quackery
This study from the department of Osteopathic Manipulative Medicine, New York Institute of Technology College of Osteopathic Medicine tested whether new-onset impairments (NOI) of neurological functions identified by Immediate Post-Concussion Assessment and Cognitive Testing (ImPACT) will improve more so after osteopathic manipulative medicine (OMM) than after concussion-education.
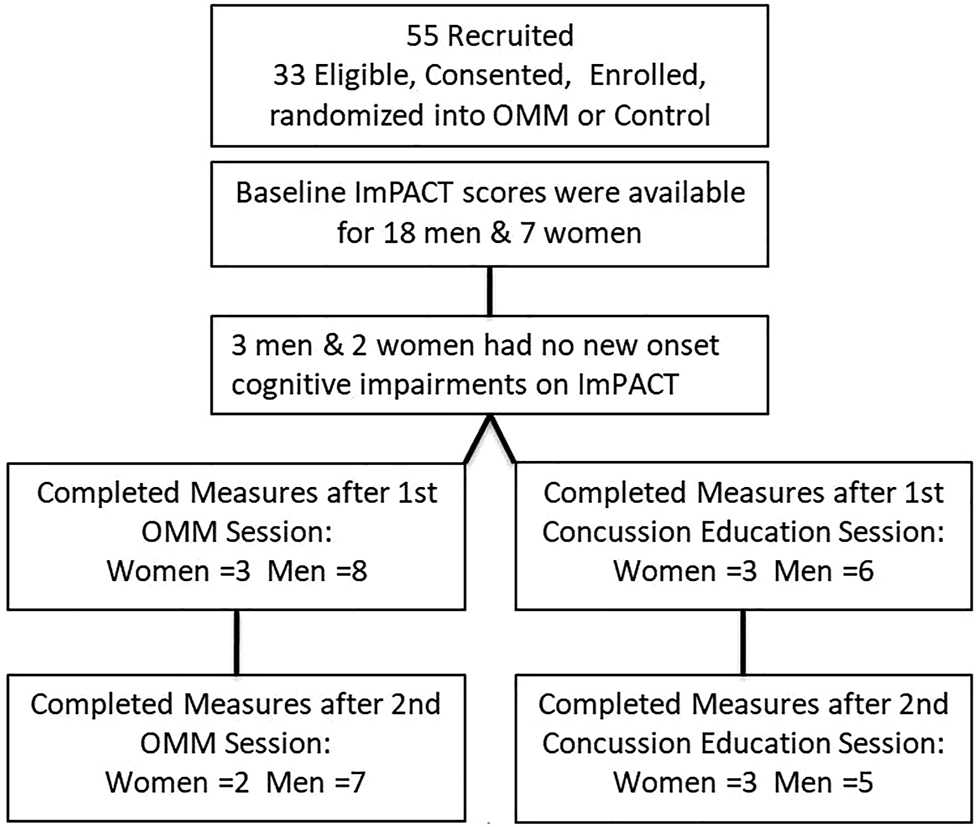
College athletes presenting to the outpatient academic healthcare center (AHCC) with concussion due to head injury within the preceding 2 weeks were recruited for this IRB-approved, randomized, single-blinded trial. Consented men and women were randomized into two groups:
- the verum group received two OMM treatments;
- the control group received two concussion-education sessions.
Preseason, Baseline, ImPACT was compared to Post-Injury scores to determine NOI. Baseline, Post-Injury, and Post-Interventions ImPACTs were compared by analysis of variance (ANOVA, α≤0.05). Post-Injury correlations and mean changes in King-Devick (KD) scores were analyzed.
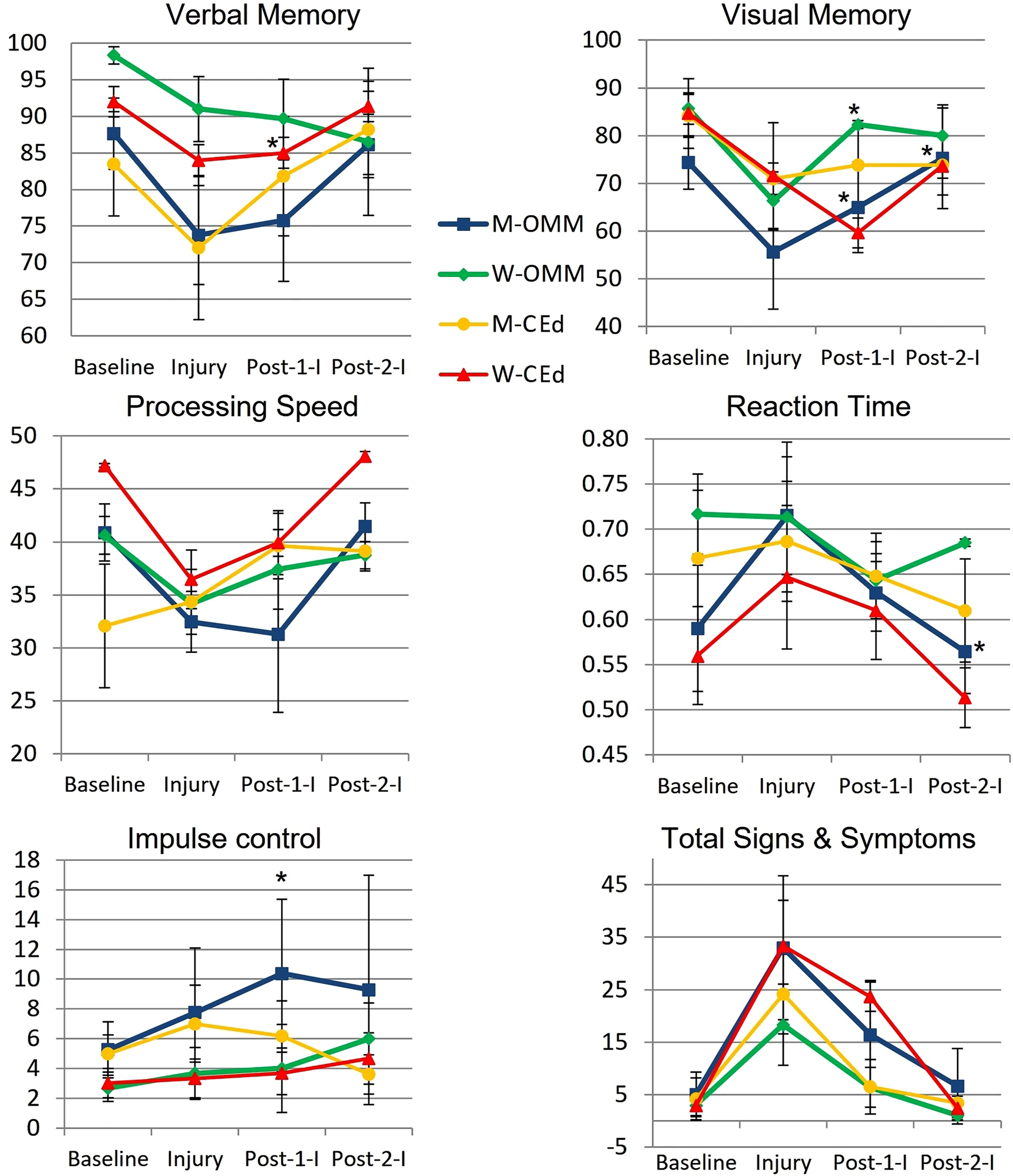
Post-Injury NOI were found in 77.8% (14/18) men and 85.7% (6/7) women, including ImPACT subscore indices for verbal and visual memory, processing speed (PS), and reaction time (RT). Of those with NOI, mean visual memory recovered by 50.0% following one and by 104.9% (p=0.032) following two OMM treatments in men and by 82.8% (p=0.046) following one treatment in women. Following two interventions, the mean RT in men receiving OMM improved by 0.10 more than education (p=0.0496). The effect sizes of OMM were large (Cohen’s d=1.33) on visual memory and small (Cohen’s d=0.31) on RT.
The authors concluded that NOI in visual memory and RT following concussion significantly improved in the OMM group compared to the education group. Integrating OMM utilizing physical exam and this treatment was a safe individualized approach in athletes with acute uncomplicated concussions. Further research is warranted to improve the utilization of OMM for individuals with concussion.
What the abstract does not tell you is that the two groups were extremely small and that they became even smaller, as some patients were lost to follow-up.
In addition, the results were all over the place.
Furthermore, it is noteworthy that neither the therapists nor the patients were blinded and the observation period was short. Finally, the authors state in their conclusions that OMM is safe. Considering the sample size and the attrition rate (perhaps all those patients lost to follow-up died?), this is of course ridiculously wishful thinking.
So, what can we conclude from this study? I don’t know about you, but I conclude that the department of Osteopathic Manipulative Medicine, New York Institute of Technology College of Osteopathic Medicine could do with a good science teacher.
Wellness seems to be everywhere these days – I mean of course the term, not the state or condition. On Medline, we find in excess of 500 000 articles on wellness, just for the year 2022! Wellness is en vogue, sexy, politically correct, etc. It looks good to talk and write about it. Most importantly it is good business. A report by the Global Wellness Institute stated that in 2020 the wellness industry was valued at $4.5 trillion and continues to grow at a frightening rate.
Having studied some of the recent literature on the subject, I get the impression that, for many, wellness is foremost an excuse for waffling utter nonsense. Let me, therefore, today ask just 5 simple questions about wellness that are likely to reduce the wellness of the ‘wellness brigade’:
1.What is wellness?
It is quite evidently a sector that is unable to define itself. Here are just a few of the definitions that have been suggested. Wellness is:
- the active pursuit of activities, choices and lifestyles that lead to a state of holistic health
- the result of personal initiative, seeking a more optimal, holistic and balanced state of health and well-being across multiple dimensions
- an active process of becoming aware of and making choices towards a healthy and fulfilling life
- the state of being in good health, especially as an actively pursued goal
- a state beyond absence of illness but rather aims to optimize well-being
- the act of practicing healthy habits on a daily basis to attain better physical and mental health outcomes
- an active process through which people become aware of, and make choices toward, a more successful existence
- the optimal state of health of individuals and groups
A 2018 review revealed that there is a lack of a uniform definition of wellness and showed that there is insufficient evidence to support the clinical utility of a single particular wellness instrument.
2. How do we measure wellness?
The short answer to this question is: nobody is quite sure. There simply is no generally accepted, well-validated measure. A few domains come to mind:
- physical functioning,
- somatic symptoms, e.g. pain,
- psychological symptoms,
- social functioning,
- needs and satisfaction.
But there is no simple means to quantify wellness. If you think that I am exaggerating, consider this recent review: 79 mental wellness instruments were identified. Most studies did not provide a definition for mental wellness. We identified thirteen mental wellness concepts from 97 studies, namely: life satisfaction, mental wellbeing [general], resilience, self-efficacy, self- esteem, connectedness, coping, self-control, mindfulness/spiritual, hope, sense of coherence, happiness, and life purpose.
3. What affects wellness?
The short answer is: potentially everything. My very own wellness, for instance, deteriorates sharply, if I have to read yet another nonsensical article about it.
4. Which interventions improve wellness?
As we have seen in my previous post, this is where so-called alternative medicine (SCAM) comes in. Since there is no measure to quantify wellness, we just have to take the word of SCAM proponents for it: SCAM improves wellness!!!
Which specific SCAM?
Can I see the evidence?
Sorry, no questions allowed!
And if you dare to insist on evidence, the ‘wellness brigade’ would just give you a pitiful smile and say: wellness has to be experienced, not measured.
5. Are there risks?
Yes, of course! Here are just some of them:
- The treatments advocated for wellness almost invariably cost money.
- The treatments advocated for wellness almost invariably cause direct and indirect harm, as discussed in many of my previous posts.
- Wellness treatments tend to give the impression that one can buy wellness like an expensive piece of clothing without putting in any real effort oneself.
Considering all this, I’d like to offer my very own definition of the sector:
Wellness is a fashionable paradise for charlatans in which they are protected from scientific scrutiny and feel at liberty to bullshit to their hearts’ content.
The All-Party Parliamentary Group (APPG) on Beauty and Wellbeing, UK, has undertaken an investigation into the ‘complementary therapies sector’, to consider how the sector can support everyone’s physical health, mental health, and well-being and take pressure off the NHS. In their recent document, they state:
The complementary therapies industry is an integral part of the Personal Care sector, which includes beauty, wellbeing, and alternative therapies. These therapies can be key to supporting everyone’s health and mental wellbeing…
To ensure complementary therapies can adequately support the NHS, we need to attract more talent into the sector and ensure all therapists receive the right training to become highly skilled professionals.
We also need to enhance the perception of the professionalism within the sector, so that it is no longer seen as ‘frivolous and fluffy’ and non-essential. Building awareness and understanding of its value in supporting our nation’s health is one step. However, it also important to crack down on any bad practice and the ‘underground market’ of poor treatment…
The committee makes the following recommendations:
1. The Government must work with NHS England to better promote the benefits of social prescribing with GPs, nurses and other health and care professionals, and how they can refer people to non-clinical complementary therapy services.
2. The Personal Care sector team in the Department for Business, Energy, Industry and Strategy must work with officials within the Department for Health and Social Care responsible for social prescribing to better integrate complementary therapy services into the NHS, and produce guidance to support health professionals and therapists in doing so.
3. The Department for Health and Social Care must undertake or fund research studies to demonstrate the value of integrating complementary therapy services into the NHS through social prescribing.
4. The Department for Education must revisit the gap between the apprentice wage and minimum wage for apprentices aged 19+, and provide financial incentives for employers to take on learners on any ‘job ready ‘qualification.
5. The Government must give Environmental health officers (EHOs) greater powers to act quickly to deal with bad practice and lead a crack-down on tax evading businesses that are driving down prices and undermining legitimate businesses under pressure.
…
…
…
Conclusions
The evidence that we have received during this investigation clearly demonstrate that greater support
and recognition is needed for the complementary therapies sector to ensure that they are able support
everyone’s physical health, mental health and wellbeing and take pressure off the NHS.
We hope the Government will review our recommendations in order to support the complementary
therapies sector and ensure they have adequate funding and acknowledgement.
In case you are wondering what therapies they refer to, here is their complete list of the treatments (including links to what they seem to think about them):
This could have made me laugh, had it not been so serious. The committee is composed of MPs who might be full of goodwill. Yet, they seem utterly clueless regarding the ‘complementary therapies sector’. For instance, they seem to be unaware of the evidence for some of the treatments they want to promote, e.g. craniosacral therapy, aromatherapy, Reiki, shiatsu, energy healing, or reflexology (which is far less positive than they seem to assume); and they aim at enhancing the “perception of the professionalism” instead of improving the PROFESSIONALISM of the therapists (which obviously would include adherence to evidence-based practice). And perhaps the committee might have given some thought to the question of whether it is ethical to push dubious therapies onto the unsuspecting public.
I could go on, but the perplexing wooliness of the document speaks for itself, I think.
And in case you are wondering who the MP members of the committee are, here is the list of its members:
• Carolyn Harris MP – Co-Chair
• Judith Cummins MP – Co-Chair
• Jessica Morden MP – Vice-Chair
• Jackie Doyle-Price MP – Vice-Chair
• Peter Dowd MP – Treasurer
• Nick Smith MP – Secretary
• Caroline Nokes MP – Member
• Sarah Champion MP – Member
• Alex Davies-Jones MP – Member
• Kate Osamor MP – Member
• John McNally MP – Member
• Kevan Jones MP – Member
• Gagan Mohindra MP- Member
The Secretariat for this APPG is Dentons Global Advisors with support from the National Hair and Beauty Federation, the Federation of Holistic Therapists and spabreaks.com.
PS
Two hours after having posted this, I begin to feel bad about being so dismissive. Let me thus try to do something constructive: I herewith offer to give one or more lectures to the committee about the evidence as it pertains to the therapies they included in their report.
In one of my last posts, I was rather dismissive of veterinary chiropractic.
Was I too harsh?
I did ask readers who disagree with my judgment to send me their evidence.
Sadly, none arrived!
Therefore, I did several further literature searches and found a recent review of the topic. It included 14 studies; 13 were equine and one was a canine study. Seven of these were cohort studies and seven were randomized controlled clinical trials. . Study quality was low (n = 4), moderate (n = 7), and high (n = 3) and included a wide array of outcome parameters with varying levels of efficacy and duration of therapeutic effects, which prevented further meta-analysis. The authors concluded that it was difficult to draw firm conclusions despite all studies reporting positive effects. Optimal technique indications and dosages need to be determined to improve the standardization of these treatment options.
This, I think, can hardly be called good evidence. But I also found this more recent paper:
Chiropractic care is a common treatment modality used in equine practice to manage back pain and stiffness but has limited evidence for treating lameness. The objective of this blinded, controlled clinical trial was to evaluate the effect of chiropractic treatment on chronic lameness and concurrent axial skeleton pain and dysfunction. Two groups of horses with multiple limb lameness (polo) or isolated hind limb lameness (Quarter Horses) were enrolled. Outcome measures included subjective and objective measures of lameness, spinal pain and stiffness, epaxial muscle hypertonicity, and mechanical nociceptive thresholds collected on days 0, 14, and 28. Chiropractic treatment was applied on days 0, 7, 14, and 21. No treatment was applied to control horses. Data was analyzed by a mixed model fit separately for each response variable (p < 0.05) and was examined within each group of horses individually. Significant treatment effects were noted in subjective measures of hind limb and whole-body lameness scores and vertebral stiffness. Limited or inconsistent therapeutic effects were noted in objective lameness scores and other measures of axial skeleton pain and dysfunction. The lack of pathoanatomical diagnoses, multilimb lameness, and lack of validated outcome measures likely had negative impacts on the results.
Great! So, we finally have an RCT of chiropractic for horses. Unfortunately, the study is less than convincing:
- It included just 20 polo horses plus 18 horses active in ridden or competitive work all suffering from lameness.
- The authors state that ‘horses were numerically randomized to treatment and control groups’; yet I am not sure what this means.
- Treatment consisted of high-velocity, low-amplitude, manually applied thrusts to sites of perceived pain or stiffness with the axial and appendicular articulations. Treatment was applied on days 0, 7, 14, and 21 by a single examiner. The control group received no treatment and was restrained quietly for 15 min to simulate the time required for chiropractic treatment. In other words, no placebo controls were used.
- The validity of the many outcome measures is unknown.
- The statistical analyses seem odd to me.
- No correction for multiple statistical tests was done.
- Most of the outcomes show no significant effect.
- Overall, there were some small positive treatment effects based on subjective assessment of lameness, but no measurable treatment effects on objective measures of limb lameness.
- The polo horses began their competition season at the beginning of the study which would have confounded the outcomes.
What does all this tell us about veterinary chiropractic?
Not a lot.
All we can safely say, I think, is that veterinary chiropractic is not evidence-based and that claims to the contrary are certainly ill-informed and most probably of a promotional nature.
About 10 years ago, I published this little post about ‘MY HOLISTIC HEALTH CENTRE’:
Where I live, some of the old-fashioned, privately-owned shops that used to dominate our high streets have survived the onslaught of the supermarkets. Our bakery is such a quaint remnant from the past. Surprisingly, it also is more holistic and more therapeutic than any alternative health centre I have come across.
The first thing that strikes anyone who enters the premises is the irresistible smell. Customers’ well-being hits the ceiling, and the local aromatherapists are in danger of going out of business. The intense stimulation of the customers’ olfactory system relaxes their minds and puts them into a meditative state as they patiently wait to be served. Everyone in the queue has a little word with the baker’s wife, and progress is therefore slow – but we don’t mind: the chat is holistic counseling at its best, and our slow movements toward the counter are healthier than tai chi.
“You are looking well today,” says the baker’s wife, thereby gently arousing me from my aroma-induced meditation and indicating that she is about to focus her shaman healing energy on me. Her diagnosis is spot on; the alternative therapies I enjoyed while waiting have re-balanced my chakras and got my qi flowing nicely – no wonder I am looking well!
The whole-wheat scones are finely balanced and nutritious; so I order three—one for the walk home and two for tea later. Prices have gone up a bit but, as with all holistic therapies, the more you pay, the more it’s worth. “Here you are,” she says, handing me her dietary delights. As I pay, our hands touch ever so briefly, just long enough for me to experience the instant transfer of healing energy that is so characteristic of Therapeutic Touch.
“Take care now, and God bless”, she says. As I walk out of her aura, I contemplate her words full of empathetic spiritual guidance and ancient wisdom. “That was expensive”, my wife mutters back home. I beg to differ: not only did I get the most wholesome food for my physical body, but I received holistic and patient-centered aromatherapy, counseling, meditation, tai chi, and energy healing for my emotional, psychological, and spiritual needs.
If only our Health Secretary knew about this traditional, yet integrated and therefore cutting-edge approach to cost-effective health and holistic well-being. We could all have it for free, and it might even save the NHS from its current crisis!
Since I wrote these lines, the healthcare crises have deepened and, in some countries, privatization is considered a possible solution. If that moment arrives, it will be the day of so-called alternative medicine (SCAM) clinics. They will pop up like mushrooms and prosper like gold mines. In preparation for this glorious development, I have been trying to think of a few names that would be best for attracting needy consumers to my new alternative health clinics:
- An establishment specializing in SCAM for grieving individuals: GOOD GRIEF
- A clinic for traditional acupuncture: WHAT’S THE POINT?
- A body purification center: CHUCKY’S DETOX TINCTURES
- An institute specializing in SCAM for erectile dysfunction: SOMETHING MIGHT COME UP
- A clinic for talking therapies: THE HOT AIR SALOON
- Osteopathy school: STILL FOR ALL ILLS
- An institute for veterinary homeopathy: NOTHING IS BETTER
- A center specializing in SCAM for premature ejaculation: COMING LATER
- SCAM diagnostic clinic: SECOND BEST OPINION
- Chiropractic clinic: SUBLUXOURIOUS LUXATIONS
- Energy healing institute: TOO GOOD TO BE TRUE
- Clinic specializing in SCAM for intestinal pain: GONE WITH A WIND
- Essential oils clinic: I CAN’T BELIEVE IT’S NOT BUTTER
- Coffee enema clinic: STARBUCKS
- Spiritual healing: CREED AND GREED
- Clinic for Oriental medicine: EAST OF EDEN
- Body reshaping center: WASTE WATCHERS
- Leech therapy clinic: BORN TO SUCK
- Mind-body institute: NEVER MIND
- Alternative computer skills: NEUROLINGUISTIC PROGRAMMING
- Vibrational medicine clinic: SATISFACTION GUARANTEED
- Homeopathic health clinic: A LOT TO DO ABOUT NOTHING
- Clinic specializing in SCAM for Benign Prostate Hypertrophy: TO PEE OR NOT TO PEE
I am sure many of you have much better ideas than I can think of – please, do not hesitate to let me know.
Drip IV is “Australia’s first and leading mobile healthcare company specialising in assisting with nutritional deficiencies”. They claim to provide a mobile IV service that is prescribed and tailored individually to your nutritional needs. Treatment plans and customised infusions are determined by a medical team to suit individual requirements. They deliver vitamins, minerals and amino acids directly to the body via the bloodstream, a method they state allows for optimal bioavailability.
These claims are a little puzzling to me, not least because vitamins, minerals and amino acids tailored individually to the nutritional needs of the vast majority of people would mean administering nothing at all. But I guess that virtually every person who consults the service will get an infusion [and pay dearly for it].
The Australian Therapeutic Goods Administration (TGA) seems to have a similarly dim view on Drip IV. The TGA has just issued 20 infringement notices totalling $159,840 to the company and to one of its executive officers. The reason: unlawful advertising of intravenous infusion products to Australian consumers on a company website and social media. Ten notices totalling $133,200 were issued to the company and ten notices totalling $26,640 were issued to an executive officer. The TGA considers the intravenous infusion products to be therapeutic goods because of the claims made about them, and the advertising to be unlawful because the advertisements allegedly:
- contained prohibited representations, such as claims regarding cancer.
- contained restricted representations such as that the products would alleviate fatigue caused by COVID-19, assist in the treatment of Graves’ Disease and Alzheimer’s Disease, and support the treatment of autoimmune diseases such as Multiple Sclerosis. No TGA approval had been given to make such claims.
- referred to ingredients that are prescription only, such as glutathione. Prescription medicines cannot be advertised directly to the public in Australia.
- contained a statement or picture suggesting or implying the products were ‘TGA Approved’. Advertising of therapeutic goods cannot include a government endorsement.
- contained a statement or picture expressing that the goods were ‘miraculous’.
Vitamin infusions have become very popular around the globe. There are now thousands of clinics offering this service, and many of them advertise aggressively with claims that are questionable. Here is just one example from the UK:
Modern life is hectic. If you are looking to boost your wellbeing, increase your energy levels, lift your mood and hydrate your body, Vitamin IV Infusions are ideal. Favoured by celebrities such as Madonna, Simon Cowell and Rihanna, Vitamin IV Infusions are an easy, effective way of delivering vitamins, minerals and amino acids directly into your bloodstream via an IV (intravenous) drip. Vitamins are essential for normal growth and staying healthy – but our bodies can’t produce all of the nutrients we need to function and thrive. That’s why more than one in three people take daily vitamin supplements – often without realising that only 15% of the active nutrients consumed orally actually find their way into their bloodstream. With Vitamin IV Infusions, the nutrients enter your bloodstream directly and immediately, and are delivered straight to your cells. We offer four different Vitamin IV Infusions, so you can choose the best combination for your personal needs, while boosting your general health, energy and wellbeing.
My advice to consumers is a little different and considerably less costly:
- to ensure you get enough vitamins, minerals, and amino acids, eat a balanced diet;
- to boost your well-being, sit down and calculate the savings you made by NOT using such a service;
- to increase your energy levels, take a nap;
- to lift your mood, recount the money you saved and think of what nice things you might buy with it;
- to hydrate your body drink a glass of water.
Perhaps it is time the authorities in all countries had a look at what these clinics are offering and what health claims they are making. Perhaps it is time they act as the TGA just did.
The UK medical doctor, Sarah Myhill, has a website where she tells us:
Everyone should follow the general approach to maintaining and restoring good health, which involves eating a paleo ketogenic diet, taking a basic package of nutritional supplements, ensuring a good night’s sleep on a regular basis and getting the right balance between work, exercise and rest. Because we live in an increasingly polluted world, we should probably all be doing some sort of detox regime.
She also happens to sell dietary supplements of all kinds which must surely be handy for all who want to follow her advice. Dr. Myhill boosted her income even further by putting false claims about Covid-19 treatments online. And that got her banned from practicing for nine months after a medical tribunal.
She posted videos and articles advocating taking vitamins and other substances in high doses, without evidence they worked. The General Medical Council (GMC) found her recommendations “undermined public health” and found some of her recommendations had the potential to cause “serious harm” and “potentially fatal toxicity”. The tribunal was told she uploaded a series of videos and articles between March and May 2020, describing substances as “safe nutritional interventions” which she said meant vaccinations were “rendered irrelevant”. But the substances she promoted were not universally safe and have potentially serious health risks associated with them, the panel was told. The tribunal found Dr. Myhill “does not practice evidence-based medicine and may encourage false reassurance in her patients who may believe that they will not catch Covid-19 or other infections if they follow her advice”.
Dr. Myhill previously had a year-long ban lifted after a General Medical Council investigation into her claims of being a “pioneer” in the treatment of chronic fatigue syndrome. In fact, the hearing was told there had been 30 previous GMC investigations into Dr. Myhill, but none had resulted in findings of misconduct.
Dr. Myhill is also a vocal critic of the PACE trial and biopsychosocial model of ME/CFS. Dr. Myhill’s GMC complaint regarding a number of PACE trial authors was first rejected without investigation by the GMC, after Dr. Myhill appealed the GMC stated they would reconsider. Dr. Myhill’s action against the GMC for failing to provide reasoning for not investigating the PACE trial authors is still continuing and began a number of months before the most recent GMC instigation of her practice started.
The recent tribunal concluded: “Given the circumstances of this case, it is necessary to protect members of the public and in the public interest to make an order suspending Dr. Myhill’s registration with immediate effect, to uphold and maintain professional standards and maintain public confidence in the profession.”
If you think that scanning through dozens of new scientific articles every week is a dry and often somewhat tedious exercise, you are probably correct. But every now and then, this task is turned into prime entertainment by some pseudoscientists trying to pretend to be scientists. Take, for instance, the latest homeopathy study by Indian researchers with no less than 9 seemingly impressive affiliations:
- 1Department of Organon of Medicine and Homoeopathic Philosophy, National Institute of Homoeopathy, Ministry of AYUSH, Govt. of India, Salt Lake, Kolkata, West Bengal, India.
- 2Department of Organon of Medicine and Homoeopathic Philosophy, National Institute of Homoeopathy, Ministry of AYUSH, Govt. of India, Block GE, Sector III, Salt Lake, Kolkata, West Bengal, India.
- 3Department of Homoeopathy, State Homoeopathic Dispensary, Karaila, Pratapgarh, Uttar Pradesh, India.
- 4Department of Homoeopathy, State Homoeopathic Dispensary, Tulsipur, Shrawasti, Uttar Pradesh, India.
- 5Department of Materia Medica, National Institute of Homoeopathy, Ministry of AYUSH, Govt. of India, Salt Lake, Kolkata, West Bengal, India.
- 6State Homoeopathic Dispensary, Mangalbari Rural Hospital, Matiali Block, Jalpaiguri, West Bengal, under Department of Health & Family Welfare, Govt. of West Bengal, India.
- 7Department of Repertory, The Calcutta Homoeopathic Medical College and Hospital, Govt. of West Bengal, Kolkata, West Bengal, India.
- 8Department of Homoeopathy, East Bishnupur State Homoeopathic Dispensary, Chandi Daulatabad Block Primary Health Centre, Village and Post Office: Gouripur (South), Police Station Bishnupur, West Bengal, under Department of Health & Family Welfare, Govt. of West Bengal, India.
- 9Department of Repertory, D. N. De Homoeopathic Medical College and Hospital, Govt. of West Bengal, Tangra, Kolkata, West Bengal, India.
Now that I have whetted your appetite, here is their study:
Lumbar spondylosis (LS) is a degenerative disorder of the lumbar spine. Despite substantial research efforts, no gold-standard treatment for LS has been identified. The efficacy of individualized homeopathic medicines (IHMs) in lumbar spondylosis (LS) is unknown. In this double-blind, randomized, placebo-controlled trial, the efficacy of IHMs was compared with identical-looking placebos in the treatment of low back pain associated with LS. It was conducted at the National Institute of Homoeopathy, West Bengal, India.
Patients were randomized to receive IHMs or placebos; standardized concomitant care was administered in both groups. The Oswestry low back pain and disability questionnaire (ODQ) was used as the primary outcome measure; the Roland-Morris questionnaire (RMQ) and the short form of the McGill pain questionnaire (SF-MPQ) served as secondary outcome measures. They were measured at baseline and every month for 3 months. Intention-to-treat analyses (ITT) were used to detect any inter-group differences using two-way repeated measures analysis of variance models overall and by unpaired t-tests at different time points.
Enrolment was stopped prematurely because of time restrictions; 55 patients had been randomized (verum: 28; control: 27); 49 could be analyzed by ITT (verum: 26; control: 23).
The results are as follows:
- Inter-group differences in ODQ (F 1, 47 = 0.001, p = 0.977), RMQ (F 1, 47 = 0.190, p = 0.665) and SF-MPQ total score (F 1, 47 = 3.183, p = 0.081) at 3 months were not statistically significant.
- SF-MPQ total score after 2 months (p = 0.030) revealed an inter-group statistical significance, favoring IHMs against placebos.
- Some of the SF-MPQ sub-scales at different time points were also statistically significant: e.g., the SF-MPQ average pain score after 2 months (p = 0.002) and 3 months (p = 0.007).
- Rhus Toxicodendron, Sulphur, and Pulsatilla nigricans were the most frequently indicated medicines.
The authors concluded that owing to failure in detecting a statistically significant effect for the primary outcome and in recruiting a sufficient number of participants, our trial remained inconclusive.
Now that I (and hopefully you too) have recovered from laughing out loud, let me point out why this paper had me in stitches:
- The trial was aborted not because of a “time limit” but because of slow recruitment, I presume. The question is why were not more patients volunteering? Low back pain with LS is extremely common. Could it be that patients know only too well that homeopathy does not help with low back pain?
- If a trial gets aborted because of very low patient numbers, it is probably best not to publish it or at least not to evaluate its results at all.
- If the researchers insist on publishing it, their paper should focus on the reason why it did not succeed so that others can learn from their experience by avoiding their mistakes.
- However, once the researchers do run statistical tests, they should be honest and conclude clearly that, because the primary outcome measure showed no inter-group difference, the study failed to demonstrate that the treatment is effective.
- The trial did not “remain inconclusive”; it was squarely negative.
- The editor of the journal HOMEOPATHY should know better than to publish such nonsense.
A final thought: is it perhaps the ultimate proof of homeopathy’s ‘like cures like’ assumption to use sound science (i.e. an RCT), submit it to the homeopathic process of endless dilutions and succussions, and – BINGO – generate utter nonsense?
The UK mainstream media have so far failed to report on this new and highly worrying development: in a rare show of unity, the UK practitioners of so-called alternative medicine (SCAM) have formed the ‘SCAM Union’ (SCAMU) – pronounced ‘scam you’ – and decided to go on strike. Their demands are straightforward:
- increase pay in line with inflation;
- full recognition of their profession;
- right to regular 15 min tai chi breaks.
Already last week, they staged a two-day nationwide walkout.
- Homeopaths stopped seeing patients and some had to start taking remedies at the C 2000 potency to keep calm but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Chiropractors did not adjust a single subluxation and started cracking jokes instead but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Naturopaths failed to detox a single patient but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Crystal healers kept their crystals under wraps but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Osteopath mobilized not a single joint but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Acupuncturists failed to insert a single needle but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Vaginal steamers only steamed the odd dim sum for lunch but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Ear candlers did not light a single candle and instead aligned them in a visual picket line but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Aromatherapists refused to open any bottles with essential oil but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Herbalists simply said ‘Thyme will tell’ but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Bach flower therapists had to consume their own Rescue Remedies in large quantities but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
- Holistic practitioners claimed to be wholly distraught but NOBODY NOTICED AND THE EFFECT ON THE NATIONS HEALTH WAS NOT NOTICABLE.
Perhaps the most outrageous thing about these events is that the UK press studiously ignored the all-out strike (one broadsheet editor commented: “if it’s not about Megan, we are not interested). Merely King Charles seemed alarmed and was overheard privately mumbling to Camilla: “What next?”
PS
I have been told that some of my readers have difficulties knowing when I am pulling their legs. So, let me confirm: every word here is uninvented – or was that uninventive?
About 3 years ago, I reported that the Bavarian government had decided to fund research into the question of whether the use of homeopathy would reduce the use of antibiotics (an idea that also King Charles fancies). With the help of some friends, I found further details of the project. Here are some of them:
The study on individualized homeopathic treatment to reduce the need for antibiotics in patients with recurrent urinary tract infections is a randomized, placebo-controlled, multicenter, double-blind trial. Frequent urinary tract infections (more than two infections within six months or more than three infections within twelve months) occur in up to three percent of all women during their lifetime and represent a high risk for increased antibiotic use in this population.
The current guidelines therefore also provide for therapeutic approaches without antibiotic administration under close monitoring. The approach to be investigated in the study is the administration of a homeopathic medicine individually selected for the patient for prophylaxis. The number of urinary tract infections and the need for antibiotics will be recorded and evaluated at the end of the trial period, around mid to late 2023.
The aim of the study is to find out whether patients taking homeopathics need antibiotics for the treatment of urinary tract infections less often compared to the placebo group. This could lead to a reduction in the use of antibiotics for recurrent urinary tract infections.
Project participants: Technical University of Munich, Klinikum Rechts der Isar
Project funding: 709,480.75 Euros
Project duration: January 1, 2021 to December 31, 2023
____________________
This sketch is of course not enough for providing a full evaluation of the study concept (if someone has more details, I’d be interested to learn more). From the little information given above, I feel that:
- the design of the trial might be quite rigorous,
- a fairly large sample will be required to have enough power,
- the closing date of 31/12/2023 seems optimistic (but this obviously depends on the number of centers cooperating),
- I, therefore, predict that we will have to wait a long time for the results (the pandemic and other obstacles will have delayed recruitment),
- the costs of the trial are already substantial and might increase due to delays etc.
My main criticism of the study is that:
- I see no rationale for doing such a trial,
- there is no evidence to suggest that homeopathy might prevent recurrent urinary tract infections,
- there is compelling evidence that homeopathic remedies are placebos,
- the study thus compares one placebo with another placebo (in fact, it is a classic example of what my late friend Harriet Hall would have called TOOTH FAIRY SCIENCE),
- therefore, its results will show no difference between the 2 groups (provided the trial was conducted without bias),
- if that is true, enthusiastic homeopaths will claim that the homeopathic verum was inadequate (e.g. because the homeopaths prescribing the verum did not or could not do their job properly),
- when that happens, they will therefore not stop claiming that homeopathy can reduce the over-prescribing of antibiotics;
- that means we will be exactly where we were before the trial.
In other words, the study will turn out to be a waste of 709,480.75 Euros. To express it as I did in my previous post: the Bavarian government has gone barmy!