medical ethics
Guest post by Tobias Katz
What do we know?
ICU admission
Taken from the BMJ (Ref 1): ICNARC latest report 31/12/21 showed that the proportion of patients admitted to critical care in December 2021 with confirmed covid-19 who were unvaccinated was 61%.
Prevention of infection
The government’s week 45 Covid surveillance report (Ref 3) is clear that vaccination prevention of infection (positive PCR, for Delta) effectiveness is estimated at 65% for Oxford-AstraZeneca and 80% for Pfizer.
Prevention of transmission
The Lancet’s (Ref 4) paper, suggests once infected, initial viral load is similar for vaccinated and unvaccinated individuals, suggesting likely equal chance of transmitting on the virus.
Protection of the individual
Ref 3, is clear cut that vaccination protects individuals from hospitalisation and severe infection (for Delta).
(Omicron) “Among those who had received 2 doses of AstraZeneca, there was no effect against Omicron from 20 weeks after the second dose. Among those who had received 2 doses of Pfizer or Moderna effectiveness dropped from around 65-70% down to around 10% by 20 weeks after the 2nd dose. 2 to 4 weeks after a booster dose vaccine effectiveness ranged from around 65 to 75%, dropping to 55 to 70% at 5 to 9 weeks and 40-50% from 10+ weeks after the booster.” (Ref 2)
Effectiveness here is measured by admission to hospital and shows the necessity for booster jabs when fighting Omicron.
Who are Dr James and Dr Malhotra?
Steven James, consultant anaesthetist, has recently been in the news for confronting Sajid Javid RE mandatory vaccinations for hospital and nursing staff. “The science isn’t strong enough” to support the policy he stated and “I’ve got antibodies”, suggesting that he’s as protected as he would be if he had a vaccine.
Aseem Malhotra, who goes by the name of ‘lifestylemedicinedoctor’ on Instagram is an extremely controversial cardiology consultant who seems to be Djokovic’s biggest fan and whose tweets are passionately quoted and forwarded by anti-vaxxers.
With tweets such as “Mark my words, with everything we know and don’t know about the current vaccine Novak Djokovic will ultimately be proven to be on the right side of history #BadPharma #truth #transparency #InformedConsent”:
Mark my words, with everything we know and don’t know about the current vaccine Novak Djokovic will ultimately be proven to be on the right side of history #BadPharma #truth #transparency #InformedConsent
— Dr Aseem Malhotra (@DrAseemMalhotra) January 9, 2022
And a retweet: “Dr Jordan Peterson Oh well. It’s just fertility. Women’s Periods May Be Late After Coronavirus Vaccination, Study Suggests”; he stirs the cooking pot of anti-establishment rhetoric and only deepens an already fractured relationship between doctors and their patients caused by the pandemic.
Oh well. It's just fertility. Women’s Periods May Be Late After Coronavirus Vaccination, Study Suggests https://t.co/ndQC9QgwMH
— Dr Jordan B Peterson (@jordanbpeterson) January 8, 2022
You’d think a mature, well-researched doctor would be able to tell the difference between the menstrual cycle and becoming fertile. You’d also hope he would not be short-sighted enough to support one of the most anti-science/anti-conventional medicine public figures in the world (see here)… Alas, no.
I feel as though both of these figures need to be reminded of their ethical duty of candour as doctors and reminded that their public actions have consequences. I may not completely disagree with Dr James (RE mandatory vaccinations) but the way in which he conducted himself during this nationally broadcasted video left many shaking with rage as it undermines many of his health professional colleagues. Me, included.
When a doctor appears on national news, opposing [mandatory] vaccination and offering incorrect explanations of why this is so, it should be obvious to them that their opinion will inevitably act as anti-vaccine propaganda, whether meant for this or not.
Malhotra’s ideas (cutting back on statins, healthy diet etc.) are often worth consideration/evaluation and as a new-age medical ‘influencer’ with 130k+ followers on Twitter, with ample publications behind him, he deserves to be listened to. Not necessarily agreed with, but listened to. But he also has a duty as a doctor to guard against complacency. Similar to James’ public actions, Malhotra’s tweets that are so one-sided give a biased, inaccurate and frankly dangerous view on the efficacy and safety profile of COVID vaccinations that have been safely and effectively used in millions of people to prevent hospitalisations. Is he doing it for the views? The hits? The likes? The retweets? To have people recognise him for his Pioppi diet?
What should we do?
Candour
Doctors, including James and Malhotra have an ethical responsibility not to spread imperfect information to a wide-receiving audience where their actions can be misconstrued and misrepresented so easily. Doing so may bolster anti-vaccine views, cause less ‘on-the-fence’ people to get the jabs and essentially lead to more preventable deaths.
More and more we are seeing social media take over and often act as the public’s primary source of news. More doctors than ever are now in the [social] media limelight. Some, such as Dr Alex George (mental health advocate) are promoting health responsibly. Others, seek to undermine it. In an era when Joe Rogan has more daily views than Fox News’ Tucker Carlson, to ignore and not rebut [health] social media giants like Malhotra would just worsen the situation. Malhotra and James need to be challenged by the scientific community, as the BBC so brilliantly did here.
Complacency
If doctors want to become socialite Instagram influencers, they must do this without complacency. I think this means being responsible when offering controversial and potentially public health implicating opinions where evidence isn’t clear cut.
Final thoughts
Using all the possible information above, as the vaccines are not 100% without risk, transmission is not completely cut post-vaccine and as we have a decent-ish way of monitoring infection (lateral flows and PCRs), I feel as though mandating vaccines for all NHS staff is currently unjust. I see Steve’s point. But I’d be extremely careful in how I’d make this point. And certainly not on live Sky News when the nation is watching, where it will inevitably be seized upon by the anti-vax community.
Saying this, the data is pretty clear that there is evidence that the vaccines offer protection against infection, reducing viral load quicker once infected and against hospitalisation and so if you’re a rational doctor who thinks that at least one time your lateral flow test may give a false negative, it makes complete sense to get your vaccine to protect your patients…
References
- https://www.bmj.com/content/376/bmj.o5?fbclid=IwAR2MgoD_vYo0FsaVsQdLxfeYCukuRu2RegcJa-HclA13byhH71g-AnNhnP8
- https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1045329/Vaccine_surveillance_report_week_1_2022.pdf
- https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1032859/Vaccine_surveillance_report_-_week_45.pdf
- https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(21)00690-3/fulltext
Please take a moment to read this short letter by the ‘LIGA MEDICORUM HOMOEOPATHICA INTERNATIONALIS’:
As you know, the World Health Organization (WHO) is predicting that civilization faces a crisis of antibiotic-resistant diseases that may soon result in as many as 10 million deaths per year while pushing as many as 24 million people into extreme poverty.
We, the undersigned, are duly licensed healthcare professionals practicing homeopathy, with the authority to diagnose and treat disease, who have reviewed the extensive research literature demonstrating the clear therapeutic value of homeopathy. Each of us has had extensive clinical experience successfully treating hundreds of thousands of patients suffering from infectious diseases worldwide.
Homeopathy works, does not cause further antibiotic resistance, is generally devoid of side effects, is inexpensive, and is good for health of the planet.
We are calling upon the WHO to encourage the international medical community to immediately begin training in homeopathy as an adjunctive therapeutic measure to avoid this catastrophic loss of life and would like a meeting with you or your representative to discuss the grave challenge of antibiotic resistance at your earliest convenience.
Thank you for considering this urgent appeal.
________________________
I stated above that this is a letter. In fact, it is more – it is a petition directed to the Director-General of the World Health Organization (WHO), Dr. Tedros Adhanom Ghebreyesus, to immediately begin training physicians in homeopathy as an adjunctive therapeutic measure to combat the looming crisis of antibiotic-resistant diseases.
The Liga Medicorum Homoeopathica Internationalis (LMHI) represents homeopathic physicians in more than 70 countries all over the world. The purposes of the association are the development and securing of homeopathy worldwide and the creation of a link among licensed homeopaths with medical diplomas and societies and persons who are interested in homeopathy. The LMHI is exclusively devoted to non-profit activities serving philanthropic benefits.
The LMHI might ring a bell for regular readers of this blog. A few years ago, I reported that its president advocates curing cancers with homeopathy. And in 2014, I reported that a journey to Liberia of leading homeopaths was co-organized by the LMHI; its purpose was to cure Ebola patients of their disease with homeopathy.
I find all of this seriously worrying – not because I fear that the WHO will now start training physicians across the globe in homeopathy. It is worrying, I feel, because it shows how hopelessly deluded homeopaths are. The fact that clinicians so far detached from reality treat ill and vulnerable patients frightens me.
On this blog and elsewhere, I have heard many strange arguments against COVID-19 vaccinations. I get the impression that most proponents of so-called alternative medicine (SCAM) hold or sympathize with such notions. Here is a list of those arguments that have come up most frequently together with my (very short) comments:
COVID is not dangerous
It’s just a flu and nothing to be really afraid of, they say. Therefore, no good reason exists for getting vaccinated. This, I think, is easily countered by pointing out that to date about 5.5 million people have died of COVID-19. In addition, I fear that the issues of ‘long-COVID’ is omitted in such discussions
It’s only the oldies who die
As an oldie myself, I find this argument quite distasteful. More importantly, it is simply not correct.
Vaccines don’t work
True they do not protect us 100% from the infection. But they very dramatically reduce the likelihood of severe illness or death from COVID-19.
Vaccines are unsafe
We have now administered almost 10 billion vaccinations worldwide. Thus we know a lot about the risks. In absolute terms, there is a vast amount of cases, and it would be very odd otherwise; just think of the rate of nocebo effects that must be expected. However, the risks are mostly minor, and serious ones are very rare. Some anti-vaxxers predicted that, by last September, the vaccinated population would be dead. This did not happen, did it? The fact is that the benefits of these vaccinations hugely outweigh the risks.
Vaccines are a vicious tracking system
Some claim that ‘they‘ use vaccines to be able to trace the vaccinated people. Who are ‘they‘, and why would anyone want to trace me when my credit card, mobile phone, etc. already could do that?
Vaccines are used for population control
‘They‘ want to reduce the world population through deadly vaccines to ~5 billion, some anti-vaxxers say. Again, who are ‘they‘ and would ‘they‘ want to do that? Presumably ‘they‘ need us to pay taxes and buy their goods and services.
There has not been enough research
If those who make this argument would bother to go on Medline and look for COVID-related research, they might see how ill-informed this argument is. Since 2021, more than 200 000 papers on the subject have emerged.
I trust my immune system
This is just daft. I am triple-vaccinated and also hope that I can trust my immune system – this is why I got vaccinated in the first place. Vaccinations rely on the immune system to work.
It’s all about making money
Yes, the pharma industry aims to make money; this is a sad reality. But does that really mean that their products are useless? I don’t see the logic here.
People should have the choice
I am all for it! But if someone’s poor choice endangers my life, I do object. For instance, I expect other people not to smoke in public places, stop at red traffic lights and drive on the correct side of the street.
Most COVID patients in hospitals have been vaccinated
If a large percentage of the population has been vaccinated and the vaccine conveys not 100% protection, it would be most surprising, if it were otherwise.
I have a friend who…
All sorts of anecdotes are in circulation. The thing to remember here is that the plural of anecdote is anecdotes and not evidence.
SCAM works just as well
Of course, that argument had to be expected from SCAM proponents. The best response here is this: SHOW ME THE EVIDENCE! In response SCAM fans have so far only been able to produce ‘studies’ that are unconvincing or outright laughable.
In conclusion, the arguments put forward by anti-vaxxers or vaccination-hesitant people are rubbish. It is time they inform themselves better and consider information that originates from outside their bubble. It is time they realize that their attitude is endangering others.
Like so many other anti-vaxxers, Djokovic is deep into so-called alternative medicine (SCAM).
An article in THE TELEGRAPH explains it quite clearly. Here are a few passages:
Here is an anti-scientific crank hiding in plain sight … [In his book Djokovic explains] how he suffered from recurring physical ailments – allergies, breathing difficulties, blocked sinuses – until he gave up gluten.
Nothing especially weird so far – until he explains how his gluten intolerance was diagnosed. A Serbian nutritionist called Dr Igor Cetojevic asked Djokovic to hold his right arm out at right angles and resist the pressure as he pushed down on it. Then the exercise was repeated, only this time while Djokovic held a slice of bread against his stomach. “I was noticeably weaker,” writes Djokovic, who adds that “kinesiological arm testing [has] long been used as a diagnostic tool by natural healers.” Yes, and mediums have long claimed to speak to the dead …
Here is a man who broke up his visits to Wimbledon with trips to the nearby Buddhapadipa Temple to meditate by a lake. A man who revealed two years ago that he has a “friend” in Melbourne’s Botanical Gardens – “a Brazilian fig tree that I like to climb”. Yes, Djokovic’s jet-setting spiritualism might sound charming in itself. But its side-effect has been credulousness.
Serve To Win [ND’s book] describes a so-called “researcher” taking two glasses of water and directing loving energy towards one, while swearing angrily at the other. “After a few days … [the angry glass] was tinted slightly green … the other glass was still bright and crystal clear”. Harmless, perhaps, if deeply dippy. But then, last year, Djokovic could be found hosting a former estate agent called Chervin Jafarieh on his Instagram Live channel. Jafarieh was selling bottles of Advanced Brain Nutrients at $50 apiece, which – like Djokovic’s resistance to the Covid vaccination – sounded contrary to the interests of public health…
… Djokovic expressed in a 2018 interview with Shortlist magazine. “I believe that it is our mission to reach a higher frequency through self-care by exploring and respecting our own avatar, our body and, by doing that, raising the vibration of the planet.” …
And so we return to the dark side of this whole peculiar tale. Were Djokovic just a journeyman player, his pseudo-scientific beliefs would be no more than a bizarre footnote. As it is, he is a powerful role model, particularly in the Balkans. Thousands of people have probably emulated his stance on vaccines. Some are likely to suffer consequences as a result…
Another article explains:
New York Times tennis reporter Ben Rothenberg tweeted out after the news of Djokovic’s visa rejection that the Serbian had been “wildly anti-science” over the years. 
“Let’s not lose sight of how wildly anti-science Djokovic has publicly been for years,” Rothenberg began. “Here he was last year preaching about how you can change water with emotion.
“Naive, but maybe these real consequences today can be a reality check for his nonsense?”
Former New York Times reporter Steven Greenhouse said it was “sad to see such a brilliant tennis player join the anti-science, pro-poppycock anti-vaxxers”.
Tennis Channel producer David Kane added: “I sort of don’t care whether Australia bungled L’Affaire Novak because of political/media pressure. This is about someone who has been stridently anti-science and never indicated a good faith effort to receive this essentially mandatory vaccine.F around & find out, as they say.”
And a Guardian article provides further information:
His belief in alternative medicine is complemented by his commitment to alternative history. He frequently retreats to Visoko, in the hills of Bosnia and Herzegovina, where he meets up with the businessman Semir Osmanagic – whose claims that there are ancient man-made structures with magical healing powers, refuted by scientists, have turned the hills into a lucrative tourist destination. Djokovic has also expressed his support for the ultranationalist alternative historian Jovan Deretic, whose writings claim, among other things, that numerous European cultures, including ancient Greeks, Celts and Etruscans, are descended from Serbs.
I am quite confident that I play tennis as splendidly as Djokovic understands medicine. Yet, I do not pretend to be able to teach you how to do a perfect ‘top slice’. In contrast, Djokovic loves to take the role of ambassador for SCAM and other weird stuff.
His father stated that “Novak is the Spartacus of the new world who does not tolerate injustice, colonialism and hypocrisy but fights for the equality of all on this planet, regardless of skin color, religious belief and money they have.” Personally, I see this differently: Djokovic is badly affected by proctophasia; he tolerates no end of BS and fights for pseudoscience. And sadly, his views are all too persuasive to gullible consumers – not exactly what we need in a global health crisis!
As you know, I am not in the habit of telling personal stories on this blog. Today, allow me to make an exception by taking you back 40 years into my own history.
Back in the 1980s, I spent much of my time doing research in hemorheology (flow properties of blood). At the time, this was a buoyant area of research, and my late friend Arpad Matrai and I were enthusiastically investigating it, first in London under John Dormandy and later at the LMU in Munich. But we were by no means the only team working in hemorheology. Another group at Aachen was much larger, better-funded, and in many ways way ahead of us. One member of that group regularly irritated us; this was Holger Kiesewetter, the ‘hero’ of my story.
Arpad was sure that much of Kiesewetter’s work and even more of his financial dealings were suspect (“How come a junior research can afford driving a Porsche?”, he used to wonder). Something did not seem quite right. Despite our reservations, we did collaborate occasionally. In 1984, we even managed to co-organize a conference and jointly publish its proceedings.
After my friend and co-worker Arpad had died of leukemia, I gradually drifted back into clinical medicine, became a professor of rehab medicine first in Hannover and then in Vienna. This also meant that I completely lost touch with Holger Kiesewetter. I was, therefore, more than a little surprised to one day receive a phone call from him in Vienna. He told me that he had applied for a professorship at my Uni and asked me to support his application. I did not promise to do so and I certainly did not lend my support to his application. Quite simply, I remembered too many instances that gave me reasons to be concerned about my ‘friend’s’ integrity.
Kiesewetter did not get the Vienna post but I later learned that he had become a professor of transfusion medicine at the Charite in Berlin. In the mid-1990s, a chance meeting at an airport occurred when we were both catching flights. He told me that he was doing fine, and he seemed to have his fingers in many pies.
Then I lost sight of him completely.
Until yesterday, that is.
I was doing some searches on herbal remedies when I came across the intriguing subject of ‘BIO VIAGRA‘. A German article reported this:
“In clinical trials, 50 men had much better sex afterward, more fun in bed, and just generally felt better about themselves,” the Sueddeutsche Zeitung daily cited Olaf Schroeder from Berlin’s Charite hospital as saying. “Their libido was even higher than the control group taking Viagra,” he said. The potent cocktail includes tribulus terrestris, a herb already used in alternative medicine, a root vegetable found in the Andes called maca and grape juice extract, newspapers said. The treatment, dubbed “Plantagrar”, is due to be launched in early 2010, the Bild daily said.
Having published a review of maca, I was interested and continued searching.
Another article stated that a certain Mr. Schröder had stated that he had investigated the efficacy of the remedy on 50 test persons. However, the data of the experiment have not been published. In addition, the researchers’ procedure has been massively criticized: 25 men were given the bio-potency drug, 25 others a placebo, i.e. a tablet without active ingredients. Afterward, the test persons were to compare their experiences with those they had had with Viagra. Fritz Sörgel, director of the Nuremberg Institute for Biomedical and Pharmaceutical Research, calls the procedure “completely dubious”. “This is a completely new kind of study that this doctoral student has invented.” The number of test persons is much too low, the comparison with Viagra cannot be taken seriously.
This sounded already quite dodgy, and a third article in the usually reliable German Medical Journal provided more details:
For several months, those involved kept a low profile, but now the affair surrounding the development of a herbal aphrodisiac at Berlin’s Charité University Hospital has consequences: Last week, the head of the Institute for Transfusion Medicine, Prof. Dr.-Ing. Dr. med. Holger Kiesewetter, was given leave of absence. This step was taken “at his own request”, said hospital spokesperson Claudia Peter. The withdrawal came about two weeks after the public prosecutor’s office searched his work and private rooms as well as other locations.
The “Bio-Viagra affair” had caused a furore in mid-March. A doctoral student of Kiesewetter’s had claimed to the Deutsche Presse-Agentur that he had successfully developed an aphrodisiac on a purely herbal basis. Some daily newspapers reported on the remedy, which was called “Plantagrar”. A little later, however, the Charité management denied it. It was “the activity of an employee (. . .) on his own responsibility”. The case also came to the attention of the drug supervisory authority. Erectile dysfunctions are recognised diseases according to the ICD-10 classification system. The “Bio-Viagra” was therefore a drug whose development should have been controlled, the state office for health and social affairs said.
A spokesperson for the Berlin public prosecutor’s office confirmed the presumption of a violation of the German Medicines Act to the Deutsches Ärzteblatt. In addition, Kiesewetter is being investigated for bribery, corruption and breach of trust to the detriment of the Charité. The head of the institute had apparently been promised benefits by private companies.
That sounded very much like the Kiesewetter I remembered. I was unable to find the actual trial or more details about the herbal remedy. The scandal seems to have put an end not only to the university career of the researchers but also to the aphrodisiac.
However, I did find a Wiki page about Kiesewetter that suggests that ‘bio viagra’ was by no means the only escapade from the straight and narrow. But what is he up to today? Did he retire? No, after the debacle at the Charite, he seems to have gone into private practice:
After working as director of the Institute for Transfusion Medicine and Immunohaematology at the Charité and head of the coagulation outpatient clinic at the Charité, he has been providing patient care at the Hämostaseologicum Berlin-Mitte since 2010.
This is also the address he used for his most recent (2020) publication.
Am I worried about my old ‘friend’?
No, I am confident that he is doing just fine … financially, I mean.
For my last post of the year 2021, I take the liberty to borrow parts of a BMJ editorial entitled A NEW YEAR’S RESOLUTION OF HEALTH WORKERS:
The prospect of a return to normality seems within reach. But what will that normality look like? We believe that health workers, who have been at the frontline of the pandemic, must offer a vision of a healthier future. We must not let the terrible events of this year recast the pre-pandemic world in a glowing light. The normality we departed from at the onset of the pandemic was unjust, unsustainable, and shaped the evolution of, and responses to, the pandemic with devastating consequences, particularly for the most deprived and vulnerable.
The start of a new year offers an opportunity to question old ways of working and to ask how we can create a better future for everyone. It is a cliché to say that you should never waste a crisis. Just as in wartime and in the global financial crisis, many have profited greatly from the pandemic, whether as providers of online services or by taking advantage of the rush to procure essential goods such as personal protective equipment.
But many were far less fortunate, living in circumstances that rendered them vulnerable to an infection that spread especially rapidly through communities where successive generations had been living ever more precarious lives. As the recovery begins, the powerful groups who benefited from the social and economic systems that created those conditions will, once again, seek to shape the world to their advantage. Health workers cannot remain silent. They must offer a compelling vision of how we should reconfigure the world so that it produces and sustains health for all, resilient in the face of future threats…
A country navigating the pandemic is like a ship navigating treacherous and unpredictable waters in a storm. If the ship, its crew, and its passengers are to come through the experience unscathed it needs three things. First, it needs an experienced captain who understands the ship and commands the trust of the crew. Unfortunately, in some of the countries worst affected, captains were either away from the bridge, denied there was a storm, or had lost the trust of those on whom they depended.
Second, it needs a crew that is adequate for the size of the ship, that is well trained, and that is working as a team to achieve the same goal. Yet in too many countries, skeleton crews were working in health systems that were highly fragmented. Dissenting voices who raise the alarm about the integrity of the ship, the working of the team, or its leadership must not be silenced or lives can be lost. It also needs passengers who are as seaworthy as possible so that they can withstand the storm. One of the sentinel challenges of covid-19 was finding large segments of the population weighted by a disproportionate burden of preventable disease that predisposed them to severe covid-19 once infected.
Third, we need a ship that is securely constructed. Yet in many of the countries that have fared worst, we have been working in vessels that are full of holes. Social safety nets have been ripped asunder, allowing too many people to fall through the holes. We have made many demands on our people—to stay at home, to face loss of income—and we have added greater uncertainty to what were already difficult situations, particularly for certain racially and economically marginalised groups. The disproportionate exposure to covid-19 of many in these groups—a consequence of precarious jobs and social circumstances that denied them the luxury of social distancing—drove, in large part, the high burden of covid-19 among minority and marginalised groups worldwide.
As we look to the prospect of a covid-19 secure future, with effective vaccines, new treatments, and continued countermeasures as necessary, we must ask how we can strengthen the foundations of our societies, coming together to repair the torn safety nets. We must never be afraid to challenge our political leaders when they are going in the wrong direction, and we must insist that they really are guided by the science, and not just those bits that support their beliefs. And we must ensure that our fellow citizens are as healthy as possible so they can withstand the inevitable storms that lie ahead. We must insist that our health systems and other public systems are adequately staffed, with the tools needed to do the job, with teams that are working together, pulling in the same direction. If we do all this, then we, and the populations we serve, can be confident that we can weather any future storms.
___________________________
The editorial was written by 4 authors:
- Martin McKee, professor of European public health
- May C I van Schalkwyk, NIHR doctoral research fellow
- Nason Maani, assistant professor in public health evaluation
- Sandro Galea, dean
I think it is most sensible and thought-provoking and I suspect many of us agree with its sentiments. If it did not make you think, perhaps this information will do so:
The editorial was published one year ago in the Christmas issue of the BMJ
2020!
Yes, 2021 has disappointed many of our hopes and turned out to be a difficult year.
I wish us all that 2022 will be better, much better.
Always on the lookout for so-called alternative medicine (SCAM) that we have not yet covered on this blog, I came across a really weird one. ‘Access Consciousness’ (AC) is claimed to be a form of self-improvement therapy based on the idea that you are not wrong, that you know, and that consciousness can shift anything. It gives you access to the possibilities that exist when you no longer stick yourself and no longer believe that you are stuck. [1] Gary Douglas ([pictured below] “bestselling author, international speaker and business innovator”) pioneered this set of transformational tools in the 1990s. His work is claimed to have now spread to more than 170 countries and is claimed to have transformed the lives of tens of thousands of people. 
Access Consciousness allegedly empowers people to help themselves. The techniques of AC focus on your knowledge about yourself and the world around you. Part of what makes AC so different, according to its promoters, is that it is continuously being created. [2] AC promises to assist people with their health, weight, money, sex, relationships, anxiety, etc. It promises members, known as ‘Accessories,’ to become more conscious. To fully get it, Accessories should take part in classes. There they have 32 points on their heads lightly touched which is supposed to help them let go of all the thoughts, ideas, and emotions stored in any lifetime. Accessories are claimed to be able to “uncreate” memories of the past, or preconceived ideas picked up throughout a lifetime. As far as I can see, there is no evidence to suggest that AC is effective.
Some ex-members have alleged that AC is a “scam cooked up by a conman to rinse the vulnerable of their savings, a Scientology knock-off, and even a cult”. One ex-Accessory, for instance, claimed the group “programs its members to think like robots. It is very clever how it is done. Because it’s not like any other cult but it is mind control.” [3] In each 90-minute session, which costs up to US$ 300, 5,000 to 10,000 years of “limitations” are released, it is claimed.
My conclusion: there is no evidence that AC is plausible or effective and it is a SCAM and possibly also a cult.
[1] About Access Consciousness | Dr. Dain Heer (drdainheer.com)
[2] About Access Consciousness | Access Consciousness
[3] ‘Scientology knock-off’: Whistleblower exposes ‘cult’ that thinks ‘children are sexy’ (EXCLUSIVE) — RT UK News
THE GUARDIAN published an interesting article about vaccination hesitancy yesterday. Here is a short passage from it:
One major missing piece of the puzzle, currently under consideration, is a strategy that gets to the bottom of why 5 million people remained unvaccinated, especially those in communities with an ingrained distrust of authority.
No 10 even turned to an artificial intelligence (AI) company earlier in the year to determine the causes of vaccine hesitancy, but Whitehall sources acknowledge there is still a lack of understanding about how many of the unvaccinated remain so because of entrenched anti-vax ideology, misconceptions that could be turned around, a lack of time or transport to get to vaccine centres, or just apathy.
Yesterday, it was also reported in DER STANDARD that the Austrian Science Minister Martin Polaschek has commissioned a study from Statistics Austria, which for the first time was to look at the vaccination status of the population according to socio-economic characteristics.
The study yielded fascinating findings that might shed some light on the phenomenon of ‘entrenched anti-vax ideology’:
- Across all age groups, the proportion of vaccinated persons, including recovered persons, is 67%.
- Slightly less than four percent of the population are only recovered, and about 30% are neither one nor the other.
- There are no marked differences between men and women.
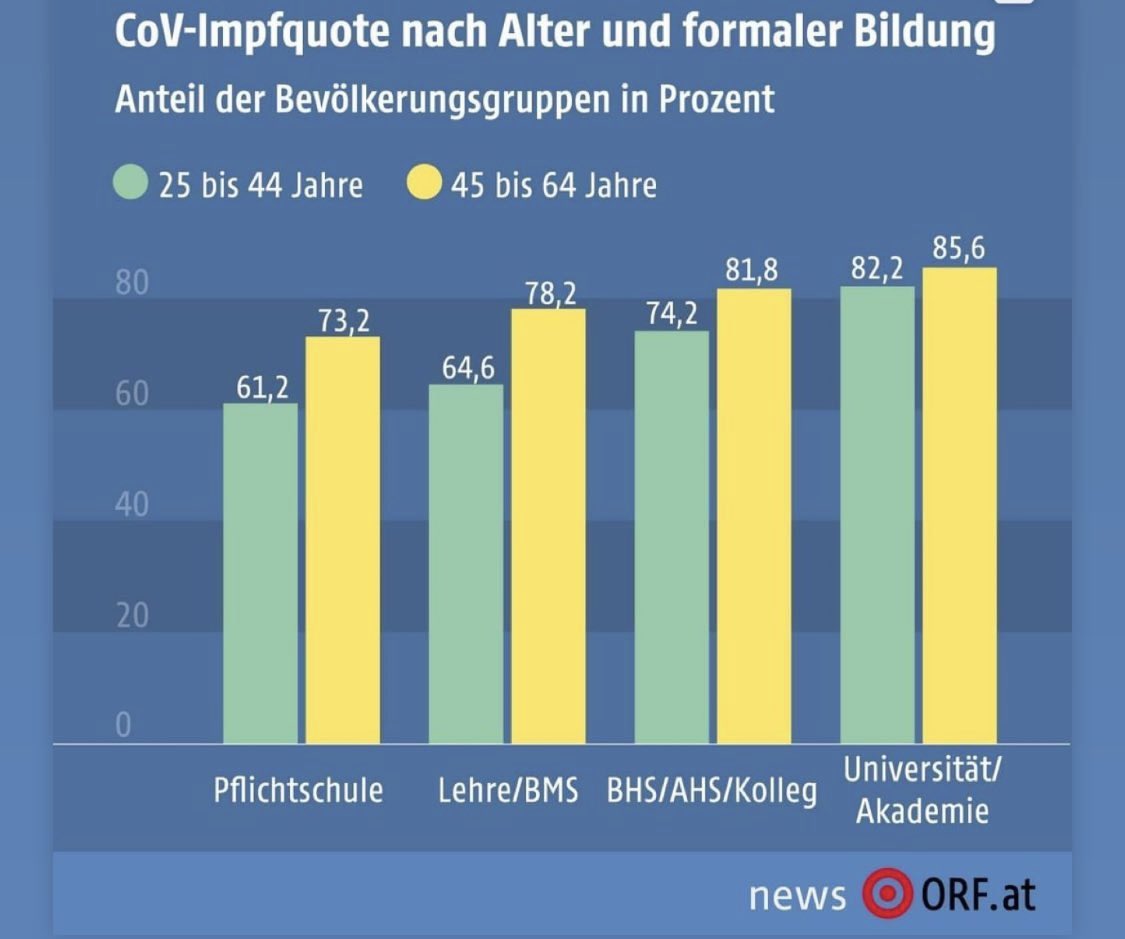
- The willingness to vaccinate is strongly related to the level of education.
- The vaccination rate in the group of 25-64 year-olds with a university degree is about 84% and thus significantly higher than among those who have only basic education (68%).
- In this age group, it also seems important whether someone has a job (76%) or not (69%).
- People employed in the information and communication sector (85%) and public administration (83%) are the most likely to be vaccinated.
- Workers in agriculture and forestry (67%) and construction (65%) are the least likely to accept vaccinations.
- Health and social services personnel have a vaccination rate of 79%.
- More than half of the 600,000 schoolchildren had already been vaccinated, and in the upper secondary school it was even 72%.
- The rate among teachers is also high, at 85%.
- 86% of the approximately 395,000 students at universities had been vaccinated.
- As 92% of all medical students were vaccinated.
- The vaccination rate among Austrian nationals, at about 70%, is clearly higher than that of people without an Austrian passport (52%).
- The difference between those born in Austria and those not born in Austria is only five percentage points.
- The willingness to be vaccinated is higher among people from Turkey (73%) than among those born in Austria (68%).
- Among Germans and Afghans, it is around 72%.
- People from Romania (43%) and the Russian Federation (45%) have the lowest vaccination rates.
- The percentage of vaccinated people is highest among those between 75 and 84 years.
Similar findings have, of course, been reported from other countries. However, what seems new to me here is the finding that vaccination rates are strongly correlated to the level of education: the anti-vax brigade tends to be uneducated and ignorant. If confirmed, this suggests that education might be a way to make them accept vaccinations.
PS
Of course, correlation is not causality. But there seems to be a dose-response relationship between education and willingness to vaccinate. This makes a causal effect more likely.
THOSE WHO KNOW NOTHING MUST BELIEVE EVERYTHING
DNP (2,4-dinitrophenol) is highly toxic. In the UK, it is illegal to sell DNP for human consumption. DNP causes serious harm to health. Its consumption has resulted in a significant number of deaths in the UK. Other side effects of DNP include: 
- nausea
- vomiting
- restlessness
- flushed skin
- sweating
- dizziness
- headaches
- rapid breathing
- an irregular heartbeat.
All this does not seem to deter entrepreneurs in so-called alternative medicine (SCAM). One of them has just been jailed. Jack Finney, 25, of Northwich in Cheshire, sold the highly toxic chemical 2.4-Dinitrophenol (DNP) between June 2017 and July 2020 on the dark web. Finney was sentenced at Chester Crown Court and was handed a 28-month prison sentence.
In 2018, 31-year-old businessman Bernard Rebelo, from east London, was the first person to be convicted of manslaughter in relation to the sale of DNP pills. Mr Rebelo became a millionaire after selling the ‘weight-loss capsules’ to clients, but he was jailed for seven years after selling them to bulimic student Eloise Parry, who later died.
Reginald Bevan, Deputy Head of the National Food Crime Unit, said: ‘We welcome today’s sentencing as it sends a strong message to anyone seeking to profit from the illegal sale of this life-threatening substance. We continue to be relentless in pursuing and bringing to justice those who are endangering the public and breaking the law. This operation continues to demonstrate how seriously the NFCU takes the illegal sale of DNP for human consumption in the UK and through our close working partnership with local authorities and other law enforcement agencies in the UK and abroad that we are able to tackle offenders, close websites and work to disrupt possible supply routes within and into the UK.’
In Germany, the anti-vax movement is frighteningly strong and it constitutes one of the main reasons for the relatively immunization rate. In no small part, this is due to the many anti-vax Heilpraktiker who practice in Germany. In an attempt to put the record straight, the ‘Verband Klassischer Homöopathen Deutschlands’ (VKHD, Association of Classical Homeopaths of Germany) recently published an article entitled ‘Heilpraktiker – Homeopathy – Vaccination’ (Heilpraktiker – Homöopathie – Impfen). Here is a short excerpt (my translation):
… There is a clear conceptual similarity between homeopathy and vaccination [1]. From a historical point of view, this was already reflected in the early days of homeopathy, when its discoverer, Samuel Hahnemann, expressed himself very positively with regard to the smallpox vaccination newly introduced at that time [2]. Thus, it is historically wrong to insinuate that users of homeopathy have a fundamentally negative attitude towards vaccinations [3]. In this context, terms such as “vaccination opponents” or “vaccination refusers” are misleading and defamatory [4].
A critical (not skeptical) approach to the topic of vaccinations is basically a characteristic of people with medical expertise. Such an attitude corresponds to the critical consideration necessary in daily practice and in each individual case to advise on suitable therapy options [5]. Properly working alternative practitioners give differentiated advice accordingly [6]. A fundamentally vaccine-rejecting attitude is precisely not a characteristic of a critical assessment that has taken place. The same applies to an unreflective recommendation of vaccinations or therapy methods, without taking into account individual factors as well as scientific and social backgrounds [7].
For the VKHD, we cannot give exact figures on recovered, vaccinated, or unvaccinated members. It is not the responsibility of a professional association to demand such information from its members [8]. We assume that alternative practitioners who provide information on vaccinations do so in accordance with a responsible ethical attitude, regardless of their own vaccination status [9] …
I have taken the liberty of inserting some references into this text. They relate to my comments, which are as follows:
- A conceptual similarity between vaccination and homeopathy exists only in the minds of homeopaths. They often claim that both use highly diluted remedies. This is wrong because homeopathic remedies do not usually contain active ingredients, whereas vaccines do. This fact also explains why homeopathics do not produce immune reactions, whereas vaccines do.
- Correct! Hahnemann was in favor of vaccination. That is why he would be ashamed today if he knew how many homeopaths oppose vaccination.
- What has this got to do with ‘historical’? I assume that the ‘insinuations’ refer to the situation today. Further, I don’t think anyone is suggesting that all homeopaths are ‘fundamentally’ opposed to vaccination. However, that many of them are anti-vaxers is an indisputable fact.
- I would rather think they are accurate.
- Correct.
- How can they without any medical background?
- Is it to be implied here that real medical people do?
- Maybe not ‘demand’, but inquire or request would be possible and desirable, wouldn’t it?
- It is nice that you believe this. But belief is not evidence.