conflict of interest
Prof. Harald Walach and his work have been regular topics on this blog (e.g. here, here, and here). Walach has served as the editor of Forschende Komplementärmedizin / Research in Complementary Medicine for 20 years and is now retiring from this post. On this occasion, he just published an EDITORIAL looking both back and ahead on research into so-called alternative medicine (SCAM). Here are the last paragraphs of his piece:
What lies in store? We do not know. “Hidden is the future before me, I am wondering what my destiny will bring,” sings Lensky in Tschaikowsky’s opera Eugen Onegin, and this is a good description of our current situation, not only in medicine, but also politically. If I have one wish for the future of CAM, for the future of our journal, then it is to keep the fire ablaze and uphold the hope of change that has been at the source of its founding and is still empowering many in the field. The field of medicine, but also the world, needs examples of visions and visionaries. The landscape will change. While the beginning of the field and the journal was a decidedly German-speaking, central European enterprise, we have now seen the extension of the field.
China has entered the scene with enormous manpower, a venerable tradition, and a huge amount of experience, research, and funding. Other countries, Iran for instance, are discovering the sources of traditional medical approaches. It might well be the case that those who forget that the world does not end at the rim of the Mediterranean and of the Atlantic will be left behind. It has always been a decisive element of CAM research that it bridged countries, nations, polities, and worldviews. The ISCMR, Consortium, and European Congress for Integrative Medicine (ECIM) conferences probably had as attendees more researchers from outside Europe and the US than from their host countries. Africa is only slowly beginning to enter the scene. The future will be less Euro- and Western-centric than the beginning of CAM, I am quite sure. The Western model of healthcare and economic growth through single pharmacological inventions is not sustainable worldwide and in the long run, apart from the fact that it is conceptually ill-founded. Thus, our hope very likely lies in broadening our view: thinking about other systems of medicine, other approaches, whole-systems thinking. This is actually very similar to our beginning. Every end is a beginning, every beginning is an end, Oscar Wilde used to say.
Apart from the abundant use of platitudes, there are several statements that might deserve a comment:
- The beginning of the field and the journal was a decidedly German-speaking, central European enterprise. Yes, the journal started as a predominantly German publication, yet the field was never mostly German/ central European. SCAM always included many modalities that originated from China, the US, and other non-European countries. Neither was the research into these areas ever dominated by German-speaking investigators.
- China has entered the scene with enormous manpower, a venerable tradition, and a huge amount of experience, research, and funding. This is true – but is it a good development? On this blog, I have often written about the fact that research from China is notoriously unreliable or even fabricated. As the quantity of such work is about to totally overwhelm SCAM research, this is a most concerning development, in my view.
- It has always been a decisive element of CAM research that it bridged countries, nations, polities, and worldviews. I would say that this is not something that characterizes SCAM research. It is a hallmark of any research. And considering my last point, it might soon no longer apply to SCAM. As we are being flooded with unreliable Chinese SCAM research, Chinese dominance might soon stifle criticism of SCAM.
- The Western model of healthcare and economic growth? As far as I can see, the model of economic growth is fast being adopted by non-Western counties.
So, what is the future of SCAM and SCAM research? Like Walach, I don’t know. But contrary to Walach, I hope for something entirely different. I hope that the stupidly short-sighted notion of two types of research and two types of healthcare can eventually be abandoned. In the end, there can only be one type of science – the one that understands itself as critically testing hypotheses by trying to prove them wrong – and only one type of medicine – the one that does more good than harm.
A review conducted in 2015 reported community pharmacists are willing to adopt a professional role in counselling consumers about the appropriate and safe use of so-called alternative medicine (SCAM) but faced multiple barriers in doing so. This current review aimed to update and extend these findings, by identifying studies published since 2015 that reported on pharmacists across any setting.
Eligible studies published between January 01, 2016, and December 31, 2021, were identified across 6 databases (PubMed, Scopus, Web of Science, EMBASE, ScienceDirect and MEDLINE). A grounded theory approach was used to thematically synthesize the data extracted.
A total of 64studies representing pharmacists across 30 countries were included for review. The study designs varied and included:
- cross-sectional surveys (n = 36),
- qualitative studies (n = 14),
- pseudo-patient studies (n = 3).
Eight studies reported on practice and/or bioethical responsibilities and 19 studies documented factors that would enable pharmacists to fulfill these responsibilities, while 37 studies reported on both.
The authors concluded that these findings indicate research about pharmacists’ responsibilities associated with SCAM is evolving from gap analysis towards research that is proactive in advocating for change in multiple areas. These findings can be used to inform a consensus discussion among pharmacists and key stakeholders regarding a set of professional responsibilities that would serve in the development of: a clearly defined role and associated practice standards, and competency requirements that inform educational learning objectives for inclusion in undergraduate, post-graduate and continuing professional pharmacy education.
I am puzzled why so many researchers in this specific area seem to avoid clearer language plainly stating the essential, simple, and undeniable facts. I am equally puzzled why so few pharmacists speak out.
It is obvious that community pharmacists are firstly healthcare professionals and only secondly shopkeepers. As such, they have important professional and ethical duties. Foremost, they are obliged to inform their customers responsibly – and responsible means telling them about the evidence for or against the SCAM product they are about to purchase. This duty also entails that pharmacists must inform themselves about the best current evidence. In turn, this means they must stop tolerating the current plethora of under- or post-graduate SCAM courses that are not evidence-based.
As we have discussed ad nauseam on this blog, none of this is actually happening (except in very few laudable cases)!
By and large, pharmacists continue to go along with the double standards of a) evidence for conventional drugs and b) fairy tales for SCAM. In the interest of progress, patient safety, and public health, it is time that pharmacists wake up and remind themselves that they are not commercially orientated shopkeepers but ethical healthcare professionals.
In recent weeks, I have been thinking a lot about ‘INTEGRATIVE MEDICINE‘. Skeptics mostly see it as a way of smuggling quackery into conventional healthcare. This is undoubtedly true and important. But it occurred to me that there also is a somewhat different perspective that has so far been neglected. Let me try to explain by recounting a story. It is fictive, of course, but the fiction is based on the observation of many cases during previous decades.
The story is about a doctor – let’s call him George – who, to be frank, is not the most gifted of his colleagues. Already at medical school, he was not as dedicated as his teachers would have hoped. In fact, medicine had not been his first choice at all. Yet he ended up as a general practitioner and eventually became a partner in a practice with 5 GPs.
Over the years, it became clear that George lacked something to be a good doctor. He knew his stuff, alright, got most of the diagnoses correct, and made not too many mistakes. But something was not quite right. One could say that, relative to his colleagues, he lacked kindness, dedication, compassion, and empathy. He often found it unnecessary to respect his patients. Sometimes, he even joked about them and about what he perceived as their stupidity.
If we view medicine as being both a science and an art, one might conclude that George was just about alright with the science but notably deficient in the art of healthcare. Most of his patients were aware that something was amiss; many even avoided him and tried to consult one of his colleagues instead. On more than one occasion, patients had told George that they were disappointed with his attitude. Some had even told him to the face that he lacked kindness. Such conversations made George think. He had to admit to himself that his colleagues were better at building good relationships with their patients. Eventually, George decided that something ought to change.
As it happened, George’s wife had a friend who was a Reiki healer. One day, he asked the healer – let’s call her Liz – whether she would like to try working alongside the GPs in his practice. Liz was delighted and accepted. George did not believe for a minute that Reiki was more than hocus-pocus, but he knew that Liz was kind and had loads of the compassion that he was so obviously lacking.
Hence force George and Liz formed a team: George looked after his patients the best he could and whenever he felt that more empathy and compassion were required, he would send the patient to Liz. This partnership changed everything. The patients were content, George was happy, and Liz was beaming.
As some patients frowned at the idea of Reiki, George soon recruited an aromatherapist as well. After that, a lay homeopath and a reflexologist were employed. George’s GP partners (who made little use of the alternative practitioners) were sure that none of these therapies had any specific effects (incidentally, a belief not shared by the practitioners in question who felt they were doing wonders). But for George, the therapists clearly did supplement his limited interpersonal skills. Patients were delighted and the GP practice began to thrive. As for George, he became an increasingly outspoken and prominent advocate of INTEGRATED MEDICINE. The fact that there was no evidence to support it did hardly matter to him; what counted was that it rendered his own incompetence less visible.
About a year later, George convinced his slightly bewildered partners to rename their practice ‘THE INTEGRATIVE HEALTH CENTRE’.
End of story
In case you did not get my point, let me make it more bluntly: INTEGRATIVE MEDICINE can be a way for some doctors to delegate the art of medicine to quacks. Good doctors don’t need to do this because they are able to show compassion and treat their patients as whole human beings. Less gifted doctors, however, find INTEGRATIVE MEDICINE a practical solution to their own incompetence.
So, is INTEGRATIVE MEDICINE a good compromise then?
No, certainly not!
The last thing we need in healthcare is for doctors to start delegating the art of medicine to others. It would be a serious mistake, nothing less than abandoning the core values of medicine to charlatans.
But what is the solution?
Obviously, it is to make sure all doctors are competent. We need to select medical students adequately, tell them much more about the importance of kindness, compassion, empathy, holism, etc., and teach them how to show and use these qualities. We need to train doctors to be competent in both the science and the art of medicine. This has to begin in medical school and must continue throughout their professional career. We need to make sure that doctors like George understand the message; if they prove to be unable to do so, we should direct them to professions where compassion is not essential.
The worst solution we can possibly envisage is to allow charlatans to cover up the incompetence of people like George and call it INTEGRATED MEDICINE.
This study described osteopathic practise activity, scope of practice and the osteopathic patient profile in order to understand the role osteopathy plays within the United Kingdom’s (UK) health system a decade after the authors’ previous survey.
The researchers used a retrospective questionnaire survey design to ask about osteopathic practice and audit patient case notes. All UK-registered osteopaths were invited to participate in the survey. The survey was conducted using a web-based system. Each participating osteopath was asked about themselves, and their practice and asked to randomly select and extract data from up to 8 random new patient health records during 2018. All patient-related data were anonymized.
The survey response rate was 500 osteopaths (9.4% of the profession) who provided information about 395 patients and 2,215 consultations. Most osteopaths were:
- self-employed (81.1%; 344/424 responses),
- working alone either exclusively or often (63.9%; 237/371),
- able to offer 48.6% of patients an appointment within 3 days (184/379).
Patient ages ranged from 1 month to 96 years (mean 44.7 years, Std Dev. 21.5), of these 58.4% (227/389) were female. Infants <1 years old represented 4.8% (18/379) of patients. The majority of patients presented with musculoskeletal complaints (81.0%; 306/378) followed by pediatric conditions (5%). Persistent complaints (present for more than 12 weeks before the appointment) were the most common (67.9%; 256/377) and 41.7% (156/374) of patients had co-existing medical conditions.
The most common treatment approaches used at the first appointment were:
- soft-tissue techniques (73.9%; 292/395),
- articulatory techniques (69.4%; 274/395),
- high-velocity low-amplitude thrust (34.4%; 136/395),
- cranial techniques (23%).
The mean number of treatments per patient was 7 (mode 4). Osteopaths’ referral to other healthcare practitioners amounted to:
- GPs 29%
- Other complementary therapists 21%
- Other osteopaths 18%
The authors concluded that osteopaths predominantly provide care of musculoskeletal conditions, typically in private practice. To better understand the role of osteopathy in UK health service delivery, the profession needs to do more research with patients in order to understand their needs and their expected outcomes of care, and for this to inform osteopathic practice and education.
What can we conclude from a survey that has a 9% response rate?
Nothing!
If I ignore this fact, do I find anything of interest here?
Not a lot!
Perhaps just three points:
- Osteopaths use high-velocity low-amplitude thrusts, the type of manipulation that has most frequently been associated with serious complications, too frequently.
- They also employ cranial osteopathy, which is probably the least plausible technique in their repertoire, too often.
- They refer patients too frequently to other SCAM practitioners and too rarely to GPs.
To come back to the question asked in the title of this post: What do UK osteopaths do? My answer is
ALMOST NOTHING THAT MIGHT BE USEFUL.
This study aimed to evaluate the number of craniosacral therapy sessions that can be helpful to obtain a resolution of the symptoms of infantile colic and to observe if there are any differences in the evolution obtained by the groups that received a different number of Craniosacral Therapy sessions at 24 days of treatment, compared with the control group which did not received any treatment.
Fifty-eight infants with colic were randomized into two groups:
- 29 babies in the control group received no treatment;
- babies in the experimental group received 1-3 sessions of craniosacral therapy (CST) until symptoms were resolved.
Evaluations were performed until day 24 of the study. Crying hours served as the primary outcome measure. The secondary outcome measures were the hours of sleep and the severity, measured by an Infantile Colic Severity Questionnaire (ICSQ).
Statistically significant differences were observed in favor of the experimental group compared to the control group on day 24 in all outcome measures:
- crying hours (mean difference = 2.94, at 95 %CI = 2.30-3.58; p < 0.001);
- hours of sleep (mean difference = 2.80; at 95 %CI = – 3.85 to – 1.73; p < 0.001);
- colic severity (mean difference = 17.24; at 95 %CI = 14.42-20.05; p < 0.001).
Also, the differences between the groups ≤ 2 CST sessions (n = 19), 3 CST sessions (n = 10), and control (n = 25) were statistically significant on day 24 of the treatment for crying, sleep and colic severity outcomes (p < 0.001).
The authors concluded that babies with infantile colic may obtain a complete resolution of symptoms on day 24 by receiving 2 or 3 CST sessions compared to the control group, which did not receive any treatment.
Why do SCAM researchers so often have no problem leaving the control group of patients in clinical trials without any treatment at all, while shying away from administering a placebo? Is it because they enjoy being the laughingstock of the science community? Probably not.
I suspect the reason might be that often they know that their treatments are placebos and that their trials would otherwise generate negative findings. Whatever the reasons, this new study demonstrates three things many of us already knew:
- Colic in babies always resolves on its own but can be helped by a placebo response (e.g. via the non-blinded parents), by holding the infant, and by paying attention to the child.
- Flawed trials lend themselves to drawing the wrong conclusions.
- Craniosacral therapy is not biologically plausible and most likely not effective beyond placebo.
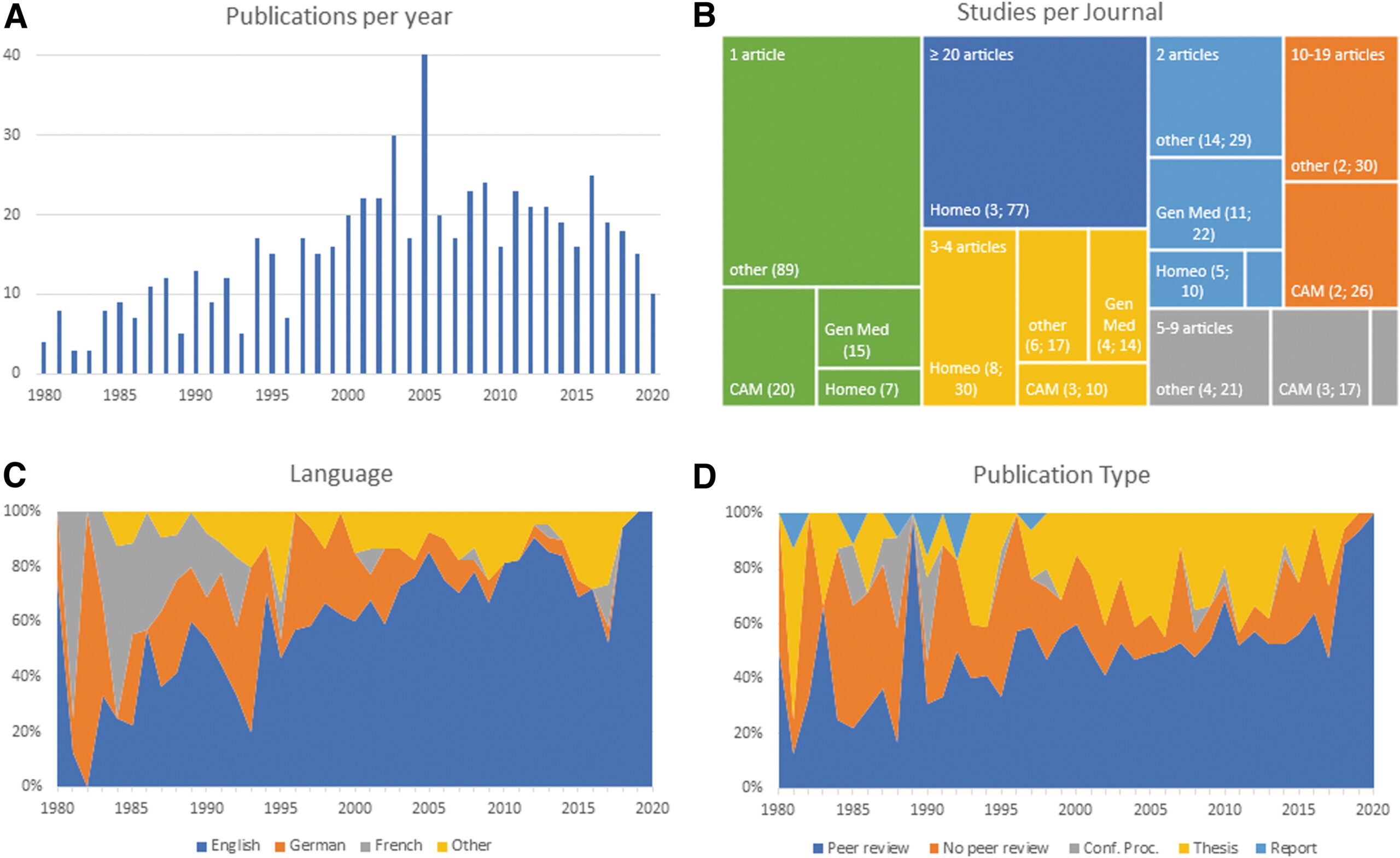
The authors of this article searched 37 online sources, as well as print libraries, for homeopathy (HOM) and related terms in eight languages (1980 to March 2021). They included studies that compared a homeopathic medicine or intervention with a control regarding the therapeutic or preventive outcome of a disease (classified according to International Classification of Diseases-10). Subsequently, the data were extracted independently by two reviewers and analyzed descriptively.
A total of 636 investigations met the inclusion criteria, of which 541 had a therapeutic and 95 a preventive purpose. Seventy-three percent were randomized controlled trials (n = 463), whereas the rest were non-randomized studies (n = 173). The most frequently employed comparator was placebo (n = 400).
The type of homeopathic intervention was classified as:
- multi-constituent or complex (n = 272),
- classical or individualized (n = 176),
- routine or clinical (n = 161),
- isopathic (n = 19),
- various (n = 8).
The potencies ranged from 1X (dilution of -10,000) to 10 M (100–10.000). The included studies explored the effect of HOM in 223 different medical indications. The authors also present the evidence in an online database.
The authors concluded that this bibliography maps the status quo of clinical research in HOM. The data will serve for future targeted reviews, which may focus on the most studied conditions and/or homeopathic medicines, clinical impact, and the risk of bias of the included studies.
There are still skeptics who claim that no evidence exists for homeopathy. This paper proves them wrong. The number of studies may seem sizable to homeopaths, but compared to most other so-called alternative medicines (SCAMs), it is low. And compared to any conventional field of healthcare, it is truly tiny.
There are also those who claim that no rigorous trials of homeopathy with a positive results have ever emerged. This assumption is also erroneous. There are several such studies, but this paper was not aimed at identifying them. Obviously, the more important question is this: what does the totality of the methodologically sound evidence show? It fails to convincingly demonstrate that homeopathy has effects beyond placebo.
The present review was unquestionably a lot of tedious work, but it does not address these latter questions. It was published by known believers in homeopathy and sponsored by the Tiedemann Foundation for Classical Homeopathy, the Homeopathy Foundation of the Association of Homeopathic Doctors (DZVhÄ), both in Germany, and the Foundation of Homeopathy Pierre Schmidt and the Förderverein komplementärmedizinische Forschung, both in Switzerland.
The dataset established by this article will now almost certainly be used for numerous further analyses. I hope that this work will not be left to enthusiasts of homeopathy who have often demonstrated to be blinded by their own biases and are thus no longer taken seriously outside the realm of homeopathy. It would be much more productive, I feel, if independent scientists could tackle this task.
Guest post by Norbert Aust and Viktor Weisshäupl
Readers of this blog may remember the recent study of Frass et al. about the adjunct homeopathic treatment of patients suffering from non-small cell lung cancer (here). It was published in 2020 by the ‘Oncologist’, a respectable journal, and came to stunning results about to the effectiveness of homeopathy.
In our analysis, however, we found strong indications for duplicity: important study parameters like exclusion criteria or observation time were modified post hoc, and data showed characteristics that occur when unwanted data sets get removed.
We, that is the German Informationsnetzwerk Homöopathie and the Austrian ‘Initiative für wissenschaftliche Medizin’, had informed the Medical University Vienna about our findings – and the research director then asked the Austrian Agency for Scientific Integrity (OeAWI) to review the paper. The analysis took some time and included not only the paper and publicly available information but also the original data. In the end, OeAWI corroborated our findings: The results are not based on sound research but on modified or falsified data.
Here is their conclusion in full:
The committee concludes that there are numerous breaches of scientific integrity in the Study, as reported in the Publication. Several of the results can only be explained by data manipulation or falsification. The Publication is not a fair representation of the Study. The committee cannot for all the findings attribute the wrongdoings and incorrect representation to a single individual. However following our experience it is highly unlikely that the principal investigator and lead author, but also the co-authors were unaware of the discrepancies between the protocols and the Publication, for which they bear responsibility. (original English wording)
Profil, the leading news magazine of Austria reported in its issue of October 24, 2022, pp 58-61 (in German). There the lead author, Prof. M. Frass, a member of Edzard’s alternative medicine hall of fame, was asked for his comments. Here is his concluding statement:
All the allegations are known to us and completely incomprehensible, we can refute all of them. Our work was performed observing all scientific standards. The allegation of breaching scientific integrity is completely unwarranted. To us, it is evident that not all documents were included in the analysis of our study. Therefore we requested insight into the records to learn about the basis for the final statement.
(Die Vorwürfe sind uns alle bekannt und absolut unverständlich, alle können wir entkräften. Unsere Arbeit wurde unter Einhaltung aller wissenschaftlichen Standards durchgeführt. Der Vorhalt von Verstößen gegen die wissenschaftliche Intergrität enbehrt jeder Grundlage. Für uns zeigt sich offenkundig, dass bei der Begutachtung unserer Studie nicht alle Unterlagen miteinbezogen wurden. Aus diesem Grunde haben wir um Akteneinsicht gebeten, um die Grundlagen für das Final Statment kennenzulernen.)
The OeAWI together with the Medical University Vienna asked the ‘Oncologist’ for a retraction of this paper – which has not occurred as yet.
Turmeric is a commonly used herbal product implicated in causing liver injury. The aim of this case series was to describe the clinical, histologic, and human leukocyte antigen (HLA) associations of turmeric-associated liver injury enrolled in the U.S. Drug Induced Liver Injury Network (DILIN).
was to describe the clinical, histologic, and human leukocyte antigen (HLA) associations of turmeric-associated liver injury enrolled in the U.S. Drug Induced Liver Injury Network (DILIN).
All adjudicated cases enrolled in DILIN between 2004-2022 in which turmeric was an implicated product were reviewed. Causality was assessed using a 5-point expert opinion score. Available products were analyzed for the presence of turmeric using ultra-high-performance liquid chromatography. Genetic analyses included HLA sequencing.
Ten cases of turmeric-associated liver injury were found, all enrolled since 2011 and six since 2017. Of the 10 cases, 8 were women, 9 were White and the median age was 56 years (range, 35-71). Liver injury was hepatocellular in 9 patients and mixed in one. Liver biopsies in 4 patients showed acute hepatitis or mixed cholestatic-hepatitic injury with eosinophils. Five patients were hospitalized, and one patient died of acute liver failure. Chemical analysis confirmed the presence of turmeric in all 7 products tested; 3 also contained piperine (black pepper). HLA typing demonstrated that 7 patients carried HLA-B*35:01, 2 of whom were homozygous, yielding an allele frequency of 0.450 compared to population controls of 0.056-0.069.
The authors concluded that liver injury due to turmeric appears to be increasing in the United States, perhaps reflecting usage patterns or increased combination with black pepper. Turmeric causes potentially severe liver injury that is typically hepatocellular, with a latency of 1 to 4 months and strong linkage to HLA-B*35:01.
Turmeric or curcumin is said to cause multiple effects, such as inhibiting inflammation, oxidative stress, tumor cell proliferation, cell death, and infection. Yet, sound clinical trials to test whether these effects might translate into health benefits are rare. In addition, the bioavailability of oral turmeric supplements is known to be low.
Turmeric has been used in food for millennia and is thus generally considered to be safe. Known adverse effects include gastrointestinal problems such as nausea and diarrhea and allergic reactions. Clearly, the new case series casts considerable doubt on the safety of turmeric. Yet, one ought to point out that the number of cases is low (but, on the other hand under-reporting can be assumed to be high). Furthermore, we should take into account that the quality of commercially available products is often low. One must therefore ask whether the liver injuries were truly caused by turmeric itself or by contaminants.
My conclusion is that turmeric is unquestionably an interesting plant with considerable potential as a medicine. At present, there is much hype surrounding it. Yet, hype is almost always contra-productive. If we want to know the true value of turmeric, we need to solve the bioavailability problem and do much more research into its safety and efficacy for defined conditions.
Aging often contributes to a decrease in physical activity. As age advances, a decrease in muscle mass, muscle strength, and flexibility can impair physical function. One obvious way to prevent these developments might be regular physical exercise.
This open-label, randomized trial was intended to evaluate the effects of an integrated yoga module in improving the flexibility, muscle strength, and quality of life (QOL) of older adults. Participants were 96 older adults, aged 60-75 years (64.1 ± 3.95 years). The program was a three-month, yoga-based lifestyle intervention. The participants were randomly allocated to the intervention group (n = 48) or to a waitlisted control group (n = 48). The intervention group underwent three one-hour sessions of yoga weekly, with each session including loosening exercises, asanas, pranayama, and meditation spanning.
At baseline and post-intervention, the following assessments were made:
- spinal flexibility using a sit-and-reach test,
- back and leg strength using a back leg dynamometer,
- handgrip strength (HGS) and endurance (HGE) using a hand-grip dynamometer,
- Older People’s Quality of Life (OPQOL) questionnaire.
Analysis was performed employing Wilcoxon’s Sign Rank tests and Mann-Whitney Tests, using an intention-to-treat approach.
The results show that, compared to the control group, the intervention group experienced a significantly greater increase in spinal flexibility (P < .001), back leg strength (P < .001), HGE (P < .01), and QOL (P < .001) after three months of yoga.
The authors concluded that yoga can be used safely for older adults to improve flexibility, strength, and functional QOL. Larger randomized controlled trials with an active control intervention are warranted.
I agree with the authors that this trial was too small and not properly controlled. I disagree that their study shows yoga to be effective or safe. In fact, the two sentences of the conclusion do not seem to fit together at all.
Is it surprising that doing yoga exercises is better than doing nothing at all?
No!
Is it relevant to demonstrate this fact in an RCT?
No!
If anyone wants to test the value of yoga exercises, they must compare them to conventional exercises. And why don’t they do this? Could it be because they know they would be unlikely to show that yoga is superior?
Here in the UK, we are looking yet again for a new Prime Minister (PM). Did I say ‘we’? That’s not quite true; the Tory party is hunting for one, and it seems a difficult task for the talent-depleted conservatives. Eventually, the geriatric group of Tory members might again have the say. Amazingly, some senior Tories are already suggesting Boris Johnson (BJ).
To me, this demonstrates how common cognitive decline and memory loss seem to be among the elderly. They evidently have already forgotten that, only a few months ago, BJ has already been our PM.
Yes, it is often the short-term memory that suffers first!
It might, therefore, help to remind the Tory membership thus affected that BJ:
- was elected as PM in 2019,
- he then created scandal after scandal,
- he was even found guilty of breaking the law,
- he is still under investigation for misleading the Parliament,
- eventually, in 2022, he was removed from office after mishandling a sexual abuse scandal.
I hope this helps to refresh your memory, Tory members suffering from cognitive decline. Considering this blog is about so-called alternative medicine (SCAM), I should perhaps also offer you some treatments for the often progressive deterioration of mental capacity. Here is a recent paper that might point you in the right direction:
Senile ages of human life is mostly associated with developmental of several neurological complicated conditions including decreased cognition and reasoning, increased memory loss and impaired language performance. Alzheimer’s disease (AD) is the most prevalent neural disorder associated with dementia, consisting of about 70% of dementia reported cases. Failure of currently approved chemical anti-AD therapeutic agents has once again brought up the idea of administering naturally occurring compounds as effective alternative and/or complementary regimens in AD treatment. Polyphenol structured neuroprotecting agents are group of biologically active compounds abundantly found in plants with significant protecting effects against neural injuries and degeneration. As a subclass of this family, Flavonoids are potent anti-oxidant, anti-inflammatory and signalling pathways modulatory agents. Phosphatidylinositol 3-kinase (PI3K)/AKT and mitogen activated protein kinase (MAPK) pathways are both affected by Flavonoids. Regulation of pro-survival transcription factors and induction of specific genes expression in hippocampus are other important anti AD therapeutic activities of Flavonoids. These agents are also capable of inhibiting specific enzymes involved in phosphorylation of tau proteins including β-secretases, cyclin dependent kinase 5 and glycogen synthase. Other significant anti AD effects of Flavonoids include neural rehabilitation and lost cognitive performance recovery. In this review, first we briefly describe the pathophysiology and important pathways involved in pathology of AD and then describe the most important mechanisms through which Flavonoids demonstrate their significant neuroprotective effects in AD therapy.
Sorry, I forgot that this might be a bit too complex for semi-senile Tories. Put simply, this means consuming plenty of:
- berries,
- apples,
- garlic,
- onion,
- green tea,
- beans (beware flatulence in Parliament!)
In addition, I might advise you to stay off the Port, get enough rest, avoid stress of any type, and do plenty of aerobic exercise. And please:
- not too much excitement,
- stimulate your brain (this means avoid reading right-wing papers),
- no major scandals,
- no further deterioration of moral standards,
- no more lies,
- no more broken promises!
In other words, no vote for BJ!!!