acupuncture
The objective of this study was to evaluate the effect of acupuncture on cognitive task performance in college students.
Sixty students aged 18-25 years were randomly allocated into acupuncture group (AG) (n=30) and control group (CG) (n=30). The AG underwent 20 min of acupuncture/day, while the CG underwent their normal routine for 10 days. Assessments were performed before and after the intervention.
Between-group analysis showed a significant increase in AG’s six-letter cancellation test (SLCT) score compared with CG. Within-group analysis showed a significant increase in the scores of all tests (i.e. SLCT, forward and backward Digit span test [DST]) in AG, while a significant increase in backward DST was observed in CG.
The authors concluded that acupuncture has a beneficial effect on improving the cognitive function of college students.
I am unable to access the full paper [it is behind a paywall]. Thus, I am unable to assess the study in further detail. As I am skeptical about the validity of the effect, I can only assume that it is due to the expectation of the volunteers receiving acupuncture. There was not even an attempt to control for placebo effects!
The over-stated conclusion made me wonder what else the 1st author has published. It turns out he has three more Medline-listed papers to his name all of which are about so-called alternative medicine (SCAM).
The 1st one is an RCT similar to the one above, i.e. without an attempt to control for placebo effects. Its conclusion is equally over-stated: Acupuncture could be considered as an effective treatment modality for the management of primary dysmenorrhea.
The other two papers refer to one case report each. Despite the fact that case reports (as any researcher must know) do not lend themselves to conclusions about the effectiveness of the treatments employed, the authors’ conclusions seem to again over-state the case:
- This suggests that integrative Naturopathy and Yoga therapies could be considered as an adjuvant to conventional medicine in rheumatoid arthritis associated with type-2 diabetes and essential hypertension.
- Though the results are encouraging, further studies are required with larger sample size and advanced inflammatory markers.
What does that tell us?
I don’t know about you, but I would not rely on acupuncture to improve my mental performance.
This randomized clinical trial (RCT) tested whether acupuncture is effective for the prevention of chronic tension-type headaches (CTTH). The researchers recruited 218 participants who were diagnosed with CTTH.
- The participants in the intervention group received 20 sessions of true acupuncture (TA group) over 8 weeks. The acupuncture treatments were standardized across participants, and each acupuncture site was needled to achieve deqi sensation. Each treatment session lasted 30 minutes.
- The participants in the control group received the same sessions and treatment frequency of superficial acupuncture (SA group)—defined as a type of sham control by avoiding deqi sensation at each acupuncture site.
The main outcome measure was the responder rate at 16 weeks after randomization. Followed-up was 32 weeks. A responder was defined as a participant who reported at least a 50% reduction in the monthly number of headache days (MHDs).
The responder rate was 68.2% in the TA group (n=110) versus 48.1% in the SA group (n=108) at week 16 (odds ratio, 2.65; 95%CI, 1.5 to 4.77; p<0.001); and 68.2% in the TA group versus 50% in the SA group at week 32 (odds ratio, 2.4; 95%CI, 1.36 to 4.3; p<0.001). The reduction in MHDs was 13.1±9.8 days in the TA group versus 8.8±9.6 days in the SA group at week 16 (mean difference, 4.3 days; 95%CI, 2.0 to 6.5; p<0.001), and the reduction was 14±10.5 days in the TA group versus 9.5±9.3 days in the SA group at week 32 (mean difference, 4.5 days; 95%CI, 2.1 to 6.8; p<0.001). Four mild adverse events were reported; three in the TA group versus one in the SA group.
The authors concluded that the 8-week TA treatment was effective for the prophylaxis of CTTH. Further studies might focus on the cost-effectiveness of the treatment.
“Our study showed that deqi sensation could enhance the effect of acupuncture in the treatment of chronic TTH, and the effect of acupuncture lasted at least 6 months when the treatment was stopped,” said co-investigator Ying Li, MD, PhD, The Third Hospital/Acupuncture and Tuina School, Chengdu University of Traditional Chinese Medicine, Chengdu, China.
Why am I not convinced?
Assuming that all the findings are correctly reported, the study does not at all show that the treatment was effective. It merely demonstrates that those patients who knew that were receiving TA told the researcher that they improved more than those who knew they has sham acupuncture. The difference in outcomes is not in the least surprising: patients’ knowledge of having had the verum leads to a placebo effect and to social desirability (patients giving the researchers positive responses simply because they were thankful for being looked after). Patients’ knowledge of having had the sham treatment leads to disappointment and thus worse outcomes.
But this is not the only reason why I am skeptical about this study. The authors claim they achieved deqi at every treatment. That is 20 treatments in 110 patients or 2 200 deqis! I think someone might be telling porkies here. Deqi cannot reliably be elicited on every single occasion. I, therefore, feel that perhaps the authors of this trial were a bit more than generous when writing up their study, and I am reminded of the recent report claiming that more than 80% of clinical trial data from China are fabricated.
Earlier this year, I started the ‘WORST PAPER OF 2022 COMPETITION’. As a competition without a prize is no fun, I am offering the winner (that is the lead author of the winning paper) one of my books that best fits his/her subject. I am sure this will overjoy him or her.
And how do we identify the winner? I will continue blogging about nominated papers (I hope to identify about 10 in total), and towards the end of the year, I let my readers decide democratically.
In this spirit of democratic voting, let me suggest to you ENTRY No 8 (it is so impressive that I must show you the unadulterated abstract):
Introduction
Female sexual dysfunction (FSD) seriously affects the quality of life of women. However, most women do not have access to effective treatment.
Aim
This study aimed to determine the feasibility and effectiveness of the use of acupuncture in FSD treatment based on existing clear acupuncture protocol and experience-supported face-to-face therapy.
Methods
A retrospective analysis was performed on 24 patients with FSD who received acupuncture from October 2018 to February 2022. The Chinese version of the female sexual function index , subjective sensation, sexual desire, sexual arousal, vaginal lubrication, orgasm, sexual satisfaction, and dyspareunia scores were compared before and after the treatment in all 24 patients.
Main Outcome Measure
A specific female sexual function index questionnaire was used to assess changes in female sexual function before and after the acupuncture treatment.
Results
In this study, the overall treatment improvement rate of FSD was 100%. The Chinese version of the female sexual function index total score, sexual desire score, sexual arousal score, vaginal lubrication score, orgasm score, sexual satisfaction score, and dyspareunia score during intercourse were significantly different before and after the treatment (P < .05). Consequently, participants reported high levels of satisfaction with acupuncture. This study indicates that acupuncture could be a new and effective technique for treating FSD. The main advantages of this study are its design and efficacy in treating FSD. To the best of our knowledge, this is the first study to evaluate the efficacy of acupuncture in the treatment of FSD using the female sexual function index scale from 6 dimensions. The second advantage is that the method used (ie, the nonpharmacological method) is simple, readily available, highly safe with few side effects, and relatively inexpensive with high patient satisfaction. However, limitations include small sample size and lack of further detailed grouping, pre and post control study of patients, blank control group, and pre and post control study of sex hormones.
Conclusion
Acupuncture can effectively treat FSD from all dimensions with high safety, good satisfaction, and definite curative effect, and thus, it is worthy of promotion and application.
My conclusion is very different: acupuncture can effectively kill any ability for critical thinking.
I hardly need to list the flaws of this paper – they are all too obvious, e.g.:
- there is no control group; the results might therefore be due to a host of factors that are unrelated to acupuncture,
- the trial was too small to allow far-reaching conclusions,
- the study does not tell us anything about the safety of acupuncture.
The authors call their investigation a ‘pilot study’. Does that excuse the flimsiness of their effort? No! A pilot study cannot draw conclusions such as the above.
What’s the harm? you might ask; nobody will ever read such rubbish and nobody will have the bizarre idea to use acupuncture for treating FSD. I’m afraid you would be wrong to argue in this way. The paper already got picked up by THE DAILY MAIL in an article entitled “Flailing libido? Acupuncture could help boost sex drive, scientists say” which was as devoid of critical thinking as the original study. Thus we can expect that hundreds of desperate women are already getting needled and ripped off as we speak. And in any case, offensively poor science is always harmful; it undermines public trust in research (and it renders acupuncture research the laughing stock of serious scientists).
England’s record goalscorer Ellen White has revealed she suffered a punctured lung while receiving acupuncture treatment. The injury accelerated her decision to retire. White, 33, said she was still coming to terms with the “traumatic” injury.
Manchester City had sourced a “specialist” – evidently not such an excellent acupuncturist because the complication is avoidable with proper knowledge of anatomy – outside the club to provide her with acupuncture to treat her back problem because of a high number of injuries in the squad at the time. “If you’d said to me two or three years ago that you’re going to retire, I would have said ‘absolutely not’, but I’ve got to a time in my career,” she said. “I had a challenging time last year – coming back from the Olympics, I basically punctured my lung, and it was a lot for me to have to go through and a big reason that accelerated my want to retire.”
The injury happened when she returned to her club with a back spasm last summer. “It punctured my lung which isn’t something that happens normally, obviously,” she said. “It was a really traumatic time for me and something that I’m still figuring out now, still working through. I had to wait for the lung to basically inflate again. I had a needle put into my chest to drag all the air out then hopefully the lung would inflate again – which it has. At the time, I think for me, I just got into a zone of: ‘I need to get back playing. We’ve got these games – I want to be back playing for my club; I want to be back playing for England. I went very tunnel vision,” she said. “It wasn’t until a good two or three months later, it just hit me like a train, what actually happened and how traumatic it was.”
Despite her quick return to goalscoring form, which included becoming the Lionesses record goalscorer in November, the striker says she is still affected by the injury and suffers “phantom pain” where it feels like it is happening again. “It’s important for me now to tell my story, and say it was a big factor in my year and leading up to the decision of wanting to retire. Obviously, there are other factors that come into that as well. I don’t want it to happen to anybody else again is my main thing. I don’t want to walk away from the sport having not told it and not say that I want things in place for it not to happen to anyone else.”
______________________________
Pneumothorax is by far the most common of all the serious, potentially fatal complications caused by acupuncture. In thin individuals, several acupuncture points over the upper thorax are just a few centimeters away from the lung. Therefore, it is easily possible to puncture a lung by inserting an acupuncture needle. This is from my 2010 review of the subject:
About 90 deaths after acupuncture have been anecdotally documented in the medical literature. Thus, acupuncture has been associated with more deaths than most other ‘alternative’ therapies except herbal medicine … The fatalities are usually due to an acupuncture needle penetrating a vital organ. This, in turn, can cause pneumothorax, cardiac tamponade, or major haemorrhage. Most instances of this nature are reported in the Asian literature which, for most of us, is not easily accessible.
A 2013 review of ours located 1104 cases that had been reported in the Korean literature alone. However, the truth of the matter is that nobody can be sure of the exact incidence figures. Why? Because there is no monitoring system that would reliably record such incidences.
I would argue that every single case of acupuncture-induced pneumothorax tells us that the acupuncturist was not adequately trained. With proper knowledge of anatomy, such complications should not happen. Therefore, such instances are a rude reminder that so-called alternative medicine (SCAM) is far too often in the hands of “specialists” who are a danger to the public.
Should Acupuncture-Related Therapies be Considered in Prediabetes Control?
No!
If you are pre-diabetic, consult a doctor and follow his/her advice. Do NOT do what acupuncturists or other self-appointed experts tell you. Do NOT become a victim of quackery.
But the authors of a new paper disagree with my view.
So, let’s have a look at the evidence.
Their systematic review was aimed at evaluating the effects and safety of acupuncture-related therapy (AT) interventions on glycemic control for prediabetes. The Chinese researchers searched 14 databases and 5 clinical registry platforms from inception to December 2020. Randomized controlled trials involving AT interventions for managing prediabetes were included.
Of the 855 identified trials, 34 articles were included for qualitative synthesis, 31 of which were included in the final meta-analysis. Compared with usual care, sham intervention, or conventional medicine, AT treatments yielded greater reductions in the primary outcomes, including fasting plasma glucose (FPG) (standard mean difference [SMD] = -0.83; 95% confidence interval [CI], -1.06, -0.61; P < .00001), 2-hour plasma glucose (2hPG) (SMD = -0.88; 95% CI, -1.20, -0.57; P < .00001), and glycated hemoglobin (HbA1c) levels (SMD = -0.91; 95% CI, -1.31, -0.51; P < .00001), as well as a greater decline in the secondary outcome, which is the incidence of prediabetes (RR = 1.43; 95% CI, 1.26, 1.63; P < .00001).
The authors concluded that AT is a potential strategy that can contribute to better glycemic control in the management of prediabetes. Because of the substantial clinical heterogeneity, the effect estimates should be interpreted with caution. More research is required for different ethnic groups and long-term effectiveness.
But this is clearly a positive result!
Why do I not believe it?
There are several reasons:
- There is no conceivable mechanism by which AT prevents diabetes.
- The findings heavily rely on Chinese RCTs which are known to be of poor quality and often even fabricated. To trust such research would be a dangerous mistake.
- Many of the primary studies were designed such that they failed to control for non-specific effects of AT. This means that a causal link between AT and the outcome is doubtful.
- The review was published in a 3rd class journal of no impact. Its peer-review system evidently failed.
So, let’s just forget about this rubbish paper?
If only it were so easy!
Journalists always have a keen interest in exotic treatments that contradict established wisdom. Predictably, they have been reporting about the new review thus confusing or misleading the public. One journalist, for instance, stated:
Acupuncture has been used for thousands of years to treat a variety of illnesses — and now it could also help fight one of the 21st century’s biggest health challenges.
New research from Edith Cowan University has found acupuncture therapy may be a useful tool in avoiding type 2 diabetes.
The team of scientists investigated dozens of studies covering the effects of acupuncture on more than 3600 people with prediabetes. This is a condition marked by higher-than-normal blood glucose levels without being high enough to be diagnosed as diabetes.
According to the findings, acupuncture therapy significantly improved key markers, such as fasting plasma glucose, two-hour plasma glucose, and glycated hemoglobin. Additionally, acupuncture therapy resulted in a greater decline in the incidence of prediabetes.
The review can thus serve as a prime example for demonstrating how irresponsible research has the power to mislead millions. This is why I have often said that poor research is a danger to public health.
And what can be done about this more and more prevalent problem?
The answer is easy: people need to behave more responsibly; this includes:
- trialists,
- review authors,
- editors,
- peer-reviewers,
- journalists.
Yes, the answer is easy in theory – but the practice is far from it!
I have often called out unreliable or fraudulent research in the realm of Traditional Chinese Medicine (TCM). I think it is important to do so because the abundance of scientific misconduct is such that it has become a danger to public health. Today, I present yet another example:
This recent review claimed to summarize the evidence on TCM in treating MI, the clinical evaluations of TCM in treating male infertility (MI), and the molecular mechanisms of TCM effects. I was alerted to the fact that the authors cite a paper on acupuncture that I had co-authored. Here is the section in question from the review:
Acupuncture is one of the therapeutic techniques that are part of TCM. Acupuncture is a non-invasive technique and is regarded as free of risk if performed by trained personnel [35]. One of the advantages of acupuncture was that the incidence of adverse effects was substantially lower than that of many drugs or other accepted [35]. Acupuncture has been used in the treatment of male and female infertility and in assisted reproductive technology treatments for many years. A total of 100 patients with MI who met the diagnostic criteria were randomly divided into two groups [7]. Half of the patients received acupuncture treatment, and the other half received placebo acupuncture. After 10 weeks treatment, acupuncture successfully improved the indicators of the semen, including the spermatozoa survival rate, b-level activity rate, sperm density, sperm activity rate. A total of 28 infertile patients with severe oligoasthenozoospermia received acupuncture according to the principles of acupuncture and 29 infertile patients received placebo acupuncture. A significantly higher percentage of motile sperm (World Health Organization categories A-C), but no effect on sperm concentration, was found after acupuncture compared with placebo acupuncture [36]. Of the 279 cases of male sterility treated by the combination of acupuncture, pilose antler essence injection to acupoints and oral administration of Chinese materia medica, 142 cases (47.8%) were cured, 81 cases (27.3%) markedly effective, 53 cases (17.8%) effective and 21 cases (7.1%) ineffective [37]. The therapeutic effect of the combination of these three treatments was satisfactory.
Ref 7
Emerging evidence has shown that cell-cell interactions between testicular cells, in particular at the Sertoli cell-cell and Sertoli-germ cell interface, are crucial to support spermatogenesis. The unique ultrastructures that support cell-cell interactions in the testis are the basal ES (ectoplasmic specialization) and the apical ES. The basal ES is found between adjacent Sertoli cells near the basement membrane that also constitute the blood-testis barrier (BTB). The apical ES is restrictively expressed at the Sertoli-spermatid contact site in the apical (adluminal) compartment of the seminiferous epithelium. These ultrastructures are present in both rodent and human testes, but the majority of studies found in the literature were done in rodent testes. As such, our discussion herein, unless otherwise specified, is focused on studies in testes of adult rats. Studies have shown that the testicular cell-cell interactions crucial to support spermatogenesis are mediated through distinctive signaling proteins and pathways, most notably involving FAK, Akt1/2 and Cdc42 GTPase. Thus, manipulation of some of these signaling proteins, such as FAK, through the use of phosphomimetic mutants for overexpression in Sertoli cell epithelium in vitro or in the testis in vivo, making FAK either constitutively active or inactive, we can modify the outcome of spermatogenesis. For instance, using the toxicant-induced Sertoli cell or testis injury in rats as study models, we can either block or rescue toxicant-induced infertility through overexpression of p-FAK-Y397 or p-FAK-Y407 (and their mutants), including the use of specific activator(s) of the involved signaling proteins against pAkt1/2. These findings thus illustrate that a potential therapeutic approach can be developed to manage toxicant-induced male reproductive dysfunction. In this review, we critically evaluate these recent findings, highlighting the direction for future investigations by bringing the laboratory-based research through a translation path to clinical investigations.
This paper does not relate to the statement it is meant to support by the review authors.
Ref 35
The review by Qin et al (1) includes 5 trials none of which should have been included in a quality metaanalysis as the methodology was unconvincing: In the trial by Alraek et al., patients were randomised to receive either acupuncture or no treatment. This means that no attempt was made to control for the effects of placebo or extra attention. Therefore, this study does not demonstrate an effect of acupuncture as the outcome could be due to non-specific effects unrelated with this therapy. By contrast, the trial by Aune et al. did attempt to control for placebo effects by using a sham control group. Sham acupuncture was given using six needles superficially inserted in the calves, thighs or abdomen outside known acupuncture points or meridians. Needles were not manipulated in the sham group. Sham or placebo controls have the purpose of rendering patients unaware of whether they receive the real or the sham treatment. The method used here cannot achieve this aim; patients would be easily able to tell which intervention they received. In other words, this study also did not adequately control for placebo effects. The remaining three trials are all not Medline-listed, authored by Chinese investigators and published in inaccessible journals. This should disqualify them from inclusion as they were unverifiable by the peer review process. According to the published table, they were equivalence trials of acupuncture versus antibiotics with a sample size around 30. This means they are grossly underpowered and thus unable to generate reliable results. Unless BJOG peer reviewers could see the primary articles, or be provided with translations from Chinese, the systematic review should not have been accepted. The “many eyes of science” requires transparency, testing, challenge and verification. Although in the past, inconclusive results of acupuncture have not been thought to be due to Chinese influence (2), it has been noted that virtually all recent published acupuncture trials are “positive” (3), raising questions of publication and other biases. Our colleagues are under tremendous pressure to publish, but we do them no favours by effectively lowering the standard of scientific peer review. Elite journals too have an obligation to train and reiterate about publication ethics and sound scientific writing (4). As none of the primary studies convincingly demonstrated that acupuncture is an effective therapy for recurrent urinary tract infections, no positive conclusion was warranted. Although Qin et al. did state that the risk of bias of the included trials was generally high or unclear (1), the BJOG nevertheless allowed them to turn massive uncertainty into relatively firm, positive conclusions in the abstract (“Acupuncture appeared to be beneficial for treatment and prophylaxis of rUTIs”) and tweetable abstract (“This review found that acupuncture may improve treatment and prevent recurrence of urinary tract infection in women”), thus leading to excited media headlines that inevitably mislead the public. ‘May’ is a weasel word which should be avoided as it is unfalsifiable (for example, pigs do not fly but they ‘may’ fly in the future). The definite, straightforward conclusion must be “There is no good evidence to support the use of acupuncture for the treatment and prophylaxis of recurrent UTIs”. It is not acceptable to give international credibility to an implausible modality that no objective, independent high-quality review has found effective beyond placebo (5). The dampening accompanying mini-commentary (6) does not undo the damage.
The review should be withdrawn while the primary papers are translated for peer reviewers to examine, the above limitations discussed in the text, and the positive ‘spin’ in conclusions corrected. These improvements would consolidate the researchers’ probity and justify the accolade of BJOG publication.
Our letter to the editor does not bear any relation to the statement it is meant to support by the review authors.
Ref 36
In this first prospective, randomized, single-blind, placebo-controlled study, 28 infertile patients with severe oligoasthenozoospermia received acupuncture according to the principles of traditional Chinese medicine (TCM) and 29 infertile patients received placebo acupuncture. A significantly higher percentage of motile sperm (World Health Organization categories A–C), but no effect on sperm concentration, was found after acupuncture compared with placebo acupuncture.
This small study is far from convincing and does not lend itself to far-reaching conclusions
Ref 37
Of the 279 cases of male sterility treated by the combination of acupuncture, pilose antler
essence injection to acupoints and oral administration of Chinese materia medica, 142
cases (47.8%) were cured, 81 cases (27.3%) markedly effective, 53 cases (17.8%) effective
and 21 cases (7.1%) ineffective. The therapeutic effect of the combination of these three
treatments was satisfactory.
This study had no control group and used two different therapies. Therefore, it does not allow any conclusion about the effectiveness of acupuncture.
____________________
Perhaps you feel that these errors are trivial. But I would disagree. The review authors’ praise of acupuncture for MI is misplaced and will mislead the public. There are plenty of reviews on the subject, and those that are not overtly biased arrive at conclusions like these:
- The current evidence on acupuncture for oligoasthenozoospermia is inadequate to draw a solid conclusion due to the poor methodological quality. Rigorous full-scale RCTs are needed to validate the therapeutic efficacy and safety of acupuncture in treating oligoasthenozoospermia.
- The current evidence showing that acupuncture might improve poor semen quality is insufficient because of the small number of studies, inadequacy of procedures and/or insufficient information for semen analysis, high levels of heterogeneity, high risk of bias, and poor quality of reporting. Further large, well-designed RCTs are required.
So, how did this sloppy review come about?
Its authors are affiliated to the TCM Regulating Metabolic Diseases Key Laboratory of Sichuan Province, Hospital of Chengdu University of Traditional Chinese Medicine, Chengdu 610072, China, and the Tea Research Institute, Sichuan Academy of Agricultural Sciences, Chengdu 610066, China. A footnote tells us that their review was supported by the National Natural Science Foundation of China [No. 81973647] and the Xinglin scholar discipline promotion talent program of Chengdu University of traditional Chinese medicine [No. BSH2021018]. This sounds respectable enough.
The journal that published the review is ‘Pharmacological Research – Modern Chinese Medicine‘. Its stated aims are as follows: The journal publishes articles reporting on advances in our comprehension of mechanism and safety in experimental pharmacology and clinical efficacy and safety of pharmacologically active substances, including compound prescriptions, utilized in Traditional Chinese Medicine applying modern scientific research methods. Studies reporting also on the mechanisms of actions of the active substance(s) investigated are encouraged.
The editors in chief of the journal are Guan-Hua Du, PhD, China Academy of Chinese Medical Sciences Institute of Chinese Materia Medica, Beijing, China and Emilio Clementi, M.Mus, MD, PhD, University of Milan, Milan, Italy. No doubt, these are respectable scientists. And because they are, they should make sure that what they publish is correct – a criterion this recent review clearly does not meet.
Bee venom acupuncture (BVA) is a bizarre form of acupuncture where bee venom is applied via a bee sting or an injection into acupuncture points. The paper below starts with the sentence: “BVA is an effective treatment method for various diseases.” This clearly is not true. In fact, there is no convincing evidence that it is effective for any condition. In addition, it can cause serious harm, even life-threatening anaphylaxis.
With this review, Korean authors tried to estimate the incidence rate of anaphylaxis in response to BVA. 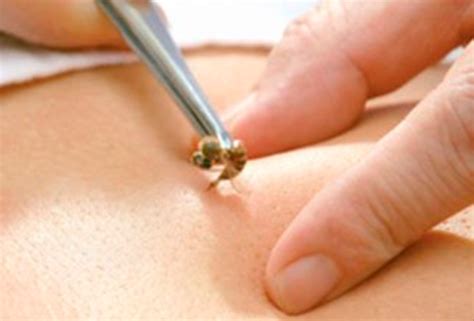
The investigators searched eight databases (MEDLINE (Pubmed), EMBASE, Cochrane Central Register of Controlled, KISS, KMBASE, Koreamed, OASIS, and NDSL) and systematically reviewed the articles that met the inclusion/exclusion criteria.
Among 225 potentially relevant articles, 49 were selected for this study. The overall incidence rate of anaphylaxis in response to BVA was 0.045% (95% CI 0.028-0.062). Women (0.083%, 95% CI 0.010-0.157) showed a higher incidence rate than men (0.019%, 95% CI -0.018 to 0.055), while the incidence for patients who had a skin test conducted (0.041%, 95% CI 0.011-0.072) was not significantly different compared to that obtained for patients for which there was no information about a skin test (0.047%, 95% CI 0.026-0.067). The publication year affected the incidence rate: it was highest before 1999 (1.099%, 95% CI -1.043 to 3.241), lower between 2000 and 2009 (0.049%, 95% CI 0.025-0.073), and lowest between 2010 and 2021 (0.037% 95% CI 0.014-0.060).
The authors concluded that, in this study, we provide reference data about risk size and factors of BVA-related anaphylaxis, which is essentially required for BVA application in clinics.
I fail to understand why this review included only observational studies and RCTs. Why not case reports? We would need a proper post-marketing surveillance system to obtain reliable incidence figures. Yet, such a system does not exist. Therefore, the data generated by this paper are next to worthless.
All this article does, is confirm that anaphylactic reactions after BVA are a reality. As the treatment has not been proven to be effective for any condition, its risk/benefit balance turns out to be negative. In other words, we should therefore not use BVA.
This study used a US nationally representative 11-year sample of office-based visits to physicians from the National Ambulatory Medical Care Survey (NAMCS), to examine a comprehensive list of factors believed to be associated with visits where complementary health approaches were recommended or provided.
NAMCS is a national health care survey designed to collect data on the provision and use of ambulatory medical care services provided by office-based physicians in the United States. Patient medical records were abstracted from a random sample of office-based physician visits. The investigators examined several visit characteristics, including patient demographics, physician specialty, documented health conditions, and reasons for a health visit. They ran chi-square analyses to test bivariate associations between visit factors and whether complementary health approaches were recommended or provided to guide the development of logistic regression models.
Of the 550,114 office visits abstracted, 4.43% contained a report that complementary health approaches were ordered, supplied, administered, or continued. Among complementary health visits, 87% of patient charts mentioned nonvitamin nonmineral dietary supplements. The prevalence of complementary health visits significantly increased from 2% in 2005 to almost 8% in 2015. Returning patient status, survey year, physician specialty and degree, menopause, cardiovascular, and musculoskeletal diagnoses were significantly associated with complementary health visits, as was seeking preventative care or care for a chronic problem.
The authors concluded that these data confirm the growing popularity of complementary health approaches in the United States, provide a baseline for further studies, and inform subsequent investigations of integrative health care.
The authors used the same dataset for a 2nd paper which examined the reasons why office-based physicians do or do not recommend four selected complementary health approaches to their patients in the context of the Andersen Behavioral Model. Descriptive estimates were employed of physician-level data from the 2012 National Ambulatory Medical Care Survey (NAMCS) Physician Induction Interview, a nationally representative survey of office-based physicians (N = 5622, weighted response rate = 59.7%). The endpoints were the reasons for the recommendation or lack thereof to patients for:
- herbs,
- other non-vitamin supplements,
- chiropractic/osteopathic manipulation,
- acupuncture,
- mind-body therapies (including meditation, guided imagery, and progressive relaxation).
Differences by physician sex and medical specialty were described.
For each of the four complementary health approaches, more than half of the physicians who made recommendations indicated that they were influenced by scientific evidence in peer-reviewed journals (ranging from 52.0% for chiropractic/osteopathic manipulation [95% confidence interval, CI = 47.6-56.3] to 71.3% for herbs and other non-vitamin supplements [95% CI = 66.9-75.4]). More than 60% of all physicians recommended each of the four complementary health approaches because of patient requests. A higher percentage of female physicians reported evidence in peer-reviewed journals as a rationale for recommending herbs and non-vitamin supplements or chiropractic/osteopathic manipulation when compared with male physicians (herbs and non-vitamin supplements: 78.8% [95% CI = 72.4-84.3] vs. 66.6% [95% CI = 60.8-72.2]; chiropractic/osteopathic manipulation: 62.3% [95% CI = 54.7-69.4] vs. 47.5% [95% CI = 42.3-52.7]).
For each of the four complementary health approaches, a lack of perceived benefit was the most frequently reported reason by both sexes for not recommending. Lack of information sources was reported more often by female versus male physicians as a reason to not recommend herbs and non-vitamin supplements (31.4% [95% CI = 26.8-36.3] vs. 23.4% [95% CI = 21.0-25.9]).
The authors concluded that there are limited nationally representative data on the reasons as to why office-based physicians decide to recommend complementary health approaches to patients. Developing a more nuanced understanding of influencing factors in physicians’ decision making regarding complementary health approaches may better inform researchers and educators, and aid physicians in making evidence-based recommendations for patients.
I am not sure what these papers really offer in terms of information that is not obvious or that makes a meaningful contribution to progress. It almost seems that, because the data of such surveys are available, such analyses get done and published. The far better reason for doing research is, of course, the desire to answer a burning and relevant research question.
A problem then arises when researchers, who perceive the use of so-called alternative medicine (SCAM) as a fundamentally good thing, write a paper that smells more of SCAM promotion than meaningful science. Having said that, I find it encouraging to read in the two papers that
- the prevalence of SCAM remains quite low,
- more than 60% of all physicians recommended SCAM not because they were convinced of its value but because of patient requests,
- the lack of perceived benefit was the most frequently reported reason for not recommending it.
Acupuncture is often promoted as a therapeutic option for obesity and weight control. The aim of this study was to investigate the effects of electroacupuncture (EA) on body weight, body mass index (BMI), skin fold thickness, waist circumference and skin temperature of the abdominal region in non-obese women with excessive abdominal subcutaneous fat.
A total of 50 women with excessive abdominal subcutaneous fat (and average BMI of 22) were randomly assigned to one of two groups:
- an EA group (n = 25) receiving 10 EA sessions (insertion of needles connected to an electrical stimulator at a frequency of 40 Hz for 40 min),
- a control group (n = 25) that received no treatment.
Outcome measures evaluated included waist circumference, supra-iliac and abdominal skinfolds, body composition and superficial skin temperature (measured by cutaneous thermography) before and after treatment.
Compared with the untreated group, women in the EA group exhibited decreased supra-iliac and abdominal skin folds (p < 0.001), waist circumference (p < 0.001), percentage body fat (p = 0.001) and percentage abdominal fat (p < 0.001). In addition, the EA group showed an elevated skin temperature at the site of the treatment. However, EA did not significantly impact body weight (p = 0.01) or BMI (p = 0.2).
The authors concluded that EA promoted a reduction in abdominal waist circumference, supra-iliac and abdominal skin folds, and percentage body and abdominal fat in women of normal BMI with excessive abdominal subcutaneous fat, as well as an increase in the superficial skin temperature of the abdominal region.
If we did not know that acupuncture researchers were all honest investigators testing hypotheses the best they can, we could almost assume that some are trying to fool us. The set-up of this study is ideally suited to introduce a proper placebo treatment. All one has to do is to not switch on the electrical stimulator in the control group. Why did the researchers not do that? Surely not because they wanted to increase the chances of generating a positive result; that would have been dishonest!!!
So, as it stands, what does the study tell us? I think it shows that, compared to patients who receive no treatment, patients who do receive the ritual of EA are better motivated to adhere to calorie restrictions and dietary advice. Thus, I suggest to re-phrase the conclusions of this trial as follows:
The extra attention of the EA treatment motivated obese patients to eat less which caused a reduction in abdominal waist circumference, supra-iliac and abdominal skin folds, and percentage body and abdominal fat in women of normal BMI with excessive abdominal subcutaneous fat.
This meta-analysis was conducted by researchers affiliated to the Evangelical Clinics Essen-Mitte, Department of Internal and Integrative Medicine, Faculty of Medicine, University of Duisburg-Essen, Germany. (one of its authors is an early member of my ALTERNATIVE MEDICINE HALL OF FAME). The paper assessed the safety of acupuncture in oncological patients.
The PubMed, Cochrane Central Register of Controlled Trials, and Scopus databases were searched from their inception to August 7, 2020. Randomized controlled trials in oncological patients comparing invasive acupuncture with sham acupuncture, treatment as usual (TAU), or any other active control were eligible. Two reviewers independently extracted data on study characteristics and adverse events (AEs). Risk of bias was assessed using the Cochrane Risk of Bias Tool.
Of 4590 screened articles, 65 were included in the analyses. The authors observed that acupuncture was not associated with an increased risk of intervention-related AEs, nonserious AEs, serious AEs, or dropout because of AEs compared with sham acupuncture and active control. Compared with TAU, acupuncture was not associated with an increased risk of intervention-related AEs, serious AEs, or dropout because of AEs but was associated with an increased risk for nonserious AEs (odds ratio, 3.94; 95% confidence interval, 1.16-13.35; P = .03). However, the increased risk of nonserious AEs compared with TAU was not robust against selection bias. The meta-analyses may have been biased because of the insufficient reporting of AEs in the original randomized controlled trials.
The authors concluded that the current review indicates that acupuncture is as safe as sham acupuncture and active controls in oncological patients. The authors recommend researchers heed the CONSORT (Consolidated Standards of Reporting Trials) safety and harm extension for reporting to capture the side effects and better investigate the risk profile of acupuncture in oncology.
You might think this article is not too bad. So, why do I feel that this paper is so bad?
One reason is that the authors included evidence up to August 2020. Since then, there must have been hundreds of further papers on acupuncture. The article was therefore out of date before it was published.
But that is by no means my main reason. We know from numerous investigations that acupuncture studies often fail to report AEs (and thus violate publication ethics). This means that this new analysis is merely an amplification of the under-reporting. It is, in other words, a means of perpetuating a wrong message.
Yes, you might say, but the authors acknowledge this; they even state in the abstract that “The meta-analyses may have been biased because of the insufficient reporting of AEs in the original randomized controlled trials.” True, but this fact does not erase the mistake, it merely concedes it. At the very minimum, the authors should have phrased their conclusion differently, e.g.: the current review confirms that AEs of acupuncture are under-reported in RCTs. Therefore, a meta-analysis of RCTs is unable to verify whether acupuncture is safe. From other types of research, we know that it can cause serious AEs.
An even better solution would have been to abandon or modify the research project when they first came across the mountain of evidence showing that RCTs often fail to mention AEs.
As it stands, the conclusion that acupuncture is as safe as sham acupuncture is simply not true. Since the article probably looks sound to naive readers, I feel that is a particularly good candidate for the WORST PAPER OF 2022 COMPETITION.
PS
For those who are interested, here are 4 of my own peer-reviewed articles on the safety of acupuncture (much more can, of course, be found on this blog):
- Patient safety incidents from acupuncture treatments: a review of reports to the National Patient Safety Agency – PubMed (nih.gov)
- Acupuncture–a critical analysis – PubMed (nih.gov)
- Prospective studies of the safety of acupuncture: a systematic review – PubMed (nih.gov)
- The risks of acupuncture – PubMed (nih.gov)

