy, Unani, Siddha and Homoeopathy (AYUSH) had been signed “to create centres of excellence in the UK … Dr Michael Dixon agreed the joint venture to provide the UK centres, which will offer and research traditional Indian medicine… The Indian government will match private UK donations to fund the AYUSH centres in the UK”. In November 2019, the following press release by the president of India offered more details:
The Prince of Wales called on the President of India, Shri Ram Nath Kovind, at Rashtrapati Bhavan today (November 13, 2019).
Welcoming the Prince to India, the President congratulated him on his election as the head of the Commonwealth. He said that India considers the Commonwealth as an important grouping that voices the concerns of a large number of countries, including the Small Island Developing States.
The President said that India and the United Kingdom are natural partners bound by historical ties and shared values of democracy, rule of law and respect for multi-cultural society. As the world’s pre-eminent democracies, our two countries have much to contribute together to effectively address the many challenges faced by the world today.
The Prince planted a Champa sapling – plant native to the subcontinent which has several uses in Ayurveda – in the Herbal Garden of Rashtrapati Bhavan. He was taken around the garden and shown different plants that have medicinal properties. The Prince showed a keen interest in India’s alternative model of healthcare.
The President thanked the Prince of Wales for his support for Ayurveda research. The Prince of Wales Charitable Foundation and the All India Institute of Ayurveda signed an MOU during the visit of Prime Minister Narendra Modi to the UK in April 2018. Under the MOU, the All India Institute of Ayurveda and the College of Medicine, UK will be conducting clinical research on Depression, Anxiety and Fibromyalgia. They will also be undertaking training programme for the development of Standard Operating Protocol on “AYURYOGA” for UK Health professionals.
_________________________
END OF EXCERPT
Charles’ initiative, encompassing Ayurveda, yoga, naturopathy, and homeopathy, was intended to be a landmark project, with the Indian government contributing £110,000 to the King’s Foundation for its implementation. However, the NHS, responsible for St Charles Hospital, never endorsed the project. Despite initial talks, the proposed collaboration did not progress, and the clinic failed to materialise. According to the west London clinical commissioning group (CCG), which oversaw the hospital at the time, there was no official involvement, and discussions ceased in 2020.
Under charity law, funds designated for a specific project cannot be diverted without donor permission and regulatory approval. The King’s Foundation has acknowledged the need to return the remaining budget to the Indian government but has not disclosed when this decision was made or why the funds were not promptly returned.
The initiative faced opposition from the NHS, as a year before the clinic’s launch, NHS England’s CEO Simon Stevens had issued guidance discouraging the prescription of homeopathy and herbal remedies, citing their limited efficacy and misuse of NHS funds.
Despite the failed project, connections between key figures persist. Dr Michael Dixon played a significant role in finalising agreements with the Indian government. The King’s Foundation defended its actions, stating that due to the Covid-19 pandemic, the project shifted online, resulting in reduced costs. They claim to have contacted the Indian government for the return of unused funds, emphasising that the money remains in a restricted account.
As the controversy unfolds, questions arise about the intersections between alternative medicine advocacy, royal endorsements, and international collaborations within the context of public healthcare.
An article in the Daily Mail reported that the original plan proposed that Ayush treatments would be provided to patients, who would be referred by local GPs, at St Charles Hospital in Kensington. Isaac Mathai, who runs Soukya, a homeopathic yoga retreat in Bangalore which Charles and Camilla have visited, was an adviser to the project at St Charles Hospital.
The Indian government made a payment from the budget of the Ayush Ministry, which Mr Modi has used as a tool of diplomacy to promote Indian medicine and culture worldwide, to the King’s Foundation. It was proposed the charity would use its expertise to help set up the clinic. But the NHS at no point agreed to the plans.
A spokesman of the west London clinical commissioning group (CCG), which administered St Charles Hospital at the time, said: ‘Provision of homeopathy and herbal treatments were not considered as part of the project by the CCG. The aim of the project was to test the use of yoga and massage to support the overall health and wellbeing of patients with long-term conditions.’ A King’s Foundation spokesman added that the initial intention had been to deliver Indian traditional medicine at St Charles Hospital.
The current BMJ has an article entitled UK could have averted 240 000 deaths in 2010s if it matched other European nations. Here is its staring passage:
The UK has fallen far behind its international peers on a range of health outcomes and major policy reforms are required to reverse this, a report1 has concluded.
Analysts from the Institute for Public Policy Research (IPPR) calculated that there would have been 240 000 fewer deaths in the UK between 2010 and 2020 if the UK matched average avoidable mortality in comparable European nations.
The report says the UK’s poor outcomes are partly down to people’s inability to access healthcare in a timely manner, a problem that has intensified since the pandemic.
To tackle this, the progressive think tank has put forward a 10 point plan to shift the NHS from a sickness service to a prevention service. It says primary care should be placed at the heart of a “prevention first” NHS with a nationwide rollout of neighbourhood health hubs to deliver integrated health and care services in every local area…
INTEGRATED HEALTH?
Isn’t that the nonsense Charles III, Michael Dixon, THE COLLEGE OF MEDICINE AND INTEGRATED HEALTH and many others promote? The integrated health we discussed so often before, e.g.:
- Prince Charles becomes patron of the ‘College of Medicine and Integrated Health’
- The ‘All-Party Parliamentary Group for Integrated Healthcare (PGIH) have just published a new report – and it’s full of surprises
- Eurocam press release in favor of integrated medicine
- A new definition of ‘INTEGRATED MEDICINE’
- Integrative medicine: one of the most colossal deceptions in healthcare today
- INTEGRATED MEDICINE: a disservice to patients?
- Integrated/integrative medicine: a paradise for charlatans?
The UK ‘Integrated Medicine Alliance’ offers information sheets on all of the following treatments: Acupuncture, Alexander Technique, Aromatherapy, Herbal Medicine, Homeopathy, Hypnotherapy, Massage, ,Naturopathy, Reflexology, Reiki, Tai Chi, Yoga Therapy. The one on homeopathy, for example, tells us that “homeopathy … can be used for almost any condition either alone or in a complementary manner.” Is the BMJ thus promoting homeopathy and similar dubious treatments?
The answer is, of course, NO!
The BMJ supports INTEGRATED HEALTH as defined not by quacks but by real experts: “Integrated care, also known as integrated health, coordinated care, comprehensive care, seamless care, or transmural care, is a worldwide trend in health care reforms and new organizational arrangements focusing on more coordinated and integrated forms of care provision. Integrated care may be seen as a response to the fragmented delivery of health and social services being an acknowledged problem in many health systems.”
I have often wondered why quacks use established terms, give it a different meaning and use it for confusing the public. I suppose the answer is embarrassingly simple: they thrive on confusion, want to hide the fact that they have no convincing arguments of their own, and like to use the established terminology of others in order to push their agenda and maximize their benefits.
Vaccine hesitancy has become a threat to public health, especially as it is a phenomenon that has also been observed among healthcare professionals. In this study, an international team of researchers analyzed the relationship between endorsement of so-called alternative medicine (SCAM) and vaccination attitudes and behaviors among healthcare professionals, using a cross-sectional sample of physicians with vaccination responsibilities from four European countries: Germany, Finland, Portugal, and France (total N = 2,787).
The results suggest that, in all the participating countries, SCAM endorsement is associated with lower frequency of vaccine recommendation, lower self-vaccination rates, and being more open to patients delaying vaccination, with these relationships being mediated by distrust in vaccines. A latent profile analysis revealed that a profile characterized by higher-than-average SCAM endorsement and lower-than-average confidence and recommendation of vaccines occurs, to some degree, among 19% of the total sample, although these percentages varied from one country to another: 23.72% in Germany, 17.83% in France, 9.77% in Finland, and 5.86% in Portugal.
The authors concluded that these results constitute a call to consider health care professionals’ attitudes toward SCAM as a factor that could hinder the implementation of immunization campaigns.
In my view, this is a very important paper. It shows what we on this blog have discussed often before: there is an association between SCAM and vaccination hesitancy. The big question is: what is the nature of this association. There are several possibilities:
- It could be coincidental. I think this is most unlikely; too many entirely different investigations have shown a link.
- It could mean that people start endorsing SCAM because they are critical about vaccination.
- It could be that people are critical about vaccination because they are proponents of SCAM.
- Finally, it could be that some people have a mind-set that renders them simultaneously hesitant about vaccination and fans of SCAM.
This study, like most of the other investigationson this subject, was not desighned to find out which possibility is most likely. I suspect that the latter two explanations apply both to some extend. The authors of this study argue that that, “from a theoretical point of view, this situation may be explicable by reasons that are both implicit (i.e., CAM would fit better with certain worldviews and ideological standpoints that conflict with the epistemology and values that underlies scientific knowledge) and explicit (i.e., some CAM techniques are doctrinally opposed to the use of vaccines). Although we have outlined these potential explanations for the observed relationships, more research is needed to better understand the underlying mechanisms”.
I know, I have often posted nasty things about integrative medicine and those who promote it. Today, I want to make good for all my sins and look at the bright side.
Imagine you are a person convinced of the good that comes from so-called alternative medicine (SCAM). Imagine you believe it has stood the test of time, is natural, holistic, tackles the root problems of illness, etc., etc. Imagine you are such a person.
Your convictions made you support more research into SCAM because you feel that evidence is needed for it to be more generally accepted. So, you are keen to see more studies proving the efficacy of this or that SCAM in the management of this or that condition.
This, unfortunately, is where the problems start.
Not only is there not a lot of money and even fewer scientists to do this research, but the amount of studies that would need doing is monstrously big:
- There are hundreds of different types of SCAM.
- Each SCAM is advocated for hundreds of conditions.
Consequently, tens of thousands of studies are needed to only have one trial for each specific research question. This is tough for a SCAM enthusiast! It means he/she has to wait decades to see the light at the end of the tunnel.
But then it gets worse – much worse!
As the results of these studies come in, one after the other, you realize that most of them are not at all what you have been counting on. Many can be criticized for being of dismal quality and therefore inconclusive, and those that are rigorous tend to be negative.
Bloody hell! There you have been waiting patiently for decades and now you must realize that this wait did not take you anywhere near the goal that was so clear in your sight. Most reasonable people would give up at this stage; they would conclude that SCAM is a pipedream and direct their attention to something else. But not you! You are single-minded and convinced that SCAM is the future. Some people might even call you obsessed – obsessed and desperate.
It is out of this sense of desperation that the idea of integrative medicine was born. It is a brilliant coup that solves most of the insurmountable problems outlined above. All you need to do is to take the few positive findings that did emerge from the previous decades of research, find a political platform, and loudly proclaim:
SCAM does work.
Consumers like SCAM.
SCAM must be made available to all.
Consumers deserve the best of both worlds.
The future of healthcare evidently lies in integrated medicine.
Forgotten are all those irritating questions about the efficacy of this or that treatment. Now, it’s all about the big issue of wholesale integration of SCAM. Forgotten is the need for evidence – after all, we had decades of that! – now, the issue is no longer scientific, it is political.
And if anyone has the audacity to ask about evidence, he/she can be branded as a boring nit-picker. And if anyone doubts the value of integrated medicine, he/she will be identified as a politically incorrect dinosaur.
Mission accomplished!
The ‘Münster Circle‘ is an informal association of multi-disciplinary experts who critically examine issues in and around so-called alternative medicine (SCAM). We exist since June 2016 and are the result of an initiative by Dr Bettina Schöne-Seifert, Professor and Chair of Professor and Chair of Medical Ethics at the University of Münster.
In the past, we have published several documents which have stimulated discussions on SCAM-related subjects. Yesterday, we have published our ‘MEMORANDUM INTEGRATIVE MEDICINE‘. It is a critical analysis of this subject and will hopefully make some waves in Germany and beyond.
Here is its English summary:
The merging of alternative medicine and conventional medicine has been increasingly referred to as Integrative (or Integrated) Medicine (IM) since the 1990s and has largely replaced other terms in this field. Today, IM is represented at all levels.
IM is often characterised with the thesis of the ‘best of both worlds’. However, there is no generally accepted definition of IM. Common descriptions of IM emphasise:
– the combination of conventional and complementary methods,
– the holistic understanding of medicine,
– the great importance of the doctor-patient relationship,
– the hope for optimal therapeutic success,
– the focus on the patient,
– the high value of experiential knowledge.
On closer inspection, the descriptions of IM show numerous inconsistencies. For example, medicine in the hands of doctors is stressed, but it is also emphasised that all relevant professions would be involved. Scientific evidence is emphasised, but at the same time, it is stressed that IM itself includes homeopathy as well as other unsubstantiated treatments and is only ‘guided’ by evidence, i.e. not really evidence-based. It is claimed that IM is to be understood as ‘complementary to science-based medicine’; however, this implies that IM itself is not science-based.
The ‘best of both worlds’ thesis impresses many. However, if one investigates what is meant by ‘best’, one finds that this term is not interpreted in nearly the same way as in conventional medicine. Many claims of IM are elementary components of all good medicine and thus cannot be counted among the characterising features of IM. Finally, it is hard to ignore the fact that the supporters of IM use it as a pretext to introduce unproven or disproven modalities into conventional medicine. Contrary to promises, IM has no discernible potential to improve medicine; rather, it creates confusion and entails considerable dangers. This cannot be in the interest of patients.
Against this background, it must be demanded that IM is critically scrutinised at all levels.
________________________
Yesterday, it was announced that the new German health secretary will be Dr. Karl Lauterbach. This seems a most reasonable choice (when did the UK last have a physician in that post?), and I certainly wish him the best of luck in his new position.
Lauterbach studied medicine at the RWTH Aachen University, University of Texas at San Antonio and University of Düsseldorf, where he graduated. From 1989 to 1992, he studied health policy and management as well as epidemiology at the Harvard School of Public Health in Boston, graduating with a Doctor of Science in 1992. From 1992 to 1993, he held a fellowship at the Harvard Medical School.
From 1998 until 2005, Lauterbach served as the director of the Institute of Health Economics and Clinical Epidemiology (IGKE) at the University of Cologne. He was appointed adjunct professor at the Harvard School of Public Health in 2008. He was a member of the Sachverständigenrat zur Begutachtung der Entwicklung im Gesundheitswesen (the council of experts advising the federal government on developments in the German healthcare system) from 1999 until he was elected to the Bundestag in September 2005.
But why does his appointment put the German defenders of homeopathy in a panic? The reason is simple: Lauterbach has in the past repeatedly argued against the reimbursement of homeopathy in Germany. This is, for instance, what DER SPIEGEL wrote in 2019 (my translation):
SPD parliamentary group vice-chairman Karl Lauterbach wants to prohibit public health insurance companies from reimbursing the costs of homeopathy. “We have to talk about this in the coalition,” he told the “Tagesspiegel”. Health insurance companies in Germany are not obliged to cover the costs of homeopathic treatments. However, they can pay for it voluntarily.
Voluntary benefits by health insurers must also be economically and medically reasonable, Lauterbach argues, referring to a similar push in France. According to the French Supreme Health Authority (HAS), the funds do not have sufficient scientific effect. The Ministry of Health had previously commissioned the HAS with the examination. It is considered likely that the French government will soon abolish the coverage of costs.
“In the spirit of reason and education as well as patient protection, it is also wrong in Germany for insurance companies to pay for homeopathy for marketing reasons,” Lauterbach wrote on Twitter in reaction to the decision in France. His demand is not new. Lauterbach had already spoken out in 2010 for a ban on the assumption of costs.
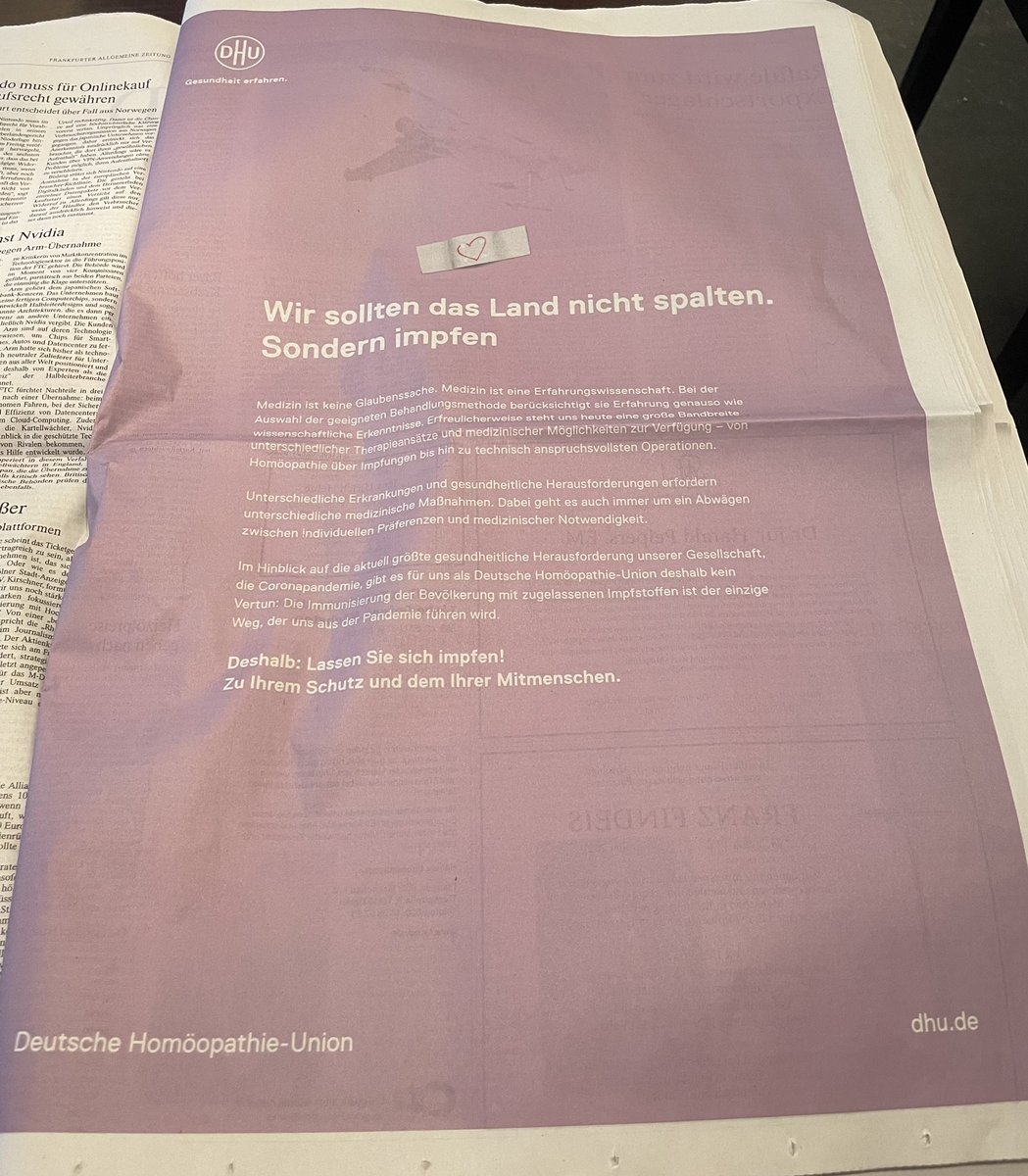
Many observers expect that Lauterbach – after getting the pandemic under control (not an easy task by any measure) – will indeed stop the reimbursement of homeopathy. Germany’s largest homeopathy producer reacted swiftly and is currently running an expensive campaign with full-page advertisements in German newspapers trying to improve the much-damaged public image of homeopathy:
In the advertisement above, for instance, it is implied that homeopaths are all in favor of vaccination. Regular readers of my blog will know that this is not true…
… and so does Dr. Lauterbach!
Psychosocial distress, depression, or anxiety are frequent problems of women after a breast cancer diagnosis and treatment. Many try so-called alternative medicine (SCAM) in an attempt to deal with them. But is this effective?
The purpose of this study was to assess the potential benefit of lavender oil as a perioperative adjunct to improve anxiety, depression, pain, and sleep in women undergoing microvascular breast reconstruction.
This was a prospective, single-blinded, randomized, controlled trial of 49 patients undergoing microvascular breast reconstruction. Patients were randomized to receive lavender oil or a placebo (coconut oil) throughout their period of hospitalization. The effect of lavender oil on perioperative stress, anxiety, depression, sleep, and pain was measured using the hospital anxiety and depression scale, Richards-Campbell Sleep Questionnaire, and the visual analogue scale.
Twenty-seven patients were assigned to the lavender group and 22 patients were assigned to the control group. No significant differences were seen in the perioperative setting between the groups with regard to anxiety (p = 0.82), depression, sleep, or pain scores. No adverse events were noted, and no significant differences in surgery-related complications were observed. When evaluating the entire cohort, postoperative anxiety scores were significantly lower than preoperative scores, while depression scores were significantly higher postoperatively as compared with preoperatively.
The authors concluded that, in the setting of microvascular breast reconstruction, lavender oil and aromatherapy had no significant adverse events or complications; however, there were no measurable advantages pertaining to metrics of depression, anxiety, sleep, or pain as compared with the control group.
One could argue that the sample size of the trial was too low to pick up small differences in the outcome measures. Yet, even then, the findings do not suggest that the treatment did make a large enough difference to justify the effort and expense of the treatment.
One could also argue that – who cares? – if a patient wants aromatherapy (or another SCAM that is harmless), why not? The answer to this is the fact that researchers have the ethical duty to identify the most effective treatment, and clinicians have the ethical duty to employ not just any odd therapy but the one that works demonstrably best. Seen from this perspective, the place of SCAM in cancer care seems far less certain than many enthusiasts try to make us believe.
The 13th European Congress for Integrative Medicine is about to take place online between 4 and 7 November 2021. It will host 125+ speakers presenting from around the world. The programme will cover the following topics.
- Anthroposophic Medicine
- Arts in Healthcare
- Acupuncture
- Antimicrobial Resistance
- Ayurveda
- Covid Research
- Diabetes
- Homeopathy
- Immunology
- Integrative Oncology
- Lifestyle Medicine
- Medical Education
- Mental Health & Stress Management
- Mind and Body Connection
- Mistletoe Therapy
- Nutrition, Gut Health & Microbiome
- Pain Management
- Patient Activation & Self-Management
- Planetary & Environmental Health
- Research and Evaluation
- Social Prescribing
- Traditional Health
- Yoga
Even looking at the more detailed list of lectures, I did not find a single contribution on conventional medicine (“Integrative medicine combines conventional medicine with…” [see below]) or a lecture that is remotely critical of integrative medicine. The definition of INTEGRATED MEDICINE (IM) adopted here seems similar to the US definition we recently discussed. Here is the European definition:
Integrative medicine combines conventional medicine with evidence-informed complementary medicine and therapies to achieve the optimum health and wellbeing of the patient. Focusing on a holistic, patient-centred approach to healthcare, it takes into consideration the patient’s physical and psychological wellbeing and treats the whole person rather than just the disease.
Allow me to do a quick analysis of this definition by looking at its key elements:
- Evidence-informed: While proper medicine is BASED on evidence, IM is merely INFORMED by it. The difference is fundamental. It allows IM clinicians to use any un- or disproven so-called alternative medicine (SCAM) they can think of or invent. The evidence for homeopathy fails to show that it is effective? Never mind, IM does not need to be evidence-based, it is evidence-informed. IM physicians know homeopathy is a placebo therapy (if not they would be ill-informed which would make them unethical), but they nevertheless use homeopathy (try to find an IM clinic that does not offer homeopathy!), because IM is not EBM. IM is evidence-informed!
- Therapies that achieve optimum health and wellbeing. This is odd because the website also states that “therapies can include anything from acupuncture, yoga, massage, aromatherapy, herbal medicine, nutrition, exercise along with many more approaches, tailored to the needs of the individual” indicating that virtually anything can be included. Anyway, “optimum health and wellbeing” seems a strange and unachievable criterion. In fact, it is nothing but a ‘bait and switch‘ salesmen’s trick.
- Holistic: This is a little trick that IM proponents love. With it, they imply that normal medicine is not holistic. However, this implication is demonstrably wrong. Any good medicine is holistic, and if a sector of healthcare fails to account for the whole person, we need to reform it. (Here are the conclusions of an editorial I published in 2007 entitled ‘Holistic heath care?‘: good health care is likely to be holistic but holistic health care, as it is marketed at present, is not necessarily good. The term ‘holistic’ may even be a ‘red herring’ which misleads patients. What matters most is whether or not any given approach optimally benefits the patient. This goal is best achieved with effective and safe interventions administered humanely — regardless of what label we put on them.) Creating a branch of medicine that, like IM, pretends to have a monopoly on holism is grossly misleading and can only hinder this process.
- Patient-centred: This is the same mean little trick in a different guise. They imply that conventional medicine is not patient-centred. Yet, all good medicine is, of course, patient-centred. To imply otherwise is just daft.
- Consideration of the patient’s physical and psychological wellbeing and treating the whole person rather than just the disease: Same trick yet again! The implication is that physical and psychological wellbeing and the whole person are not all that relevant in conventional medicine where only disease labels are being treated.
Altogether, this definition of IM is unworthy of anyone with the slightest ability to think critically. I find it much worse than the latest US definition (which already is fairly awful). In fact, it turns out to be a poorly disguised bonanza of strawman fallacies combined with ‘bait and switch’ deception.
How can this be?
How can a professional organisation engage in such mean trickery?
Perhaps a look at the list of speakers will go some way towards answering the question. Have a good look, you might recognize many individuals as members of our ALTERNATIVE MEDICINE HALL OF FAME.
PS
Registration costs £ 249 (standard rate)
PPS
Perhaps I should also mention at least 4 of the many commercial sponsors of the conference:
- Boiron
- Helixor
- Iscador
- Weleda