bogus claims
By guest blogger João Júlio Cerqueira
A word of caution to all the skeptics out there defending Reason, Science, and the Truth. This is a summary of a long story and only about one of many battles. It is not a very beautiful story but it is what it is. I’m a medical doctor, influenced by some of the great minds of our time, all of them familiar to you, Edzard Ernst, Steven Novella, David Gorski, Harriet Hall, Kimball Atwood and so much more (thank you all, for everything that you do).
I started reading skeptic blogs in 2013 and was amazed by the lack of critical thinking about science production and the lack of knowledge about pseudoscience in the medical community. And if this was bad in the medical community, in the general population it should be close to apocalyptic…
In 2017, I was confronted by a medical doctor that imported the great pitches of international charlatans. From alkaline diet, bioidentical hormones, colonic cleansings all through the “health benefits” of drinking diluted saltwater…yes, this is a real thing. He was transformed into a television celebrity, wrote one of the bestselling books in my country, and only a few people were horrified by what was happening. How? How can someone that says that kind of stuff could have this kind of reach in the media? He even sold foot detox!
So, frustrated by the lack of action of the regulatory institutions and the lack of critical approach by the media, I decided to create a blog that I called SCIMED. Using what I had learned through the years with “the masters of skepticism”, I tried to teach and convince people why pseudoscience is useless and dangerous. Why those selling pseudoscience are a danger to society and are only after the wallet of scientifically illiterate people.
Thanks to hard work and a lot of luck, the blog started to have a decent public projection. Started to get invitations to interviews in the media, invited to speak at conferences, started to write in the opinion section of mainstream journals, appearing on television, invited to do a TEDx talk, was invited to be one of the subscribers to the first world manifesto against pseudoscience and even had the pleasure to be a speaker in a conference side by side with Edzard Ernst, one of my heroes!
It was like something was changing. Well, it was not.
With public projection, came the problems…people calling my employers to get me fired, physical and death threats, constant harassment by email or in social media, doxing, and false accusations about my personal and professional life. You name it. And I endured…I considered it the dark side of defending Science and Truth.
In April of 2019, I was invited to represent my country´s Medical College in a debate about pseudoscience on television, prime time. I was very excited and emotion clouded my reason. I didn´t think about the consequences. And well, it was a shitshow.
The audience was dominated by alternative health practitioners. The moderator was sympathetic with alternative health practices. And of course, the people representing the alternative health practitioners didn’t play by the same rules. They used deception, lying, testimonials, and all the logical fallacies you can think of.
But what really took me over the hedge was a Traditional Chinese Medicine Practitioner with connections to the Chinese Government, a constant presence in the mainstream media, that started to sell “acupuncture anesthesia” as something valid. Talking about how he, more than 20 years ago, used this practice to help perform surgical procedures. For me, that was a disrespect for all the people that suffered at the hands of Mao´s Chinese dictatorship. All the people that suffered excruciating pain, being operated on without general anesthesia only to sell East Snake Oil to the West. The “miracle” of acupuncture and Eastern medicine. The propaganda.
We exchanged words in the debate and that continued into social media. In the days after, I was called everything you can imagine by the defenders of alternative therapies. And this man took the opportunity to write that I was “short, ugly and bald” and that I have an “inferiority complex” because of that. That I´m a lousy doctor that cannot compete with his clinics. That only a masochist woman would want something with me.
But I endured. I could not stop feeling disgusted by the lack of shame of these people. I could not let go. Like Gaad Sad, I feel physical pain when someone is bullshitting. It makes me physically sick that people can say outrageous things with a serious face.
So, I wrote a blog post to explain the myth and the horror of acupuncture anesthesia and to dismantle other claims said by that man, like “all babies born with fire in the
liver…if you treat that problem, you can prevent infertility and cancer metastasis in the future!”. Preventing metastasis of a non-existing cancer… And I used a lot of adjectives: dumb, ignorant, charlatan, and snake oil salesman.
In November of 2019, this man goes to a wannabe Joe Rogan show and tells all sort of outrageous things like “Chinese people are so many because Traditional Chinese Medicine was very advanced for those days” or “until recently Traditional Chinese Medicine was more effective treating cancer than Conventional Medicine” or “Homeopathy works but they don´t want you to know…see this Documentary”. Again, I used sarcasm, irony, and a lot of adjectives.
And then, legal problems…
Soon after I wrote this last blog post, I received a letter from the court saying that I was being sued by this man. I hired a lawyer and made a lengthy response to all the accusations, more than 100 pages. Nevertheless, I have been charged with seventeen defamation crimes, awaiting trial, for defending the truth. For defending the people that Institutions refused to defend.
My country, Portugal, legally recognizes “Non-Conventional Therapies” like Homeopathy, Acupuncture, Traditional Chinese Medicine, Osteopathy, Chiropractic, and Naturopathy. My country, instead of defending the consumer, took the option to give these people the legal right of robbing people. I thought that the COVID-19 pandemic would change that a little bit since pseudoscience contributed zero for solving the problem, alternative practitioners embraced negationism about COVID-19, and Traditional Chinese Medicine was put in the corner. It was Science that came to the rescue with vaccines.
But now, when the pandemic is finally getting managed in my country, the snakes are starting to come out of hibernation to sell snake oil. And the media are giving them credit, again, like nothing has happened…nothing has changed, except for me.
Right now, I face four legal battles, for defamation. Besides this man, I have another lawsuit from a Nurse that promotes Reiki and Traditional Chinese Medicine, other from a Naturopath/Quantum Doctor and, lastly, from a Medical Doctor that was the head of the “Doctors For the Truth”, an organization part of an international network of Health Professionals that still denies the science about COVID-19.
So, this is my prize for all the hours battling liars and charlatans. The regulatory institutions don´t care. The mainstream media and Social Media don´t care. They are like brokers. They always win no matter if the stock market goes up or down. They will use you just to fuel the battle between science and pseudoscience and make money out of it. Why do you think the “Disinformation Dozen” still exists, besides some gestures of goodwill by the Social Media giants?
What I learned and you should learn…
I learned that it is pointless trying to convince people to change their minds on social media… People don´t follow reason, follow emotion, and something closer to religious belief. People want to be right, don´t want to learn what is right. Facts don´t change the minds of believers.
I learned that “True Skeptics” are unicorns. Everyone is a rational, skeptical person that values truth, reason, and science until you hit some nerve, some irrational belief that they hold dear. And then the “skepticism” goes down the drain. The more topics you talk about, the lonely you will be. And then you became a unicorn or, in the words of Malcolm Gladwell in the book “Talking to Strangers”, a Holy Fool: the truth-teller that is an outcast.
The COVID-19 pandemic just made things a lot worse…People started to getting hit by the pandemic in their quality of life and you start seeing hardcore skeptics doubting the most basic science and common sense. You even see some of your personal heroes like John Ioannidis going down the rabbit hole. Making the same basic mistakes that he spent his life point out about science production!
You start to see the animal inside us taking ground, what William James argued: if something improves your chances of survival, is not that the “truth”? The pragmatic, utilitarian truth? We saw irrationality in all its splendor, people negating reality, trying to conserve their way of life, making sense of events they don´t control. Fighting for control. Reason went to sleep and a lot of skeptics ceased to be…
So, I came to ask for your help… After two years of enduring the Sword of Damocles over my head, the energy to continue is running out. The SLAPP (Strategic lawsuit against public participation) they call it, is making a dent in my will to continue to fight against irrationality and charlatans.
So, I came to ask for your help, the International Skeptic community, for covering the legal expenses. I already asked for the support of my country’s skeptical community but it was not enough…only after two years of this marathon probably will take another two, I took this decision. I´m not proud of this, I´m angry that these people, besides robbing the sick and fragile giving them false hope are now making those who fight them spend money and probably pay “compensation” for not be silent about charlatanism. You can support me through Paypal or Patreon. Thank you in advance and I will keep you up-to-date.
PS
You can donate to PayPal:
By guest blogger Michael Scholz
For several years, the “flower essences” invented by Dr. Edward Bach had a difficult time in the European Union and especially Germany. The manufacturers were regularly taken to court for violating the EU Health Claim Regulation. This now culminates in the fact that the manufacturer, Nelsons, who sells the “Original Bach Flowers” in Germany, was forced to rename its popular “Rescue” remedies.
What happened?
The “Rescue” remedies were promoted with statements such as “calm and strong through the day” and “recommended use in emotionally exciting situations, e.g. at work” or to “face emotional challenges”. The competitor, Annoyax Nutripharm, regarded this as a health-related statement that is prohibited according to the EU Health Claim Regulation. Since the “Bach Flower Remedies” are not considered to be medicinal products in Germany, they are treated as food supplements, according to a ruling by the Oberlandesgericht (Higher Regional Court) Hamburg in 2007.
As it is strictly forbidden to advertise food supplements with health-related claims that are unproven, Annoyax Nutripharm filed a lawsuit against Nelsons that all the way to the Bundesgerichtshof (Federal High Court of Justice) in Karlsruhe. Since the case concerned European law, the judges in Karlsruhe referred it to the European Court of Justice in Luxemburg.
The judges wanted two questions clarified: 1. Are the “Rescue” remedies to be regarded simply as Brandy due to their alcohol content of 27%? (in which case, health-related claims would be strictly forbidden). 2. Does the product’s name “Rescue” itself constitute a violation of the Health Claims Regulation?
The Luxemburg judges ruled “No” and “Yes”. “No”, it is not Brandy, although the „essences“ consist of a considerable quantity of alcohol, the recommended dose is too small to be intoxicating. But “Yes”, the term “Rescue” does indeed violate the Health Claim Regulation. So the plaintiff won – and what is the result?
When the Health Claims Regulation was enacted in 2005, a transition period until 2022 was established. This applied to all products that were sold using the same brand name and composition before 2005. This now gave the defendant – Nelsons – the opportunity to use Edward Bach’s 135th anniversary for launching an advertising campaign that praises the court-ordered renaming as „modernization“ for the 21st century. And as you see, the new name is a paragon of creativity, innovation & modernism, indeed (//irony:off): “Rescue” becomes – drum roll – “Rescura”. Yes, I looked just like that too…
This pyrrhic victory for the plaintiffs shows how important it is to protect the European citizens against misleading advertising. And – far more important – it is now established through a ruling of the Federal High Court of Justice that “Bach Flowers” are an esoterical concept devoid of medical evidence.
This amazing announcement reached me via Twitter. It seems that the people in the AYUSH ministry are highly delusional. According to Wikipedia, the Ministry of Ayurveda, Yoga, Naturopathy, Unani, Siddha, Sowa-Rigpa and Homoeopathy (abbreviated as AYUSH) is purposed with developing education, research and propagation of indigenous alternative medicine systems in India. As per a recent notification published in the Gazette of India on 13 April 2021, the Ministry of AYUSH (Ayurveda, Yoga & Naturopathy, Unani, Siddha and Homoeopathy), will now be known as the Ministry of Ayush.
India is suffering from a very severe health crisis, and the ministry should stop its propaganda for useless solutions.
- Ayurveda,
- Homeopathy (considered to be indigenous in India),
- Yoga,
- Naturopathy,
- Unani,
- Sidda,
- Sowa-Rigpa (the traditional medicine of Tibet)
have in common that they can offer very little help to patients infected by COVID-19. In view of this fact, the announcement is ununderstandable and irresponsible, in my view.
Vaccinations lead to masturbation! This surprising claim comes from Zita Schwyter, a Swiss anti-vaxxer, and practitioner of so-called alternative medicine (SCAM). Is there any evidence for a link? The only evidence I could find seems to suggest that the causal link (if there is one) goes in the opposite direction: “Women engaging in mutual masturbation were nearly two times more likely to decline the free vaccine.”
In her practice, Schwyter offers homeopathic treatments, hara massage, “vaccination consultations”, quantum medicine, ‘Matrix Energetics’, colon cleansing, and other SCAMs. Schwyter claims that vaccinations cause “vaccination disease” with symptoms such as sleep disorders, dyslexia, stuttering, autism, brain tumors, the tendency to masturbate, allergic reactions, cancer, swelling and redness at the injection site, or aching limbs. According to Zita Schwyter, chronic diseases and autoimmune diseases have only been on the rise since vaccination was introduced, and that, according to her fallacious thinking, implies a causal relationship.
On the website of her practice, Schwyter tells us that “Fühlen Sie sich in guten Händen und vertrauen Sie Ihre Gesundheit der ganzheitlichen Gemeinschaftspraxis vor Ort an. Ein professionelles Therapeutenteam mit einem fundierten Fachwissen, jahrelangen Ausbildungen und weitreichenden Erfahrungen erwartet Sie.” (Feel in good hands and entrust your health to the holistic group practice on site. A professional team of therapists with in-depth expertise, years of training and extensive experience awaits you.) And elsewhere, she states that “Durch meine berufliche Laufbahn verstehe ich mich deshalb als kompetentes Bindeglied zwischen Schulmedizin und Naturheilkunde, spezialisiert auf dem Gebiet der Homöopathie. Die richtige Person also, die Ihre Beschwerden ganzheitlich erfassen, richtig interpretieren und Sie mit dem angemessenen Behandlungskonzept zu besserer Gesundheit führen kann.” (Through my professional career, I therefore see myself as a competent link between conventional medicine and naturopathy, specializing in the field of homeopathy. The right person, therefore, who can grasp your complaints holistically, interpret them correctly and lead you to better health with the appropriate treatment concept.)
Homeopathy, Schwyter claims on the same site, can effectively treat the following conditions:
- Joint pain
- Rheumatism
- Gout
- Allergies
- Neurodermatitis,
- Acne
- Shingles
- Asthma
- Hay fever
- Varicose veins
- Reynauds syndrome
- Gynecological diseases
- Pregnancy pains
- Migraine
- Chronic headache
- Diarrhea
- Constipation
- Chronic bowel inflammation
- Epilepsy
- Multiple sclerosis
- Parkinson’s disease
- High blood pressure
- Dizziness
- Diabetes mellitus
- Metabolic disorders
- Liver/gall bladder problems
- Acute and chronic childhood diseases
- Growth and development disorders in children
- Susceptibility to infections
- Flu
- Otitis media
- Coughing
- Convalescence from acute diseases
- Chronic injury sequelae
- Sleep disorders
- Learning difficulties
- Exhaustion
- Nervousness
- Depression
- Anxiety
- Obsessive-compulsive disorders
- Diseases resistant to conventional medicine
- And much more
Call me a skeptic, but somehow, I doubt Schwyter’s competence, expertise, and professionalism. But I do admire her humor!
I have reported about the risks of chiropractic manipulation many times before. This is not because, as some seem to believe, I have an axe to grind but because the subject is important. This week, another case of stroke after chiropractic manipulation was in the news. Some will surely say that it is alarmist to mention such reports which lack lots of crucial details. Yet, as long as chiropractors do not establish a proper monitoring system where serious adverse effects of spinal manipulation are noted, I think it is important to record even incomplete cases in this fashion.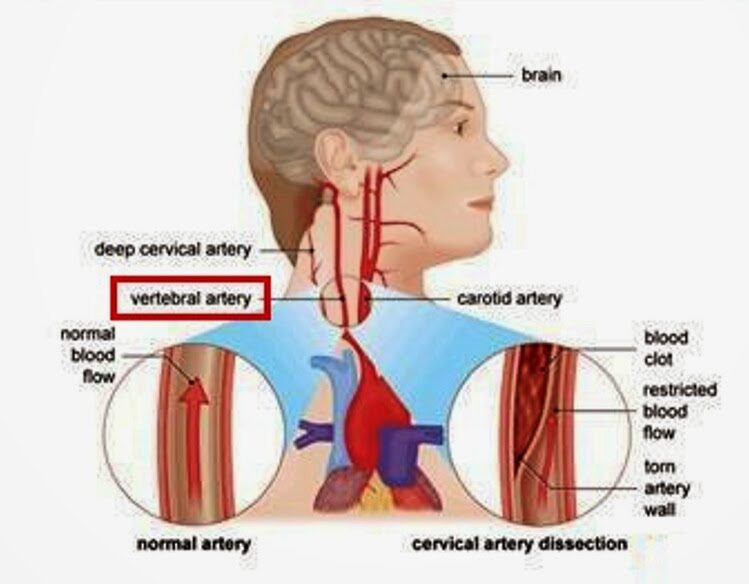
Barbara Shand is a working mom who lives in Alberta, Canada. She went to see a chiropractor because she had neck pain. “Near the very end of the appointment, the chiropractor asked: ‘Do you want your neck adjusted?’ I said: ‘Sure.’” “As soon as she did it, everything went black,” Shand recalls.
The patient was then rushed to a hospital by ambulance. “When I did open my eyes, I couldn’t focus. It was all blurry, I had massive vertigo, I didn’t know what was up or down,” Shand told the journalist. The diagnosis, Shand explains, was a right vertebral artery dissection, followed by a stroke. Mrs. Sands continues to struggle with coordination and balance.
The Alberta College and Association of Chiropractors acknowledges “there have been reported cases of stroke associated with visits to various healthcare practitioners, including those that provide cervical spine manipulation.” But they claim it is rare. They did not comment on the informed consent which, according to Shand’s description, was more than incomplete.
The fact that the ACAC admits that such events have happened before is laudable and a step in the right direction (some chiropractic organizations don’t even go that far). Yet, their caveat that such cases are rare is problematic. Without a monitoring system, nobody can tell how frequent they are! What we do see is merely the tip of a much bigger iceberg. There have been hundreds of cases like Mrs. Shand. The truth of the matter is this: Chiropractic neck manipulations are not supported by sound evidence of effectiveness for any condition. This means that even rare risks (if they are truly rare) would tilt the risk/benefit balance into the negative.
The conclusion is, I think, to avoid neck manipulations at all costs. Or, as one neurologist once put it:
don’t let the buggars touch your neck!
‘CLAMP DOWN ON THE BOGUS SCIENCE OF HOMEOPATHY’ is the title of a comment by Oliver Klamm in The Times today. Here is the background to his article.
In September 2020, the website of Homeopathy UK, www.homeopathy-uk.org, featured a page titled “Conditions Directory” with text that stated “Please find below a list of conditions where homeopathy can help …” followed by a list of medical conditions that included depression, diabetes, infertility, psoriasis and asthma. When consumers clicked-through the links to the conditions listed on that page, they were taken to separate pages for each that contained anecdotal descriptions from doctors detailing how they had applied homeopathic methods to the relevant conditions.
The UK Advertising Standards Authority received a complainant that challenged whether the ad discouraged essential treatment for conditions for which medical supervision should be sought, namely depression, diabetes, infertility, psoriasis and asthma.
The response of ‘Homeopathy UK’ said that, as a registered charity, they sought to share information about homeopathy for the benefit of others, rather than for commercial gain, and that they would always recommend that patients seeking homeopathic care did so under the supervision of a qualified medical practitioner…
The ASA upheld the complaint and argued as follows:
The CAP Code required that marketers must not discourage essential treatment for conditions for which medical supervision should be sought. For example, they must not offer specific advice on, diagnosis or treatment for such conditions unless that advice, diagnosis or treatment was conducted under the supervision of a suitably qualified medical professional. The ad referred to “depression”, “diabetes”, “infertility”, “psoriasis” and “asthma”, which we considered were conditions for which medical supervision should be sought. Any advice, diagnosis or treatment, therefore, must be conducted under the supervision of a suitably qualified medical professional. We acknowledged that the articles had been written by GMC-registered doctors, who we considered would be suitably qualified to offer advice, diagnosis or treatment. However, we noted that the ad and the articles to which it linked referred to homeopathy in general, rather than treatment by a specific individual. We understood that there were no minimum professional qualifications required to practice homeopathy, which could result in consumers being advised, diagnosed, or treated for the conditions listed in the ad by a practitioner with no medical qualification. We therefore considered Homeopathy UK would not be able to demonstrate that all such treatment would be conducted under the supervision of a suitably qualified health professional.
Furthermore, we understood that, although elsewhere on the website there were links to specific clinics, not all treatment would be conducted under the supervision of a suitably qualified health professional across those clinics. Because Homeopathy UK had not supplied evidence that treatment would always be carried out by a suitably qualified health professional. Also, because reference to the conditions listed in the ad, and discussed in the related articles, could discourage consumers from seeking essential treatment under the supervision of a suitably qualified health professional, we concluded that the ad had breached the Code.
On that point the ad breached CAP Code (Edition 12) rule 12.2 (Medicines, medical devices, health-related products and beauty products).
The ad must not appear again in the form complained about. We told Homeopathy UK to ensure their future marketing communications did not to refer to conditions for which advice should be sought from suitably qualified health professionals.
___________________________
Depression, diabetes, and asthma have few things in common. Just two characteristics stand out, in my view:
- they are potentially fatal;
- homeopathy is ineffective in changing their natural history.
- It was therefore high time that the ASA stopped this criminally dangerous nonsense of deluded homeopaths.
The article by Oliver Klamm concludes with the following wise words about homeopathy:
“For public officials and opinion formers, the time for appeasing this dangerous quackery should be long past.”
I have not often seen a paper reporting a small case series with such an impressively long list of authors from so many different institutions:
- Hospital of Lienz, Lienz, Austria.
- WissHom: Scientific Society for Homeopathy, Koethen, Germany; Umbrella Organization for Medical Holistic Medicine, Vienna, Austria; Vienna International Academy for Holistic Medicine (GAMED), Otto Wagner Hospital Vienna, Austria; Professor Emeritus, Medical University of Vienna, Department of Medicine I, Vienna, Austria. Electronic address: [email protected].
- Resident Specialist in Hygiene, Medical Microbiology and Infectious Diseases, Außervillgraten, Austria.
- St Mary’s University, London, UK.
- Umbrella Organization for Medical Holistic Medicine, Vienna, Austria.
- Shaare Zedek Medical Center, The Center for Integrative Complementary Medicine, Jerusalem, Israel.
- Apotheke Zum Weißen Engel – Homeocur, Retz, Austria.
- Reeshabh Homeo Consultancy, Nagpur, India.
- Umbrella Organization for Medical Holistic Medicine, Vienna, Austria; Vienna International Academy for Holistic Medicine (GAMED), Otto Wagner Hospital Vienna, Austria; Chair of Complementary Medicine, Medical Faculty, Sigmund Freud University Vienna, Austria; KLITM: Karl Landsteiner Institute for Traditional Medicine and Medical Anthropology, Vienna, Austria.
- WissHom: Scientific Society for Homeopathy, Koethen, Germany.
In fact, there are 12 authors reporting about 13 patients! But that might be trivial – so, let’s look at the paper itself. The aim of this study was to describe the effect of adjunctive individualized homeopathic treatment delivered to hospitalized patients with confirmed symptomatic SARS-CoV-2 infection.
Thirteen patients with COVID-19 were admitted. The mean age was 73.4 ± 15.0 (SD) years. The treating homeopathic doctor was instructed by the hospital on March 27, 2020, to adjunctively treat all inpatient COVID-19 patients homeopathically. The high potency homeopathic medicinal products were administered orally. Five globules were administered sublingually where they dissolved, three times a day. In ventilated patients in the ICU, medication was administered as a sip from a water beaker or 1 ml three times a day using a syringe. All ventilated patients exhibited dry cough resulting in respiratory failure. They were given Influenzinum, as were the patients at the general inpatient ward.
Twelve patients (92.3%) were speedily discharged without relevant sequelae after 14.4 ± 8.9 days. A single patient admitted in an advanced stage of septic disease died in the hospital. A time-dependent improvement of relevant clinical symptoms was observed in the 12 surviving patients. Six (46.2%) were critically ill and treated in the intensive care unit (ICU). The mean stay at the ICU of the 5 surviving patients was 18.8 ± 6.8 days. In six patients (46.2%) gastrointestinal disorders accompanied COVID-19.
The authors conclude that adjunctive homeopathic treatment may be helpful to treat patients with confirmed COVID-19 even in high-risk patients especially since there is no conventional treatment of COVID-19 available at present.
In the discussion section of the paper, the authors state this: “Given the extreme variability of pathology and clinical manifestations, a single universal preventive homeopathic medicinal product does not seem feasible. Yet homeopathy may have a relevant role to play precisely because of the number and diversity of its homeopathic medicinal products which can be matched with the diversity of the presentations. Patients with mild forms of disease can use homeopathic medicinal products at home using our simple algorithm. As this Case series suggests, adjunctive homeopathic treatment can play a valuable role in more serious presentations. For future pandemics, homeopathy agencies should be prepared by establishing rapid-response teams and efficacious lines of communication.”
There is nothing in this paper that would lead me to conclude that the homeopathic remedies had a positive effect on the natural history of the disease. All this article actually does do is this: it provides a near-perfect insight into the delusional megalomania of some homeopaths. These people are even more dangerous than I had feared.
The aim of this “multicenter cross-sectional study” was to analyze a cohort of breast (BC) and gynecological cancers (GC) patients regarding their interest in, perception of, and demand for integrative therapeutic health approaches.
The BC and GC patients were surveyed at their first integrative clinic visit using validated standardized questionnaires. Treatment goals and potential differences between the two groups were evaluated.
A total of 340 patients (272 BC, 68 GC) participated in the study. The overall interest in IM was 95.3% and correlated with older age, recent chemotherapy, and higher education. A total of 89.4% were using integrative methods at the time of enrolment, primarily exercise therapy (57.5%), and vitamin supplementation (51.4%). The major short-term goal of the BC patients was a side-effects reduction of conventional therapy (70.4%); the major long-term goal was the delay of a potential tumor progression (69.3%). In the GC group, major short-term and long-term goals were slowing tumor progression (73.1% and 79.1%) and prolonging survival (70.1% and 80.6%). GC patients were significantly more impaired by the side-effects of conventional treatment than BC patients [pain (p = 0.006), obstipation (< 0.005)].
The authors concluded that these data demonstrate a high overall interest in and use of IM in BC and GC patients. This supports the need for specialized IM counseling and the implementation of integrative treatments into conventional oncological treatment regimes in both patient groups. Primary tumor site, cancer diagnosis, treatment phase, and side effects had a relevant impact on the demand for IM in our study population.
This paper is, in my mind, an excellent example of pseudo-research:
- The ‘study’ turns out to be little more than a survey.
- The sample is small and not representative; therefore the findings cannot be generalized and are meaningless.
- The patients surveyed are those who decided to attend clinics of integrative medicine.
- These patients had used alternative therapies before and are evidently in favor of alternative medicine.
- The most frequently used alternative therapies (exercise, vitamins, trace elements, massage, lymph drainage) are arguably conventional treatments in Germany where the survey was conducted.
I have repeatedly commented on the plethora of useless surveys in so-called alternative medicine (SCAM). But this one might beat them all in its uselessness. The fact that close to 100% of patients attending clinics of integrative medicine are interested in SCAM and use some form of SCAM says it all, I think.
Why do people waste their time on such pseudo-research?
The best answer to this question is that it can be used for promotion. I found the paper by reading what seems to be a press release entitled: “Eine Studie bestätigt Patientenwunsch nach naturheilkundlicher Unterstützung”. This translates into “a study confirms the wish of patients for naturopathic support”. Needless to explain that the survey did not even remotely show this to be true.
What will they think of next?
I suggest a survey run in a BC clinic which amazingly discovers that nearly 100% of all patients are female.
Neuropathic pain is difficult to treat. Luckily, we have acupuncture! Acupuncturists leave us in no doubt that their needles are the solution. But are they correct or perhaps victims of wishful thinking?
This review was aimed at determining the proportion of patients with neuropathic pain who achieve a clinically meaningful improvement in their pain with the use of different pharmacologic and nonpharmacologic treatments.
Randomized controlled trials were included that reported a responder analysis of adults with neuropathic pain-specifically diabetic neuropathy, postherpetic neuralgia, or trigeminal neuralgia-treated with any of the following 8 treatments: exercise, acupuncture, serotonin-norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), topical rubefacients, opioids, anticonvulsant medications, and topical lidocaine.
A total of 67 randomized controlled trials were included. There was moderate certainty of evidence that anticonvulsant medications (risk ratio of 1.54; 95% CI 1.45 to 1.63; number needed to treat [NNT] of 7) and SNRIs (risk ratio of 1.45; 95% CI 1.33 to 1.59; NNT = 7) might provide a clinically meaningful benefit to patients with neuropathic pain. There was low certainty of evidence for a clinically meaningful benefit for rubefacients (ie, capsaicin; NNT = 7) and opioids (NNT = 8), and very low certainty of evidence for TCAs. Very low-quality evidence demonstrated that acupuncture was ineffective. All drug classes, except TCAs, had a greater likelihood of deriving a clinically meaningful benefit than having withdrawals due to adverse events (number needed to harm between 12 and 15). No trials met the inclusion criteria for exercise or lidocaine, nor were any trials identified for trigeminal neuralgia.
The authors concluded that there is moderate certainty of evidence that anticonvulsant medications and SNRIs provide a clinically meaningful reduction in pain in those with neuropathic pain, with lower certainty of evidence for rubefacients and opioids, and very low certainty of evidence for TCAs. Owing to low-quality evidence for many interventions, future high-quality trials that report responder analyses will be important to strengthen understanding of the relative benefits and harms of treatments in patients with neuropathic pain.
This review was published in a respected mainstream journal and conducted by a multidisciplinary team with the following titles and affiliations:
- Associate Professor in the College of Pharmacy at the University of Manitoba in Winnipeg.
- Pharmacist in Edmonton, Alta, and Clinical Evidence Expert for the College of Family Physicians of Canada.
- Family physician and Assistant Professor at the University of Alberta.
- Family physician and Associate Professor in the Department of Family Medicine at the University of Alberta.
- Pharmacist, Clinical Evidence Expert Lead for the College of Family Physicians of Canada, and Associate Clinical Professor in the Department of Family Medicine at the University of Alberta.
- Pharmacist in Edmonton and Clinical Evidence Expert for the College of Family Physicians of Canada.
- Pharmacist and Clinical Evidence Expert at the College of Family Physicians of Canada.
- Family physician, Director of Programs and Practice Support at the College of Family Physicians of Canada, and Adjunct Professor in the Department of Family Medicine at the University of Alberta.
- Professor in the Faculty of Pharmaceutical Sciences at the University of British Columbia in Vancouver.
- Pharmacist at the CIUSSS du Nord-de-l’lle-de-Montréal and Clinical Associate Professor in the Faculty of Pharmacy at the University of Montreal in Quebec.
- Care of the elderly physician and Assistant Professor in the Department of Family Medicine at the University of Alberta.
- Family physician and Professor in the Department of Family Medicine at the University of Alberta.
- Assistant Professor in the Department of Family Medicine at Queen’s University in Kingston, Ont.
- Research assistant at the University of Alberta.
- Medical student at the University of Alberta.
- Nurse in Edmonton and Clinical Evidence Expert for the College of Family Physicians of Canada.
As far as I can see, the review is of sound methodology, it minimizes bias, and its conclusions are therefore trustworthy. They suggest that acupuncture is not effective for neuropathic pain.
But how can this be? Do the authors not know about all the positive evidence on acupuncture? A quick search found positive recent reviews of acupuncture for all of the three indications in question:
- Diabetic neuropathy: Acupuncture alone and vitamin B combined with acupuncture are more effective in treating DPN compared to vitamin B.
- Herpes zoster: Acupuncture may be effective for patients with HZ.
- Trigeminal neuralgia: Acupuncture appears more effective than pharmacotherapy or surgery.
How can we explain this obvious contradiction?
Which result should we trust?
Do we believe pro-acupuncture researchers who published their papers in pro-acupuncture journals, or do we believe the findings of researchers who could not care less whether their work proves or disproves the effectiveness of acupuncture?
I think that these papers offer an exemplary opportunity for us to study how powerful the biases of researchers can be. They also remind us that, in the realm of so-called alternative medicine (SCAM), we should always be very cautious and not accept every conclusion that has been published in supposedly peer-reviewed medical journals.
The UK ‘Advertising Standards Authority‘ (ASA) received a complaint about an advertisement that stated:
“Homeopathy is used throughout the world to keep healthy … People in the UK have been using it to successfully help with migraine, anxiety, chronic pain, woman’s [sic] health issues, depression, eczema, chronic fatigue, asthma, IBS, rheumatoid arthritis, and many other conditions”.
The ‘Good Thinking Society‘ had challenged whether:
- the ad discouraged essential treatment for conditions for which medical supervision should be sought, namely migraines, chronic pain, women’s health issues, depression, asthma, rheumatoid arthritis; and
- the claim “People in the UK have been using [homeopathy] to successfully help with anxiety, chronic pain … eczema, chronic fatigue syndrome … IBS” was misleading and could be substantiated.
The response of the ASA has just been published. Here are the key excerpts from the ASA’s assessment:
1. Upheld
The CAP Code required that marketers must not discourage essential treatment for conditions for which medical supervision should be sought. For example, they must not offer specific advice on, diagnosis or treatment for such conditions unless that advice, diagnosis or treatment was conducted under the supervision of a suitably qualified medical professional. Among other conditions, the ad referred to “migraines”, “chronic pain”, “woman’s [sic] health issues”, “depression”, “asthma”, and “rheumatoid arthritis”, which we considered were conditions for which medical supervision should be sought, and therefore advice, diagnosis or treatment must be conducted under the supervision of a suitably qualified medical professional. We noted that the practice was run by a GMC-registered GP, who we considered was a suitably qualified health professional. However, the individual homeopaths were not registered and did not hold the same qualifications. Therefore, Homeopathy UK had not shown that all treatment and diagnoses conducted at the practice would be conducted under the supervision of a suitably qualified medical professional. Because Homeopathy UK had not supplied evidence that treatment would always be carried out by a suitably qualified health professional, and because reference to the conditions listed in the ad could discourage consumers from seeking essential treatment under the supervision of a suitably qualified health professional, we concluded that the ad had breached the Code.
On that point the ad breached CAP Code (Edition 12) rule 12.2 (Medicines, medical devices, health-related products and beauty products).
2. Upheld
We considered that consumers would understand the claim “People in the UK have been using [homeopathy] to successfully help with anxiety, chronic pain … eczema, chronic fatigue syndrome … IBS” to mean that homeopathy could be used to successfully treat those conditions … when we reviewed the evidence provided by Homeopathy UK, we considered that the studies provided did not meet the standard of evidence we required for the types of claims being made, both in terms of adequacy and relevance…
On that point the ad breached CAP Code (Edition) rules 3.1 (Misleading advertising), 3.7 (Substantiation) and 12.1 (Medicines, medical devices, health-related products and beauty products).
Action
The ad must not appear again in the form complained about. We told Homeopathy UK to ensure their future marketing communications did not to refer to conditions for which advice should be sought from suitably qualified health professionals. We also told them to ensure they did not make claims for homeopathy unless they were supported with robust evidence.
_____________________________
Am I reading this correctly?
The ASA seems to be saying that homeopaths are not suitably qualified health professionals and, as no therapeutic claims are supported by robust evidence, that claims for homeopathy are improper.

