chiropractic
Yesterday, L’EXPRESS published an interview with me. It was introduced with these words (my translation):
Professor emeritus at the University of Exeter in the United Kingdom, Edzard Ernst is certainly the best connoisseur of unconventional healing practices. For 25 years, he has been sifting through the scientific evaluation of these so-called “alternative” medicines. With a single goal: to provide an objective view, based on solid evidence, of the reality of the benefits and risks of these therapies. While this former homeopathic doctor initially thought he was bringing them a certain legitimacy, he has become one of their most enlightened critics. It is notable as a result of his work that the British health system, the NHS, gave up covering homeopathy. Since then, he has never ceased to alert us to the abuses and lies associated with these practices. For L’Express, he looks back at the challenges of regulating this vast sector and deciphers the main concepts put forward by “wellness” professionals – holism, detox, prevention, strengthening the immune system, etc.
The interview itself is quite extraordinary, in my view. While UK, US, and German journalists usually are at pains to tone down my often outspoken answers, the French journalists (there were two doing the interview with me) did nothing of the sort. This starts with the title of the piece: “Homeopathy is implausible but energy healing takes the biscuit”.
The overall result is one of the most outspoken interviews of my entire career. Let me offer you a few examples (again my translation):
Why are you so critical of celebrities like Gwyneth Paltrow who promote these wellness methods?
Sadly, we have gone from evidence-based medicine to celebrity-based medicine. A celebrity without any medical background becomes infatuated with a certain method. They popularize this form of treatment, very often making money from it. The best example of this is Prince Charles, sorry Charles III, who spent forty years of his life promoting very strange things under the guise of defending alternative medicine. He even tried to market a “detox” tincture, based on artichoke and dandelion, which was quickly withdrawn from the market.
How to regulate this sector of wellness and alternative medicines? Today, anyone can present himself as a naturopath or yoga teacher…
Each country has its own regulation, or rather its own lack of regulation. In Germany, for instance, we have the “Heilpraktikter”. Anyone can get this paramedical status, you just have to pass an exam showing that you are not a danger to the public. You can retake this exam as often as you want. Even the dumbest will eventually pass. But these practitioners have an incredible amount of freedom, they even may give infusions and injections. So there is a two-tier health care system, with university-trained doctors and these practitioners.
In France, you have non-medical practitioners who are fighting for recognition. Osteopaths are a good example. They are not officially recognized as a health profession. Many schools have popped up to train them, promising a good income to their students, but today there are too many osteopaths compared to the demand of the patients (knowing that nobody really needs an osteopath to begin with…). Naturopaths are in the same situation.
In Great Britain, osteopaths and chiropractors are regulated by statute. There is even a Royal College dedicated to chiropractic. It’s a bit like having a Royal College for hairdressers! It’s stupid, but we have that. We also have professionals like naturopaths, acupuncturists, or herbalists who have an intermediate status. So it’s a very complex area, depending on the state. It is high time to have more uniform regulations in Europe.
But what would adequate regulation look like?
From my point of view, if you really regulate a profession like homeopaths, it means that these professionals may only practice according to the best scientific evidence available. Which, in practice, means that a homeopath cannot practice homeopathy. This is why these practitioners have a schizophrenic attitude toward regulation. On the one hand, they would like to be recognized to gain credibility. But on the other hand, they know very well that a real regulation would mean that they would have to close shop…
What about the side effects of these practices?
If you ask an alternative practitioner about the risks involved, he or she will take exception. The problem is that there is no system in alternative medicine to monitor side effects and risks. However, there have been cases where chiropractors or acupuncturists have killed people. These cases end up in court, but not in the medical literature. The acupuncturists have no problem saying that a hundred deaths due to acupuncture – a figure that can be found in the scientific literature – is negligible compared to the millions of treatments performed every day in this discipline. But this is only the tip of the iceberg. There are many cases that are not published and therefore not included in the data, because there is no real surveillance system for these disciplines.
Do you see a connection between the wellness sector and conspiracy theories? In the US, we saw that Qanon was thriving in the yoga sector, for example…
Several studies have confirmed these links: people who adhere to conspiracy theories also tend to turn to alternative medicine. If you think about it, alternative medicine is itself a conspiracy theory. It is the idea that conventional medicine, in the name of pharmaceutical interests, in particular, wants to suppress certain treatments, which can therefore only exist in an alternative world. But in reality, the pharmaceutical industry is only too eager to take advantage of this craze for alternative products and well-being. Similarly, universities, hospitals, and other health organizations are all too willing to open their doors to these disciplines, despite the lack of evidence of their effectiveness.
Musculoskeletal disorders (MSDs) are highly prevalent, burdensome, and putatively associated with an altered human resting muscle tone (HRMT). Osteopathic manipulative treatment (OMT) is commonly and effectively applied to treat MSDs and reputedly influences the HRMT. Arguably, OMT may modulate alterations in HRMT underlying MSDs. However, there is sparse evidence even for the effect of OMT on HRMT in healthy subjects.
A 3 × 3 factorial randomized trial was performed to investigate the effect of myofascial release (MRT), muscle energy (MET), and soft tissue techniques (STT) on the HRMT of the corrugator supercilii (CS), superficial masseter (SM), and upper trapezius muscles (UT) in healthy subjects in Hamburg, Germany. Participants were randomised into three groups (1:1:1 allocation ratio) receiving treatment, according to different muscle-technique pairings, over the course of three sessions with one-week washout periods. We assessed the effect of osteopathic techniques on muscle tone (F), biomechanical (S, D), and viscoelastic properties (R, C) from baseline to follow-up (primary objective) and tested if specific muscle-technique pairs modulate the effect pre- to post-intervention (secondary objective) using the MyotonPRO (at rest). Ancillary, we investigate if these putative effects may differ between the sexes. Data were analysed using descriptive (mean, standard deviation, and quantiles) and inductive statistics (Bayesian ANOVA). 59 healthy participants were randomised into three groups and two subjects dropped out from one group (n = 20; n = 20; n = 19–2). The CS produced frequent measurement errors and was excluded from analysis. OMT significantly changed F (−0.163 [0.060]; p = 0.008), S (−3.060 [1.563]; p = 0.048), R (0.594 [0.141]; p < 0.001), and C (0.038 [0.017]; p = 0.028) but not D (0.011 [0.017]; p = 0.527). The effect was not significantly modulated by muscle-technique pairings (p > 0.05). Subgroup analysis revealed a significant sex-specific difference for F from baseline to follow-up. No adverse events were reported.
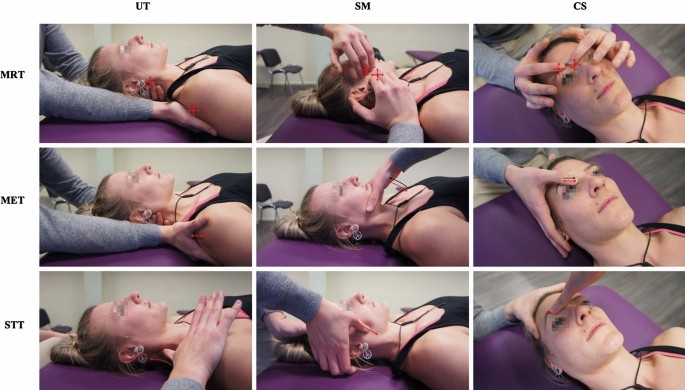
The authors concluded that OMT modified the HRMT in healthy subjects which may inform future research on MSDs. In detail, MRT, MET, and STT reduced the muscle tone (F), decreased biomechanical (S not D), and increased viscoelastic properties (R and C) of the SM and UT (CS was not measurable). However, the effect on HRMT was not modulated by muscle–technique interaction and showed sex-specific differences only for F.
I think that this study merits a few comments:
- It seems unsurprising that manual manipulation can relax muscles.
- The blinding of the volunteers was compromised because the participants were osteopathy students able to distinguish between the different interventions.
- The mechanisms underlying these reported changes in HRMT following OMT are unclear.
- The effects do not seem to be treatment-specific.
- The treatments used are not typical for osteopathy.
- Manual techniques are loosely defined or standardized.
- The duration of the effect is unknown but probably short.
- The size of the effect is small.
- The clinical relevance of the effect is doubtful.
I recently came across the ‘Sutherland Cranial College of Osteopathy’.
Sutherland Cranial College of Osteopathy?
Really?
I know what osteopathy is but what exactly is a ‘cranial college’?
Perhaps they mean ‘Sutherland College of Cranial Osteopathy’?
Anyway, they explain on their website that:
Cranial Osteopathy uses the same osteopathic principles that were described by Andrew Taylor Still, the founder of Osteopathy. Cranial osteopaths develop a very highly developed sense of palpation that enables them to feel subtle movements and imbalances in body tissues and to very gently support the body to release and re-balance itself. Treatment is so gentle that often patients are quite unaware that anything is happening. But the results of this subtle treatment can be dramatic, and it can benefit whole body health.
Sounds good?
I am sure you are now keen to become an expert in cranial osteopathy. The good news is that the college offers a course where this can be achieved in just 2 days! Here are the details:
This will be a spacious exploration of the nervous system. Neurological dysfunction and conditions feature greatly in our clinical work and this is especially the case in paediatric practice. The focus of this course is how to approach the nervous system in a fundamental way with reference to both current and historical ideas of neurological function. The following areas will be considered:
-
- Attaining stillness and grounding during palpation of the nervous system. It is within stillness that potency resides and when the treatment happens. The placement of attention.
- The pineal and its relationship to the tent, the pineal shift.
- The relations of the clivus and the central importance of the SBS, How do we assess and treat compression?
- The electromagnetic field and potency.
- The suspension of the cord within the spinal canal, the cervical and lumbar expansions.
- Listening posts for the central autonomic network.
Hawkwood College accommodation
Please be aware that accommodation at Hawkwood will be in shared rooms (single sex). Some single rooms are available on a first-come-first-served basis and will carry a supplement. Requesting a single room is not a guarantee that one will be provided.
£390.00 – £490.00
29 – 30 APRIL 2023 STROUD, UK
This will be a spacious exploration of the nervous system. Neurological dysfunction and conditions feature greatly in our clinical work and this is especially the case in pediatric practice.
_________________________
You see, not even expensive!
Go for it!!!
Oh, I see, you want to know what evidence there is that cranial osteopathy does more good than harm?
Right! Here is what I wrote in my recent book about it:
Craniosacral therapy (or craniosacral osteopathy) is a manual treatment developed by the US osteopath William Sutherland (1873–1953) and further refined by the US osteopath John Upledger (1932–2012) in the 1970s. The treatment consists of gentle touch and palpation of the synarthrodial joints of the skull and sacrum. Practitioners believe that these joints allow enough movement to regulate the pulsation of the cerebrospinal fluid which, in turn, improves what they call ‘primary respiration’. The notion of ‘primary respiration’ is based on the following 5 assumptions:
- inherent motility of the central nervous system
- fluctuation of the cerebrospinal fluid
- mobility of the intracranial and intraspinal dural membranes
- mobility of the cranial bones
- involuntary motion of the sacral bones.
A further assumption is that palpation of the cranium can detect a rhythmic movement of the cranial bones. Gentle pressure is used by the therapist to manipulate the cranial bones to achieve a therapeutic result. The degree of mobility and compliance of the cranial bones is minimal, and therefore, most of these assumptions lack plausibility.
The therapeutic claims made for craniosacral therapy are not supported by sound evidence. A systematic review of all 6 trials of craniosacral therapy concluded that “the notion that CST is associated with more than non‐specific effects is not based on evidence from rigorous RCTs.” Some studies seem to indicate otherwise, but they are of lamentable methodological quality and thus not reliable.
Being such a gentle treatment, craniosacral therapy is particularly popular for infants. But here too, the evidence fails to show effectiveness. A study concluded that “healthy preterm infants undergoing an intervention with craniosacral therapy showed no significant changes in general movements compared to preterm infants without intervention.”
The costs for craniosacral therapy are usually modest but, if the treatment is employed regularly, they can be substantial.
______________________________
As the college states “often patients are quite unaware that anything is happening”. Is it because nothing is happening? According to the evidence, the answer is YES.
So, on second thought, maybe you give the above course a miss?
Have you ever wondered how good or bad the education of chiropractors and osteopaths is? Well, I have – and this new paper promises to provide an answer.
The aim of this study was to explore Australian chiropractic and osteopathic new graduates’ readiness for transition to practice concerning their clinical skills, professional behaviors, and interprofessional abilities. Phase 1 explored final-year students’ self-perceptions, and this part uncovered their opinions after 6 months or more in practice.
Interviews were conducted with a self-selecting sample of phase 1 participant graduates from 2 Australian chiropractic and 2 osteopathic programs. Results of the thematic content analysis of responses were compared to the Australian Chiropractic Standards and Osteopathic Capabilities, the authority documents at the time of the study.
Interviews from graduates of 2 chiropractic courses (n = 6) and 2 osteopathic courses (n = 8) revealed that the majority had positive comments about their readiness for practice. Most were satisfied with their level of clinical skills, verbal communication skills, and manual therapy skills. Gaps in competence were identified in written communications such as case notes and referrals to enable interprofessional practice, understanding of professional behaviors, and business skills. These identified gaps suggest that these graduates are not fully cognizant of what it means to manage their business practices in a manner expected of a health professional.
The authors concluded that this small study into clinical training for chiropractic and osteopathy suggests that graduates lack some necessary skills and that it is possible that the ideals and goals for clinical education, to prepare for the transition to practice, may not be fully realized or deliver all the desired prerequisites for graduate practice.
Their conclusions in the actual paper finish with these sentences, in the main, graduate participants and the final year students were unable to articulate what professional behaviors were expected of them. The identified gaps suggest these graduates are not fully cognizant of what it means to manage their business practices in a manner expected of a health professional.
In several ways, this is a remarkable paper – remarkably poor, I hasten to add. Apart from the fact that its sample size was tiny and the response rate was low, it has many further limitations. Most notably, the clinical skills, professional behaviors, and interprofessional abilities were not assessed. All the researchers did was ask the participants how good or bad they were at these skills. Is this method going to generate reliable evidence? I very much doubt it!
Imagine, these guys have just paid tidy sums for their ‘education’ and they have no experience to speak of. Are they going to be in a good position to critically evaluate their abilities? No, I fear not!
Considering these flaws and the fact that chiropractors and osteopaths are not exactly known for their skills of critical thinking, I find it amazing that important deficits in their abilities nevertheless emerge. If I had to formulate a conclusion from all this, I might therefore suggest this:
A dismal study seems to suggest that chiropractic and osteopathic schooling is dismal.
PS
Come to think of it, there might be another fitting option:
Yet another team of chiro- and osteos demonstrate that they don’t know how to do science.
Pancoast tumors, also called superior sulcus tumors, are a rare type of cancer affecting the lung apex. These tumors can spread to the brachial plexus and spine and present with symptoms that appear to be of musculoskeletal origin. Patients with an advanced Pancoast tumor may thus feel intense, constant, or radiating pain in their arms, around their chest wall, between their shoulder blades, or traveling into their upper back or armpit. In addition, a Pancoast tumor may cause the following symptoms:
- Swelling in the upper arm
- Chest tightness
- Weakness or loss of coordination in the hand muscles
- Numbness or tingling sensations in the hand
- Loss of muscle tissue in the arm or hand
- Fatigue
- Unexplained weight loss
This case report details the story of a 59-year-old Asian man who presented to a chiropractor in Hong Kong with a 1-month history of neck and shoulder pain and numbness. His symptoms had been treated unsuccessfully with exercise, medications, and acupuncture. He had a history of tuberculosis currently treated with antibiotics and a 50-pack-year history of smoking.
Cervical magnetic resonance imaging (MRI) revealed a small cervical disc herniation thought to correspond with radicular symptoms. However, when the patient did not respond to a brief trial of chiropractic treatment, the chiropractor referred the patient back to the chest hospital for further testing, which confirmed the diagnosis of a Pancoast tumor. The patient was then referred for medical care and received radiotherapy and chemotherapy. At 2 months’ follow-up, the patient noted feeling lighter with less severe neck and shoulder pain and numbness. He also reported that he could sleep longer but still had severe pain upon waking for 2–3 hours, which subsided through the day.
A literature review identified six previously published cases in which a patient presented to a chiropractor with an undiagnosed Pancoast tumor. All patients had shoulder, spine, and/or upper extremity pain.
The authors concluded that patients with a previously undiagnosed Pancoast tumor can present to chiropractors given that these tumors may invade the brachial plexus and spine, causing shoulder, spine, and/or upper extremity pain. Chiropractors should be aware of the clinical features and risk factors of Pancoast tumors to readily identify them and refer such patients for medical care.
This is an important case report, in my view. It demonstrates that symptoms treated by chiropractors, osteopaths, and physiotherapists on a daily basis can easily be diagnosed wrongly. It also shows how vital it is that the therapist reacts responsibly to the fact that his/her treatments are unsuccessful. Far too often, the therapist has an undeniable conflict of interest and will say: “Give it more time, and, in my experience, symptoms will respond.”
The chiropractor in this story was brilliant and did the unusual thing of not continuing to treat his patient. However, I do wonder: might he be the exception rather than the rule?
One of my recent posts prompted the following comment from a chiropractor: “… please don’t let me stop you…while we actually treat patients“. It was given in the context of a debate about the evidence for or against chiropractic spinal manipulations as a treatment of whiplash injuries. My position was that there is no convincing evidence, while the chiropractor argued that he has been using manipulations for this indication with good results. Here I do not want to re-visit the pros and cons of that particular debate. Since similar objections have been put to me so many times, I want rather to raise several more principal points.
Before I do this, I need to quickly get the personal stuff out of the way: the comment implies that I don’t really know what I am talking about because I don’t see patients and thus don’t understand their needs. The truth is that I started my professional life as a clinician, then I went into basic science, then I went back into clinical medicine (while also doing research), and eventually, I became a full-time clinical researcher. I have thus seen plenty of patients, certainly enough to empathize with both the needs of patients and the reasoning of clinicians. In fact, these provided the motives for my clinical research during the last decades of my professional career (more details here).
Now about the real issue that is at stake here. When offered by a clinician to a scientist, the comment “… please don’t let me stop you…while we actually treat patients” is an expression of an arrogant feeling of superiority that clinicians often harbor vis a vis professionals who are not at the ‘coal face’ of healthcare. Stripped down to its core, the argument implies that science is fairly useless because the only knowledge worth having stems from dealing with patients. In other words, it is about the tension that so often exists between clinical experience and scientific evidence.
Many clinicians feel that experience is the best guide to correct decision-making.
Many scientists feel that experience is fraught with errors, and only science can lead us towards optimal decisions.
Such arguments emerge regularly on this blog and are constant company to almost any type of healthcare. The question is, who is right and who is wrong?
As I indicated, I can empathize with both positions. I can see that, in the context of making therapeutic decisions in a busy clinic, for instance, the clinician’s argument weighs heavily and can make sense, particularly in areas where the evidence is mixed, weak, or uncertain.
However, in the context of this blog and other discussions focused on critical evaluation of the science, I am strongly on the side of the scientist. In fact, in this context, the argument “… please don’t let me stop you…while we actually treat patients” seems ridiculous and resembles an embarrassing admission of having no rational argument left for defending one’s own position.
To put my view of this in a nutshell: it is not a question of either or; for optimal healthcare, we obviously need both clinical experience AND scientific evidence (an insight that is not in the slightest original, since it is even part of Sackett’s definition of EBM).
If you go on Twitter you will find that chiropractors are keen like mustard to promote the idea that, after a car accident, you should consult a chiropractor. Here is just one Tweet that might stand for hundreds, perhaps even thousands:
Recovering from a car accident? If you have accident-related injuries such as whiplash, chiropractic care may provide relief. Treatments like spinal manipulation and soft tissue therapy can aid in your recovery.
In case you don’t like Twitter, you could also go on the Internet where you find hundreds of websites that promote the same idea. Here are just two examples:
There is no question, chiropractors earn much of their living by treating patients suffering from whiplash (neck injury caused by sudden back and forth movement of the neck often causing neck pain and stiffness, shoulder pain, and headache) after a car accident with spinal manipulation.
Why?
There are two not mutually exclusive possibilities:
- They think it is effective.
- It brings in good money.
I have no doubt about the latter notion, yet I think we should question the first. Is there really good evidence that chiropractic manipulations are effective for whiplash?
When I was head of the PMR department at the University of Vienna, treating whiplash was my team’s daily bread. At the time, our strategy was to treat each patient according to the whiplash stage and to his/her individual signs and symptoms. Manipulations were generally considered to be contra-indicated. But that was about 30 years ago. Perhaps the evidence has now changed. Perhaps manipulation therapy has been shown to be effective for certain types of whiplash injuries?
To find out, I did a few Medline searches. These did, however, not locate compelling evidence for spinal manipulation as a treatment of any stage of whiplash injuries. Here is an example of the evidence I found:
In 2008, the Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders (Neck Pain Task Force) found limited evidence on the effectiveness of manual therapies, passive physical modalities, or acupuncture for the management of whiplash-associated disorders (WAD) or neck pain and associated disorders (NAD). This review aimed to update the findings of the Neck Pain Task Force, which examined the effectiveness of manual therapies, passive physical modalities, and acupuncture for the management of WAD or NAD. Its findings show the following: Evidence from 15 evaluation studies suggests that for recent neck pain and associated disorders grades I-II, cervical and thoracic manipulation provides no additional benefit to high-dose supervised exercises.
But this is most puzzling!
Why do chiropractors promote their manipulations for whiplash, if there is no compelling evidence that it does more good than harm? Again, there are two possibilities:
- They erroneously believe it to be effective.
- They don’t care but are in it purely for the money.
Whatever it is – and obviously not all chiropractors would have the same reason – I must point out that, in both cases, they behave unethically. Not being informed about the evidence related to the interventions used clearly violates healthcare ethics, and so does financially not informing and exploiting patients.
It has been reported that the US Insurer ‘State Farm’ is fighting a fraudulent scheme that has been exploiting New Jersey’s personal injury protection (PIP) benefits law since 2014. The insurer is seeking to recover $2.6 million in what it claims are fraudulent auto injury claims and a declaratory judgment that it need not pay any further claims submitted by the providers involved in the alleged scheme.
State Farm’s suit accuses 12 chiropractic and spine clinics and doctors of fraud, unjust enrichment, and violations of the New Jersey Insurance Fraud Prevention Act. The insurer alleges these providers used a “predetermined protocol” for all patients and a patient referral system for services that were either not performed or were not medically necessary for the individual patients. Instead, the services were carried out to enrich the defendants by exploiting the patients’ eligibility for PIP benefits, according to the complaint.
The suit accuses the providers of failing to legitimately evaluate patients to determine the true nature of their injuries and of reporting the same or similar findings for all patients to justify a predetermined course of treatment that was substantially the same for all patients. Part of the “predetermined protocol” for patients with soft-tissue injuries of the neck and back consisted of
- hot and cold packs,
- chiropractic manipulations,
- massage,
- mechanical traction,
- physical medicine and rehabilitation,
- and manual therapy.
These treatments were administered to almost every patient on almost every visit, regardless of each patient’s unique circumstances and needs, according to the complaint. The chiropractors are also accused of referring patients to diagnostic clinics, some allegedly illegally owned by the chiropractors, for an “unnecessary and predetermined course of pain management and invasive treatments” including injections. State Farm says they would submit false documentation for each case representing that the treatments were legitimately performed and medically necessary.
The 80-page complaint details case after case where the patient’s responses to questions and tests were the same or similar, allegedly serving as a “pretext to justify” the chiropractors’ wide range of treatments. The defendants in the complaint filed in U.S. District Court for New Jersey are:
- Tri-County Chiropractic and Rehabilitation Center,
- Robert Matturro, D.C.,
- Advanced Spine and Pain Management,
- Varinder Dhillon, M.D.,
- Nicholas Rosania, D.C.,
- Bloomfield UAI,
- Dov Rand, M.D.,
- Primary Medical Services,
- Louis J. Citarelli, M.D.,
- Chiro Health Center P.C.,
- Marc Matturro, D.C.
- Marco Tartaglia, M.D.
_____________________________
This story made me wonder: which of the listed treatments
- hot and cold packs,
- chiropractic manipulations,
- massage,
- mechanical traction,
- physical medicine and rehabilitation,
- and manual therapy
would ever be indicated for patients with soft-tissue injuries of the neck and back? Or more specifically, are chiropractic manipulations indicated or contra-indicated for such problems following a car accident? I fail to see any sound evidence that they are effective. If I am correct, should insurance companies not sue all chiropractors who routinely use manipulations for such cases? If the answer is YES, the sum of 2.6 million might need to be increased by several orders of magnitude.
As numerous of my posts have demonstrated, chiropractic manipulations can cause severe adverse effects, including deaths. Several hundred have been documented in the medical literature. When discussing this fact with chiropractors, we either see denial or we hear the argument that such events are but extreme rarities. To the latter, I usually respond that, in the absence of a monitoring system, nobody can tell how often serious adverse events happen. The resply often is this:
You are mistaken because the Royal College of Chiropractors’ UK-based Chiropractic Patient Incident Reporting and Learning System (CPiRLS) monitors such events adequately.
I have heard this so often that it is time, I feel, to have a look at CPiRLS. Here is what it says on the website:
CPiRLS is a secure website which allows chiropractors to view, submit and comment on patient safety incidents.
Access to CPiRLS
CPiRLS is currently open to all UK-based chiropractors, all ECU members and members of the Chiropractic and Osteopathic College of Australasia. To access the secure area of the CPiRLS website, please click the icon below and insert the relevant CPiRLS username and password when prompted.
In the UK, these can normally be found on your Royal College of Chiropractors’ membership card unless the details are changed mid-year. Alternatively, email [email protected] from your usual email address and we will forward the details.
Alternatively, in the UK and overseas, secure access details can be obtained from your professional association.
National associations and organisations wishing to use CPiRLS, or obtain trial access to the full site for evaluation purposes, should contact The Royal College of Chiropractors at [email protected]
Please click the icon below to visit the CPiRLS site.
Yes, you understood correctly. The public cannot access CPiRLS! When I click on the icon, I get this:
Welcome to CPiRLS
CPiRLS, The Chiropractic Patient Incident Reporting and Learning System – is an online reporting and learning forum that enables chiropractors to share and comment on patient safety incidents.
The essential details of submitted reports are published on this website for all chiropractors to view and add comments. A CPiRLS team identifies trends among submitted reports in order to provide feedback for the profession. Sharing information in this way helps to ensure the whole profession learns from the collective experience in the interests of patients.
All chiropractors are encouraged to adopt incident reporting as part of a blame-free culture of safety, and a routine risk management tool.
CPiRLS is secure and anonymous. There is no known way that anyone reporting can be identified, nor do those running the system seek to identify you. For this security to be effective, you require a password to participate.
Please note that reporting to CPiRLS is NOT a substitute for the reporting of patient safety incidents to your professional association and/or indemnity insurers.
So, how useful is CPiRLS?
Can we get any information from CPiRLS about the incidence of adverse effects?
No!
Do we know how many strokes or deaths have been reported?
No!
Can chiropractors get reliable information from CPiRLS about the incidence of adverse effects?
No, because reporting is not mandatory and the number of reports cannot relate to incidence.
Are chiropractors likely to report adverse effects?
No, because they have no incentive and might even feel that it would give their profession a bad name.
Is CPiRLS transparent?
No!
Is CPiRLS akin to postmarketing surveillance as it exists in conventional medicine?
No!
How useful is CPiRLS?
I think I let my readers answer this question.
Reports of serious complications of chiropractic manipulation keep on coming. Take this one, for instance:
My daughter went for a routine chiropractor appointment. Now she’s paralysed – 1:20 000 chiropractic neck manipulations result in stroke from vertebral artery dissection.
Or take a recent article by US neurosurgeons:
Cranio-cervical artery dissection (CeAD) is a common cause of cerebrovascular events in young subjects with no clear treatment strategy established. This study evaluated the incidence of major adverse cardiovascular events (MACE) in CeAD patients treated with and without stent placement. COMParative effectiveness of treatment options in cervical Artery diSSection (COMPASS) is a single high-volume center observational, retrospective longitudinal registry that enrolled consecutive CeAD patients over a 2-year period. Patients were ≥ 18 years of age with confirmed extra- or intracranial CeAD on imaging. Enrolled participants were followed for 1 year evaluating MACE as the primary endpoint.
One-hundred ten patients were enrolled (age 53 ± 15.9, 56% Caucasian, and 50% male, BMI 28.9 ± 9.2). Grade I, II, III, and IV blunt vascular injury was noted in 16%, 33%, 19%, and 32%, respectively. Predisposing factors were noted in the majority (78%), including
- sneezing,
- carrying a heavy load,
- chiropractic manipulation.
Stent was placed in 10 (10%) subjects (extracranial carotid n = 9; intracranial carotid n = 1; extracranial vertebral n = 1) at the physician’s discretion along with medical management. Reasons for stent placement were early development of high-grade stenosis or expanding pseudoaneurysm. Stented patients experienced no procedural or in-hospital complications and no MACE between discharge and 1 year follow up. CeAD patients treated with medical management only had 14% MACE at 1 year.
The authors concluded that in this single high-volume center cohort of CeAD patients, stenting was found to be beneficial, particularly with development of high-grade stenosis or expanding pseudoaneurysm. These results warrant confirmation by a randomized clinical trial.
Yes, I know: this study was not meant to investigate the link between chiropractic manipulations and CeAD. The finding that chiropractic manipulation is a predisposing factor for CeAD is entirely incidental. But it is an important finding nevertheless.
Chiropractors will laugh about the notion that manipulation is a risk factor akin to sneezing and thus try to trivialize the danger of their treatments. I would then point out that sneezing is unavoidable and fulfills a purpose. Chiropractic manipulations do neither.

