Chinese studies
Whenever a journalist wants to discuss the subject of acupuncture with me, he or she will inevitably ask one question:
DOES ACUPUNCTURE WORK?
It seems a legitimate, obvious and simple question, particularly during ‘Acupuncture Awareness Week‘, and I have heard it hundreds of times. Why then do I hesitate to answer it?
Journalists – like most of us – would like a straight answer, like YES or NO. But straight answers are in short supply, particularly when we are talking about acupuncture.
Let me explain.
Acupuncture is part of ‘Traditional Chinese Medicine’ (TCM). It is said to re-balance the life forces that determine our health. As such it is seen as a panacea, a treatment for all ills. Therefore, the question, does it work?, ought to be more specific: does it work for pain, obesity, fatigue, hair-loss, addiction, anxiety, ADHA, depression, asthma, old age, etc.etc. As we are dealing with virtually thousands of ills, the question, does it work?, quickly explodes into thousands of more specific questions.
But that’s not all!
The question, does acupuncture work?, assumes that we are talking about one therapy. Yet, there are dozens of different acupuncture traditions and sites:
- body acupuncture,
- ear acupuncture,
- tongue acupuncture,
- scalp acupuncture,
- etc., etc.
Then there are dozens of different ways to stimulate acupuncture points:
- needle acupuncture,
- electroacupuncture,
- acupressure,
- moxibustion,
- ultrasound acupuncture,
- laser acupuncture,
- etc., etc.
And then there are, of course, different acupuncture ‘philosophies’ or cultures:
- TCM,
- ‘Western’ acupuncture,
- Korean acupuncture,
- Japanese acupuncture,
- etc., etc.
If we multiply these different options, we surely arrive at thousands of different variations of acupuncture being used for thousands of different conditions.
But this is still not all!
To answer the question, does it work?, we today have easily around 10 000 clinical trials. One might therefore think that, despite the mentioned complexity, we might find several conclusive answers for the more specific questions. But there are very significant obstacles that are in our way:
- most acupuncture trials are of lousy quality;
- most were conducted by lousy researchers who merely aim at showing that acupuncture works rather that testing whether it is effective;
- most originate from China and are published in Chinese which means that most of us cannot access them;
- they get nevertheless included in many of the systematic reviews that are currently being published without non-Chinese speakers ever being able to scrutinise them;
- TCM is a hugely important export article for China which means that political influence is abundant;
- several investigators have noted that virtually 100% of Chinese acupuncture trials report positive results regardless of the condition that is being targeted;
- it has been reported that about 80% of studies emerging from China are fabricated.
Now, I think you understand why I hesitate every time a journalist asks me:
DOES ACUPUNCTURE WORK?
Most journalists do not have the patience to listen to all the complexity this question evokes. Many do not have the intellectual capacity to comprehend an exhaustive reply. But all want to hear a simple and conclusive answer.
So, what do I say in this situation?
Usually, I respond that the answer would depend on who one asks. An acupuncturist is likely to say: YES, OF COURSE, IT DOES! An less biased expert might reply:
IT’S COMPLEX, BUT THE MOST RELIABLE EVIDENCE IS FAR FROM CONVINCING.
The origin of coronavirus 2 (SARS-CoV-2) has been the subject of intense speculation and several conspiracy theories, not least amongst the enthusiasts of so-called alternative medicine. Now Australian scientists have attempted to identify the origin of the coronavirus 2 (SARS-CoV-2). As this is undoubtedly a most sensitive subject, let me show you the unadulterated abstract of their paper:
The origin of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is contentious. Most studies have focused on a zoonotic origin, but definitive evidence such as an intermediary animal host is lacking. We used an established risk analysis tool for differentiating natural and unnatural epidemics, the modified Grunow–Finke assessment tool (mGFT) to study the origin of SARS-COV-2. The mGFT scores 11 criteria to provide a likelihood of natural or unnatural origin. Using published literature and publicly available sources of information, we applied the mGFT to the origin of SARS-CoV-2. The mGFT scored 41/60 points (68%), with high inter-rater reliability (100%), indicating a greater likelihood of an unnatural than natural origin of SARS-CoV-2. This risk assessment cannot prove the origin of SARS-CoV-2 but shows that the possibility of a laboratory origin cannot be easily dismissed.
The somewhat clumsy wording harbours explosive potential. It is more likely that the pandemic was started by a laboratory accident than by a zoonosis. In this case, it would be man-made rather than natural. The authors of the paper do, however, caution that their analysis does not prove the origin of the coronavirus. They merely speak of likelihoods. Moreover, it seems important to stress that there is no scientific evidence that Sars-CoV-2 was deliberately developed as a biological warfare agent.
Will this paper put an end to speculation and conspiracy?
I doubt it!
There are many variations of acupuncture. Electroacupuncture (EA) and Laseracupuncture (LA) are but two examples both of which are commonly used. However, it remains uncertain whether LA is as effective as EA. This study aimed to compare EA and LA head to head in dysmenorrhea.
A crossover, randomized clinical trial was conducted. EA or LA was applied to selected acupuncture points. Participants were randomized into two sequence treatment groups who received either EA or LA twice per week in luteal phase for 3 months followed by 2-month washout, then shifted to other groups (sequence 1: EA > LA; sequence 2: LA > EA). Outcome measures were heart rate variability (HRV), prostaglandins (PGs), pain, and quality-of-life (QoL) assessment (QoL-SF12). We also compared the effect of EA and LA in low and high LF/HF (low frequency/high frequency) status.
43 participants completed all treatments. Both EA and LA significantly improved HRV activity and were effective in reducing pain (Visual Analog Scale [VAS]; EA: p < 0.001 and LA: p = 0.010) and improving QoL (SF12: EA: p < 0.001, LA, p = 0.017); although without intergroup difference. EA reduced PGs significantly (p < 0.001; δ p = 0.068). In low LF/HF, EA had stronger effects than LA in increasing parasympathetic tone in respect of percentage of successive RR intervals that differ by more than 50 ms (pNN50; p = 0.053) and very low-frequency band (VLF; p = 0.035).
The authors concluded that there is no significant difference between EA and LA in improving autonomic nervous system dysfunction, pain, and QoL in dysmenorrhea. EA is prominent in PGs changing and preserving vagus tone in low LF/HF; yet LA is noninvasive for those who have needle phobia. Whether LA is equivalent with EA and the mechanism warrants further study.
Looking at the affiliations of the authors, one might expect that they should be able to design a meaningful study:
- 1Division of Hemato-Oncology, Department of Internal Medicine, Branch of Zhong-Zhou, Taipei City Hospital, Taipei, Taiwan.
- 2Institute of Traditional Medicine, National Yang-Ming Chiao Tung University, Taipei, Taiwan.
- 3Department of Traditional Medicine, Branch of Yang-Ming, Taipei City Hospital, Taipei, Taiwan.
- 4Department of Traditional Medicine, Branch of Kunming, Taipei City Hospital, Taipei, Taiwan.
- 5Department of Gynecology and Obstetrics, Branch of Yang-Ming, Taipei City Hospital, Taipei, Taiwan.
Sadly, this assumption is evidently mistaken.
The trial certainly does not show what they claim and neither had it ever the chance to show anything relevent. A clinical trial is comparable to a mathematical equation. It can be solved, if it has one unkown; it cannot produce a result, if it has two unknowns.
The efficacy of EA and LA for dysmenorrhea are both unknown. A comparative study with two unknowns cannot produce a meaningful result. EA and LA did not both improve autonomic nervous system dysfunction, pain, and QoL in dysmenorrhea but most likely they both had no effect. What caused the improvement was not the treatment per se but the ritual, the placebo effect, the TLC or other non-specific factors. The maginal differences in other parameters are meaningless; they are due to the fact that – as an equivalence trial – the study was woefully underpowered and thus open to coincidental differences.
Clinical trials should be about contributing to our knowledge and not about contributing to confusion.
Motor aphasia is common among patients with stroke. Acupuncture is recommended by TCM enthusiasts as a so-called alternative medicine (SCAM) for poststroke aphasia, but its efficacy remains uncertain.
JAMA just published a study that investigated the effects of acupuncture on language function, neurological function, and quality of life in patients with poststroke motor aphasia.
The study was designed as a multicenter, sham-controlled, randomized clinical trial. It was conducted in 3 tertiary hospitals in China from October 21, 2019, to November 13, 2021. Adult patients with poststroke motor aphasia were enrolled. Data analysis was performed from February to April 2023.
Eligible participants were randomly allocated (1:1) to manual acupuncture (MA) or sham acupuncture (SA) groups. Both groups underwent language training and conventional treatments.
The primary outcomes were the aphasia quotient (AQ) of the Western Aphasia Battery (WAB) and scores on the Chinese Functional Communication Profile (CFCP) at 6 weeks. Secondary outcomes included WAB subitems, Boston Diagnostic Aphasia Examination, National Institutes of Health Stroke Scale, Stroke-Specific Quality of Life Scale, Stroke and Aphasia Quality of Life Scale–39, and Health Scale of Traditional Chinese Medicine scores at 6 weeks and 6 months after onset. All statistical analyses were performed according to the intention-to-treat principle.
Among 252 randomized patients (198 men [78.6%]; mean [SD] age, 60.7 [7.5] years), 231 were included in the modified intention-to-treat analysis (115 in the MA group and 116 in the SA group). Compared with the SA group, the MA group had significant increases in AQ (difference, 7.99 points; 95% CI, 3.42-12.55 points; P = .001) and CFCP (difference, 23.51 points; 95% CI, 11.10-35.93 points; P < .001) scores at week 6 and showed significant improvements in AQ (difference, 10.34; 95% CI, 5.75-14.93; P < .001) and CFCP (difference, 27.43; 95% CI, 14.75-40.10; P < .001) scores at the end of follow-up.
The authors concluded that in this randomized clinical trial, patients with poststroke motor
aphasia who received 6 weeks of MA compared with those who received SA demonstrated
statistically significant improvements in language function, quality of life, and neurological
impairment from week 6 of treatment to the end of follow-up at 6 months after onset.
I was asked by the SCIENCE MEDIC CENTRE to provide a short comment. This is what I stated:
Superficially, this looks like a rigorous trial. We should remember, however, that several groups, including mine, have shown that very nearly all Chinese acupuncture studies report positive results. This suggests that the reliability of these trials is less than encouraging. Moreover, the authors state that real acupuncture induced ‘de chi’, while sham acupuncture did not. This shows that the patients were not blinded and the outcomes might easily be due to a placebo response.
Here, I’d like to add two further points:
- We have learnt that the vast majority of research coming out of China is fabricated.
- I think it is lamentable that a journal of high standing is not more critical and repeatedly falls for such suspect acupuncture studies.
This study investigated whether Tongxinluo,a traditional Chinese medicine compound that has shown promise in in vitro, animal, and small human studies for myocardial infarction, could improve clinical outcomes in patients with ST-segment elevation myocardial infarction (STEMI). The randomized, double-blind, placebo-controlled clinical trial was conducted among patients with STEMI within 24 hours of symptom onset from 124 hospitals in China. Patients were enrolled from May 2019 to December 2020; the last date of follow-up was December 15, 2021.
Patients were randomized 1:1 to receive either Tongxinluo or placebo orally for 12 months. A loading dose of 2.08 g was given after randomization, followed by the maintenance dose of 1.04 g, 3 times a day, in addition to STEMI guideline-directed treatments. The primary end point was 30-day major adverse cardiac and cerebrovascular events (MACCEs), a composite of cardiac death, myocardial reinfarction, emergent coronary revascularization, and stroke. Follow-up for MACCEs occurred every 3 months to 1 year.
Among 3797 patients who were randomized, 3777 (Tongxinluo: 1889 and placebo: 1888; mean age, 61 years; 76.9% male) were included in the primary analysis. Thirty-day MACCEs occurred in 64 patients (3.4%) in the Tongxinluo group vs 99 patients (5.2%) in the control group. Individual components of 30-day MACCEs, including cardiac death, were also significantly lower in the Tongxinluo group than the placebo group. By 1 year, the Tongxinluo group continued to have lower rates of MACCEs and cardiac death. There were no significant differences in other secondary end points including 30-day stroke; major bleeding at 30 days and 1 year; 1-year all-cause mortality; and in-stent thrombosis. More adverse drug reactions occurred in the Tongxinluo group than the placebo group, mainly driven by gastrointestinal symptoms.
The authors concluded that in patients with STEMI, the Chinese patent medicine Tongxinluo, as an adjunctive therapy in addition to STEMI guideline-directed treatments, significantly improved both 30-day and 1-year clinical outcomes. Further research is needed to determine the mechanism of action of Tongxinluo in STEMI.
Tongxinluo is mixture of various active ingredients, including
- ginseng,
- leech,
- scorpion,
- Paeonia lactiflora,
- cicada slough,
- woodlouse bug,
- centipede,
- sandalwood.
With chaotic mixtures of this type, it is impossible to name all the potentially active ingredients, list their actions, or identify the ones that are truly relevant. According to the thinking of TCM proponents, this would also be the wrong way to go about it – such mixtures work as a whole, they would insist.
Tongxinluo is by no means a mixture that has not been studied before.
A previous systematic review of 12 studies found that Tongxinluo capsule is superior to conventional treatment in improving clinical overall response rate and hemorheological indexes and is relatively safe. Due to the deficiencies of the existing studies, more high-quality studies with rigorous design are required for further verification.
A 2022 meta-analysis indicated that the mixture had beneficial effects on the prevention of cardiovascular adverse events, especially in TVR or ISR after coronary revascularization and may possibly lower the incidence of first or recurrent MI and HF within 12 months in patients with CHD, while insufficient sample size implied that these results lacked certain stability. And the effects of TXLC on cardiovascular mortality, cerebrovascular events, and unscheduled readmission for CVDs could not be confirmed due to insufficient cases. Clinical trials with large-sample sizes and extended follow-up time are of interest in the future researches.
A further meta-analysis suggested beneficial effects on reducing the adverse cardiovascular events without compromising safety for CHD patients after PCI on the 6-month course.
Finally, a systematic review of 10 studies found that the remedy is an effective and safe therapy for CHD patients after percutaneous coronary interventions.
So, should we believe the new study with its remarkable findings? On the one hand, the trial seems rigorous and is reported in much detail. On the other hand, the study (as all previous trials of this mixture) originates from China. We know how important TCM is for that country as an export item, and we know how notoriously unreliable Chinese research sadly has become. In view of this, I would like to see an independent replication of this study by an established research group outside China before I recommend Tongxinluo to anyone.
Let’s not forget:
if it sound too good to be true, it probably is!
This systematic review aimed to assess the impact of Tai Chi on individuals with essential hypertension and to compare the effects of Tai Chi with other therapies. The researchers conducted a systematic literature search of the Medline, Scholar, Elsevier, Wiley Online Library, Chinese Academic Journal (CNKI) and Wanfang databases from January 2003 to August 2023. Using the methods of the Cochrane Collaboration Handbook, a meta-analysis was conducted to assess the collective impact of Tai Chi exercise in controlling hypertension. The primary outcomes measured included blood pressure and nitric oxide levels.
A total of 32 RCTs were included. The participants consisted of adults with an average age of 57.1 years who had hypertension (mean ± standard deviation systolic blood pressure at 148.2 ± 12.1 mmHg and diastolic blood pressure at 89.2 ± 8.3 mmHg). Individuals who practiced Tai Chi experienced reductions in systolic blood pressure of 10.6 mmHg, diastolic blood pressure of 4.7 mmHg and an increase in nitric oxide levels.
The authors concluded that Tai Chi can be a viable lifestyle intervention for managing hypertension. Greater promotion of Tai Chi by medical professionals could extend these benefits to a larger patient population.
Tai Chi allegedly incorporates principles rooted in the Yin and Yang theory, Chinese medicine meridians and breathing techniques, and creates a unique form of exercise characterized by its inward focus, continuous flow, the balance of strength and gentleness, and alternation between fast and slow movements. What sets Tai Chi apart from other forms of excercise is the requirement for mindful guidance during practice. This aspect may, according to the authors, be the reason why Tai Chi also outperforms general aerobic exercise in managing hypertension.
I can well imagine that any form of relaxation reduces blood pressure. What I find hard to believe is that Tai Chi is better than any other relaxing SCAMs. The 32 RCTs included in this new review fail to impress me because they are all from China, and – as we have often mentioned before – studies from China are to be taken with a pinch of salt.
Yet, the subject is important enough, in my view, to merit a few rigorous trials conducted by independent researchers. Until such data are available, I think, I prefer to rely on our own systematic review which conculded that the evidence for tai chi in reducing blood pressure … is limited. Whether tai chi has benefits over exercise is still unclear. The number of trials and the total sample size are too small to draw any firm conclusions.
Manual therapy is considered a safe and less painful method and has been increasingly used to alleviate chronic neck pain. However, there is controversy about the effectiveness of manipulation therapy on chronic neck pain. Therefore, this systematic review and meta-analysis of randomized controlled trials (RCTs) aimed to determine the effectiveness of manipulative therapy for chronic neck pain.
A search of the literature was conducted on seven databases (PubMed, Cochrane Center Register of Controlled Trials, Embase, Medline, CNKI, WanFang, and SinoMed) from the establishment of the databases to May 2022. The review included RCTs on chronic neck pain managed with manipulative therapy compared with sham, exercise, and other physical therapies. The retrieved records were independently reviewed by two researchers. Further, the methodological quality was evaluated using the PEDro scale. All statistical analyses were performed using RevMan V.5.3 software. The Grading of Recommendations, Assessment, Development and Evaluations (GRADE) assessment was used to evaluate the quality of the study results.
Seventeen RCTs, including 1190 participants, were included in this meta-analysis. Manipulative therapy showed better results regarding pain intensity and neck disability than the control group. Manipulative therapy was shown to relieve pain intensity (SMD = -0.83; 95% confidence interval [CI] = [-1.04 to -0.62]; p < 0.0001) and neck disability (MD = -3.65; 95% CI = [-5.67 to – 1.62]; p = 0.004). However, the studies had high heterogeneity, which could be explained by the type and control interventions. In addition, there were no significant differences in adverse events between the intervention and the control groups.
The authors concluded that manipulative therapy reduces the degree of chronic neck pain and neck disabilities.
Only a few days ago, we discussed another systematic review that drew quite a different conclusion: there was very low certainty evidence supporting cervical SMT as an intervention to reduce pain and improve disability in people with neck pain.
How can this be?
Systematic reviews are supposed to generate reliable evidence!
How can we explain the contradiction?
There are several differences between the two papers:
- One was published in a SCAM journal and the other one in a mainstream medical journal.
- One was authored by Chinese researchers, the other one by an international team.
- One included 17, the other one 23 RCTs.
- One assessed ‘manual/manipulative therapies’, the other one spinal manipulation/mobilization.
The most profound difference is that the review by the Chinese authors is mostly on Chimese massage [tuina], while the other paper is on chiropractic or osteopathic spinal manipulation/mobilization. A look at the Chinese authors’ affiliation is revealing:
- Department of Tuina and Spinal Diseases Research, The Third School of Clinical Medicine (School of Rehabilitation Medicine), Zhejiang Chinese Medical University, Hangzhou, China.
- Department of Tuina and Spinal Diseases Research, The Third School of Clinical Medicine (School of Rehabilitation Medicine), Zhejiang Chinese Medical University, Hangzhou, China; Department of Tuina, The Third Affiliated Hospital of Zhejiang Chinese Medical University, Hangzhou, China. Electronic address: [email protected].
- Department of Tuina and Spinal Diseases Research, The Third School of Clinical Medicine (School of Rehabilitation Medicine), Zhejiang Chinese Medical University, Hangzhou, China; Department of Tuina, The Third Affiliated Hospital of Zhejiang Chinese Medical University, Hangzhou, China. Electronic address: [email protected].
What lesson can we learn from this confusion?
Perhaps that Tuina is effective for neck pain?
No!
What the abstract does not tell us is that the Tuina studies are of such poor quality that the conclusions drawn by the Chinese authors are not justified.
What we do learn – yet again – is that
- Chinese papers need to be taken with a large pintch of salt. In the present case, the searches underpinning the review and the evaluations of the included primary studies were clearly poorly conducted.
- Rubbish journals publish rubbish papers. How could the reviewers and the editors have missed the many flaws of this paper? The answer seems to be that they did not care. SCAM journals tend to publish any nonsense as long as the conclusion is positive.
This study investigated the potential benefits of auricular point acupressure on cerebrovascular function and stroke prevention among adults with a high risk of stroke.
A randomized controlled study was performed with 105 adults at high risk for stroke between March and July 2021. Participants were randomly allocated to receive either
- auricular point acupressure with basic lifestyle interventions (n = 53) or
- basic lifestyle interventions alone (n = 52) for 2 weeks.
The primary outcome was the kinematic and dynamic indices of cerebrovascular function, as well as the CVHP score at week 2, measured by the Doppler ultrasonography and pressure transducer on carotids.
Of the 105 patients, 86 finished the study. At week 2, the auricular point acupressure therapy with lifestyle intervention group had higher kinematic indices, cerebrovascular hemodynamic parameters score, and lower dynamic indices than the lifestyle intervention group.
The authors concluded that ccerebrovascular function and cerebrovascular hemodynamic parameters score were greater improved among the participants undergoing auricular point acupressure combined with lifestyle interventions than lifestyle interventions alone. Hence, the auricular point acupressure can assist the stroke prevention.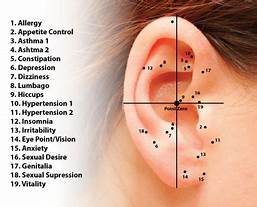
Acupuncture is a doubtful therapy.
Acupressure is even more questionable.
Ear acupressure is outright implausible.
The authors discuss that the physiological mechanism underlying the effect of APA therapy on cerebrovascular hemodynamic function is not fully understood at present. There may be two possible explanations.
- First, a previous study has demonstrated that auricular acupuncture can directly increase mean blood flow velocity in the middle cerebral artery.
- Second, cerebrovascular hemodynamic function is indirectly influenced by the effect of APA therapy on blood pressure.
I think there is a much simpler explanation: the observed effects are directly or indirectly due to placebo. As regular listeners of this blog know only too well by now, the A+B versus B study design cannot account for placebo effects. Sadly, the authors of this study hardly discuss this explanation – that’s why they had to publish their findings in just about the worst SCAM journal of them all: EBCAM.
Two years ago, I published a blog about the research activity in SCAM. To demonstrate the volume of SCAM research I looked into Medline to find the number of papers published in 2020 for the SCAMs listed below. Now I repeated the exercise for the year 2022. The respective 1st numbers below are those of 2020, and the second ones refer to 2022 (in bold):
- acupuncture 2 752 – 3,565
- anthroposophic medicine 29 – 28
- aromatherapy 173 – 205
- Ayurvedic medicine 183 – 249
- chiropractic 426 – 498
- dietary supplement 5 739 – 8,915
- essential oil 2 439 – 3,340
- herbal medicine 5 081 – 16,207
- homeopathy 154 – 212
- iridology 0 – 0
- Kampo medicine 132 – 176
- massage 824 – 996
- meditation 780 – 1,016
- mind-body therapies 968 – 1,616
- music therapy 539 – 716
- naturopathy 68 – 92
- osteopathic manipulation 71 – 85
- Pilates 97 – 152
- qigong 97 – 121
- reiki 133 – 158
- tai chi 397 – 470
- Traditional Chinese Medicine 15 277 – 22,586
- yoga 698 – 837
These data suggest the following:
- As before, the research activity in SCAM seems relatively low.
- Most numbers are pretty stable with a slight overall increase.
- The meager numbers for anthroposophic medicine, homeopathy, iridology, Kampo, and naturopathy are remarkable.
- In absolute terms, only acupuncture, dietary supplements, essential oil, herbal medicine, and TCM are impressive; by and large, these are areas where commercial interest and sponsors exist.
- The ‘big winners’ in terms of increase over time are acupuncture, supplements, essential oil, herbal medicine, and TCM; I suspect that much of this is due to the fast-growing (and repeatedly mentioned) influence that China is gaining in SCAM.
This systematic review and meta-analysis aimed to evaluate the effectiveness and safety of Chinese herbal medicine (CHM) combined with Western medicine (WM) in comparison with WM in reducing systolic and diastolic blood pressure for patients with primary hypertension (PHTN).
Various literature searches located a total of 29 studies that included 2623 patients. The results showed that the clinical effectiveness in the treatment of hypertension with CHM+WM was considerably higher than that with WM alone, clinical effective (RR 1.23, 95% CI [1.17, 1.30], P < 0.00001), and markedly effective (ME) in the patients (RR 1.66, 95% CI [1.52, 1.80], and P < 0.00001). Random effect in SBP (MD 7.91 mmHg,[6.00, 983], P < 0.00001) and DBP (MD 5.46 mmHg, [3.88, 6.43], P < 0.00001), a subgroup analysis was carried out based on the type of intervention, duration of treatment, and CHM formulas that showed significance. Furthermore, no severe side effects were reported, and no patients stopped treatment or withdrawal due to any severe adverse events.
The authors concluded that compared to WM alone, the therapeutic effectiveness of CHM combined with WM is significantly improved in the treatment of hypertension. Additionally, CHM with WM may safely and efficiently lower systolic blood pressure (SBP) and diastolic blood pressure (DBP) in individuals with PHTN. However, rigorous randomized controlled trials with a large sample, high quality, long duration of treatment, and follow-up are recommended to strengthen this clinical evidence.
The authors can boast of an impressive list of affiliations:
- 1Heilongjiang University of Chinese Medicine, Harbin, 150040, Heilongjiang, China; School of Pharmacy, Lebanese International University, 18644, Sana’a, Yemen.
- 2Heilongjiang University of Chinese Medicine, Harbin, 150040, Heilongjiang, China.
- 3Key Laboratory of Chinese Materia Medica, Ministry of Education of Heilongjiang University of Chinese Medicine, Harbin, 150040, Heilongjiang, China.
- 4Department of Urology, Affiliated Hospital of Qingdao Binhai University, Qingdao, Shandong, China.
- 5Department of Respiratory Diseases, Shandong Second Provincial General Hospital, Shandong University, Shandong, China.
- 6Heilongjiang University of Chinese Medicine, Harbin, 150040, Heilongjiang, China. Electronic address: [email protected].
Impressive in the sense of being impressively prone to bias, particularly knowing that ~80% of Chinese research findings have been shown to be fabricated and considering that Chinese authors as good as never publish anything negative about TCM.
But perhaps you still believe that the results reported here are 100% true? In this case, I might even agree with you. The reason is that the authors demonstrate in exemplary fashion what I have been saying so often before:
Blood pressure is one of the many endpoints that are highly prone to placebo effects. Therefore, even the addition of an ineffective CHM to WM would lower blood pressure more effectively than WM alone.
But there is a third way of explaining the findings of this review: some herbal remedies might actually have a hypotensive effect. The trouble is that this review does come not even close to telling us which.
